No products in the cart.
Travaxal, eye drops 0.04 mg/ml 2.5ml
€1.00
Out of stock
(E-mail when Stock is available)
Description
Pharmacotherapeutic group: Antiglaucoma agent – synthetic prostaglandin F2-alpha analogue.
ATX code: S01EE04
Pharmacological properties
Indications
Indications
Reducing elevated intraocular pressure in:
– open-angle glaucoma;
– elevated intraocular pressure.
Active ingredient
Active ingredient
Travoprost
Composition
Composition
1 ml of the drug contains:
Active ingredient:
Travoprost – 004 mg,
Excipients:
Mannitol – 46.0 mg,
Macrogol glyceryl hydroxystearate – 5.0 mg,
Boric acid – 3,0 mg,
Tromethamol – 1,2 mg,
Benzalkonium chloride – 0,015 mg,
Dinatrium edetate dihydrate (Trilon B) – 0.1 mg,
8 M sodium hydroxide solution or
8 M hydrochloric acid solution – to pH 5.5-7.0,
Water for injection – up to 1.0 ml.
How to take, the dosage
How to take, the dosage
Topically.
1 drop into the conjunctival sac of the eye (eye) once a day, in the evening. To reduce the risk of systemic side effects, it is recommended that after instillation of the drug the nasolacrimal duct be compressed by pressing on its projection area at the inner corner of the eye.
If a dose of the drug is missed, treatment should be continued with the next dose. The daily dose of the drug should not exceed 1 drop in the conjunctival sac of the eye once a day.
The drug may be used in combination with other local ophthalmic drugs to reduce intraocular pressure. In this case, the interval between their administration should be at least 5 minutes.
If the drug is prescribed as a substitute for another ophthalmic glaucoma drug, the latter should be discontinued and Travaxal started the next day.
Principle procedure:
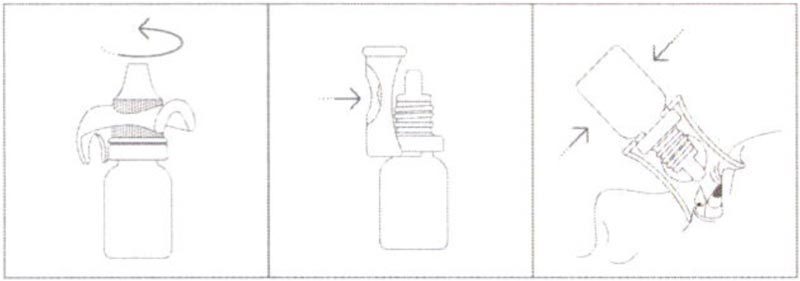

- Remove the stop and the bottle from the pack.
- Open the bottle with the stopper.
- Place eyelid stopper against eyeball, drip in desired amount.
- Remove stopper from neck of bottle.
Close bottle with lid.
.
Special Instructions
Special Instructions
The drug may cause a gradual change in eye color by increasing the number of melanosomes (pigment granules) in the melanocytes. This effect is mainly seen in patients with mixed iris coloration such as blue-brown, gray-brown, green-brown, or yellow-brown. This effect has also been noted in patients with brown iris coloration. The brown pigmentation usually spreads concentrically around the pupil to the periphery of the iris of the eye, with all or part of the iris becoming more intense brown. The long-term effects on melanocytes and the consequences are currently unknown. Changes in iris color occur slowly and may go undetected for months or years. Patients should be informed of the possibility of irreversible changes in eye color before starting treatment. If only one eye is treated, persistent heterochromia may develop. No further increase in brown iris pigmentation was noted after the end of therapy with travoprost.
Darkening of the eyelid skin and/or periorbital area has been reported in 0.4% of patients due to the use of travoprost.
Travoprost can gradually change the lash structure of the eye on which it is used; during clinical trials, such changes were observed in approximately half of patients and included increases in lash length, thickness, pigmentation, and number of lashes. The mechanism of change in lash structure and the long-term effects of this action are currently unknown.
There is no experience with travoprost in inflammatory eye disease, neovascular glaucoma, closed angle glaucoma, narrow angle glaucoma or congenital glaucoma, and only limited experience with eye disease caused by thyroid disorders, in glaucoma in patients with pseudophakia. in pigmentary or pseudoexfoliative glaucoma.
The drug is recommended with caution in patients with aphakia, pseudophakia, posterior lens capsule rupture, with risk factors for cystoid macular edema.
Contact of travoprost with the skin should be avoided because studies in rabbits have shown transdermal absorption of travoprost.
Patients with risk factors for iritis/veitis should be cautiously prescribed.
Patients should remove contact lenses before injecting the drug. Wait 15 minutes after insertion before reinserting contact lenses.
Influence on driving and operating machinery
Transient blurred vision or other visual disturbances after use of the drug may affect the ability to operate vehicles and machinery. If blurred vision occurs after injecting the drug, the patient must wait until visual clarity is restored before driving motor vehicles and operating machinery.
Contraindications
Contraindications
Hypersensitivity to the components of the drug, children under 18 years of age, pregnancy and breast-feeding.
Cautions
The drug should be used with caution in patients with aphakia; in patients with pseudophakia when the posterior lens capsule has ruptured or in patients with an anterior chamber intraocular lens; in patients at risk of cystoid macular edema.
The drug should be used with caution in patients with acute inflammation of the visual organ and in patients with risk factors predisposing to iritis, uveitis.
Side effects
Side effects
The overall profile of adverse reactions according to clinical studies showed that conjunctival injection and iris hyperpigmentation were the most common adverse events, with an incidence of 20 and 6%, respectively.
The adverse reactions detected during post-registration use of the drug were classified as follows: Very common (≥1/10); common (≥1/100 and < 1/10); infrequent (≥1/1000 and < 1/100); rare (≥1/10000 and < 1/1000); very rare (< 1/10000) and frequency unknown (cannot be estimated from available data). In each group, adverse events are presented in decreasing order of severity. Adverse events are reported in clinical trials and post-registration follow-up.
| System-organ class | Frequency of occurrence | Undesirable | ||||
| Infectious and parasitic diseases | Rarely | Infectious eye lesion caused by Herpes simplex, herpetic keratitis < | ||||
| Immune system disorders | Infrequent | Hypersensitivity, seasonal allergies | ||||
| Mental disorders | With unknown frequency | Depression, anxiety, insomnia | ||||
| Nervous system disorders | Infrequent | Headache, dizziness, loss of visual fields | ||||
| Rarely | Dysgeusia | |||||
| Visual organ disturbances | Very often | Conjunctival injection | ||||
| Often | Hyperpigmentation of the iris, pain in the eye, discomfort in the eye, dry eye syndrome, itching in the eye, eye irritation | |||||
| Infrequent | Corneal erosion, uveitis, iritis, keratitis, pitting keratitis, photophobia, blepharitis, ocular discharge, eyelid erythema, periorbital edema, itchy eyelids, decreased visual acuity, blurred vision, lacrimation, conjunctivitis, ectropion, cataracts, crusts on the edges of the eyelids, increased lash growth, discolored lashes, asthenopia, anterior chamber inflammation | Entertainment/td> | ||||
| Rarely | Photopsia, eyelid eczema, conjunctival edema, iridescent circles around light sources, conjunctival folliculosis, ocular hypoesthesia, meibomianitis, pigment dispersion in the anterior chamber, mydriasis, thickened eyelashes, trichiasis, iridocyclitis, inflammation of the eye | |||||
| Inflammatory eye/td> | ||||||
| With unknown frequency | Macular edema, sunken eyeballs | |||||
| Hearing and labyrinth disorders | With unknown frequency | Vertigo, tinnitus | ||||
| Heart disturbances | Infrequent | Feeling of palpitations | ||||
| Rarely | Irregular heartbeat, decreased heart rate | |||||
| With unknown frequency | Chest pain, bradycardia, tachycardia, arrhythmia | |||||
| Vascular disorders | Rarely | Decreased diastolic blood pressure, increased systolic blood pressure, hypotension, hypertension | ||||
| Respiratory system, thoracic and mediastinal organ disorders | Non-diastolic/td> | Infrequent | Dyspnea, asthma, nasal congestion, throat irritation | |||
| Rarely | Impaired respiratory function, oropharyngeal pain, cough, dysphonia, allergic rhinitis | |||||
| With unknown frequency | Worsening course of bronchial asthma, nasal bleeding | |||||
| Gastrointestinal disorders | Rarely | Constipation, dry mouth, gastric ulcer exacerbation, gastrointestinal disturbances | ||||
| With unknown frequency | Diarrhea, abdominal pain, nausea, vomiting | |||||
| Skin and subcutaneous fatty tissue disorders | Infrequent | Augmentation of skin pigmentation in the periorbital area, skin discoloration, changes in the structure of downy hair, hypertrichosis | ||||
| Rarely | Allergic dermatitis, contact dermatitis, erythema, rash, discoloration of downy hair, madarosis | |||||
| Allergic dermatitis, contact dermatitis, erythema, rash, discoloration of downy hair/td> | ||||||
| With unknown frequency | Itching, abnormal growth of downy hair | |||||
| Musculoskeletal and connective tissue disorders | Rarely | Musculoskeletal pain | ||||
| With unknown frequency | Arthralgia | |||||
| Renal and urinary system disorders | With unknown frequency | Dysuria, urinary incontinence | ||||
| General disorders | Rarely | Asthenia | ||||
| Laboratory abnormalities | With unknown frequency | Elevation of total specific prostatic antigen |
Adverse Event Profile in Pediatric Practice
In a 3-month phase 3 study and a 7-day pharmacokinetic study involving 102 pediatric patients, the adverse event profile was consistent with that of adult patients. Short-term safety profiles in different subpopulations of the pediatric population were also similar.
The most common adverse reactions in the pediatric population were conjunctival injection (16.9%) and increased eyelash growth (6.5%). In a similar 3-month study in adult patients, these adverse events occurred at rates of 11.4% and 0.0%, respectively. Additionally, in the pediatric population (n=77), a 3-month clinical trial similar to the one in adults (n=185) reported single cases of eyelid erythema, keratitis, lacrimation, and photophobia with an overall adverse event rate of 1.3% compared to 0.0% in the adult population.
Overdose
Overdose
Overdose toxicity by local administration is unlikely. Treatment in case of accidental ingestion is symptomatic and supportive.
In case of local overdose the drug should be flushed out the eyes with warm water.
Pregnancy use
Pregnancy use
Pregnancy
There are no or limited data on the use of hervoprost in pregnant women. Animal studies with hervoprost have shown reproductive toxicity. Women during pregnancy, as well as women planning to become pregnant, should refrain from direct contact with substances containing prostaglandins. Prostaglandins and prostaglandin analogues are biologically active substances that can be absorbed through the skin.
Women during pregnancy, as well as women planning pregnancy should use appropriate precautions to avoid direct contact of the contents of the vial on the skin. If a significant portion of the contents of the bottle does get on the skin (which is unlikely), the area of skin on which the drug got, should be immediately rinsed with water.
Breastfeeding
There is no data on whether hervoprost and/or metabolites penetrate into breast milk.
Fertility
No studies have been conducted to evaluate the effects of hervoprost on human fertility. Animal studies have shown that there is no effect of hervoprost on fertility when the drug is used in doses greater than 250 times the maximum recommended dose for humans.
Similarities
Similarities
Travatan, Travapress, Travoprost-Optic
Additional information
| Weight | 0.010 kg |
|---|---|
| Shelf life | 3 years. After opening the bottle – 1 month. Do not use after the expiration date! |
| Conditions of storage | At 2 to 8 ° C. Opened bottle should be stored at a temperature not exceeding 25 ° C. Keep out of reach of children. |
| Manufacturer | Grotex Ltd, Russia |
| Medication form | eye drops |
| Brand | Grotex Ltd |
Related products
Buy Travaxal, eye drops 0.04 mg/ml 2.5ml with delivery to USA, UK, Europe and over 120 other countries.