No products in the cart.
Glucose, 5% 500 ml
€1.00
Out of stock
(E-mail when Stock is available)
Description
Glucose increases redox processes in the body, improves antitoxic function of the liver, enhances myocardial contractile activity, and is a source of easily digestible carbohydrates.
The pharmacodynamic properties of 5%, 10% and 20% solutions of dextrose are similar to those of glucose, the main source of energy of cellular metabolism.
The 5% solution of dextrose is an isotonic solution with an osmolarity of about 278 mOsm/L. The caloric intake of 5% dextrose solution is 200 kcal/L,
10% dextrose solution is a hypertonic solution with an osmolarity of about 555 mOsm/L. The caloric intake of a 10% dextrose solution is 400 kcal/L.
The 20% dextrose solution is a hypertonic solution with an osmolarity of approximately 1110 mOsm/L. The caloric intake of a 20% dextrose solution is 680 kcal/L.
In parenteral nutrition 5%, 10% and 20% solutions of dextrose are administered as a source of carbohydrates (alone or as part of parenteral nutrition if necessary).
The 5% and 10% solutions of dextrose allow replenishment of fluid deficiencies without simultaneous administration of ions.
The 20% dextrose solution provides the maximum amount of calories in the minimum amount of fluid.
Dextrose entering the tissues is phosphorylated into glucose-6-phosphate, which is actively involved in many parts of the body’s metabolism.
When dextrose solutions are used to dilute and dissolve parenterally administered medications, the pharmacodynamic properties of the solution will depend on the substance added.
Pharmacokinetics:
Glucose is metabolized by two different pathways: anaerobic and aerobic.
Dextrose breaks down into pyruvic acid or lactic acid (anaerobic glycolysis) and is metabolized to carbon dioxide and water with the release of energy.
When using dextrose solution to dilute and dissolve parenterally administered medications, the pharmacokinetic properties of the solution will depend on the substance added.
Indications
Indications
5% glucose solution:
– as a source of carbohydrates (alone or as part of parenteral nutrition if necessary);
– for rehydration in case of fluid loss, especially in patients with a high carbohydrate requirement;
– for dilution and dissolution of parenterally administered medications.
Active ingredient
Active ingredient
Composition
Composition
Per 1 liter:
active ingredients:
dextrose (glucose) monohydrate in terms of dextrose 50 g/100 g/200 g;
excipients:
Sodium chloride 0.26 g, 0.1 M hydrochloric acid solution to pH 3.0-4.5,
water for injection to 1.0 L.
Theoretical osmolarity, mOsmol/L – 277/555/1110.
How to take, the dosage
How to take, the dosage
In an intravenous (IV) drip. The drug is usually injected into a peripheral or central vein.
The concentration and dose of the administered solution depends on the patient’s age, body weight and clinical condition.
The use of the drug should be under regular medical supervision.
Clinical and biologic parameters such as blood glucose concentration and fluid-salt balance should be monitored closely.
The dosing regimen of glucose solution for infusion is 5%
The recommended dose is as a source of carbohydrates (alone or as part of parenteral nutrition if necessary):
For adults:
– 500-3000 ml per day.
For children, including newborns:
– with a body weight of 0-10 kg – 100 ml/kg per day;
– with a body weight of 10-20 kg – 1000 ml + additional 50 ml for each kg of body weight over 10 kg per day;
– with a body weight over 20 kg – 1500 ml + additional 20 ml for each kg of body weight over 20 kg per day.
The rate and volume of infusion depend on the patient’s age, body weight, clinical condition and metabolism, as well as on concomitant therapy. In children, these should be determined by the attending physician who has experience with the use of intravenous medications in this patient population.
The threshold of glucose utilization in the body should not be exceeded to avoid hyperglycemia, so the maximum dose of dextrose varies from 5 mg/kg/min for adults and 10-18 mg/kg/min for infants and children depending on age and total body weight.
The recommended dose when used to dilute and dissolve parenterally administered medications is usually 50-250 ml per dose of medication administered, but the required volume should be determined based on the instructions for use of the medication being added. In this case, the dose and rate of solution administration are determined by the properties and dosing regimen of the diluted drug.
Interaction
Interaction
The co-administration of catecholamines and steroids decreases dextrose (glucose) absorption.
Mixing with other medications should be visually monitored for compatibility.
To dilute or dissolve other medications, the drug should only be used if there are instructions for dilution with dextrose solution in the instructions for use for the medication.
In the absence of information on compatibility, the drug should not be mixed with other medicinal products.
Be sure that any medication is soluble and stable in water within the pH range of the medication before adding it.
After adding a compatible medication to the product, the resulting solution should be administered immediately.
Drugs with known incompatibilities should not be used.
If dextrose solutions are administered through the same infusion system as for hemotransfusion, there may be a risk of hemolysis and thrombosis.
Special Instructions
Special Instructions
Since patients with diabetes mellitus, renal insufficiency or those in acute critical condition may have impaired glucose (dextrose) tolerance, their clinical and biological parameters, in particular plasma electrolyte concentration, including magnesium or phosphorus, blood glucose concentration should be monitored particularly carefully. If hyperglycemia is present, the rate of drug administration should be adjusted or short-acting insulin should be prescribed. Usually glucose is completely absorbed by the body (normally the kidneys do not excrete it), so the appearance of glucose in the urine may be a pathological sign.
In case of prolonged or high-dose dextrose administration it is necessary to monitor the concentration of potassium in plasma and if necessary to administer additional potassium to avoid hypokalemia.
In episodes of intracranial hypertension, careful monitoring of blood glucose concentration is necessary.
The use of dextrose solutions may lead to hyperglycemia. Therefore, they are not recommended after acute ischemic stroke, because hyperglycemia is associated with increased ischemic brain damage and prevents recovery.
Particular close clinical monitoring is required at the beginning of intravenous administration of the drug.
For rehydration therapy, carbohydrate solutions should be used in combination with electrolyte solutions to avoid electrolyte imbalance (hyponatremia, hypokalemia).
The concentration of glucose and electrolytes in the blood, the water balance and the acid-base state of the body should be monitored.
The solution should be inspected before use. Use only a clear solution without visible inclusions and with no damage to the package. Administer directly after connection to the infusion system.
The solution should be administered using sterile equipment and following aseptic and antiseptic procedures.
The air should be removed from the infusion system with the solution to prevent air embolism.
Do not connect containers in series to avoid air embolism, which can occur due to air being sucked out of the first container before the second container has completed the infusion.
The administration of intravenous solutions contained in soft plastic containers under increased pressure to increase the flow rate can cause an air embolism if the residual air in the container is not completely removed prior to injection.
The use of an intravenous system with a vent may cause an air embolism if the vent is open. Soft plastic containers should not be used with these systems.
Added agents may be administered prior to infusion or during infusion through the infusion site (if a dedicated drug entry port is available).
Addition of other medications to the solution or violation of the administration technique may cause fever due to possible exposure to pyrogens.
If adverse reactions develop, the infusion should be stopped immediately.
If other drugs are added before parenteral administration, the isotonicity of the resulting solution should be checked.
The complete and thorough mixing under aseptic conditions is mandatory.
The solutions containing additional substances should be used immediately and storage is prohibited.
If additional nutrients are administered, the osmolarity of the resulting mixture should be determined prior to infusion.
The resulting mixture should be administered through a central or peripheral venous catheter depending on the final osmolarity.
The compatibility of additionally administered medications should be evaluated prior to their addition to the solution (similar to the use of other parenteral solutions). It is the physician’s responsibility to evaluate the compatibility of additionally administered drugs with the drug. The resulting solution should be checked for discoloration and/or the appearance of precipitate, insoluble complexes or crystals. The instructions for use of the drugs to be added should be studied.
From a microbiological point of view, the diluted drug should be used immediately. The exception is dilutions prepared under controlled and aseptic conditions. Otherwise, once the solution has been prepared, the timing and conditions of storage prior to administration are the responsibility of the user.
Children
In newborns, especially those born prematurely or with low birth weight, there is an increased risk of hypo- or hyperglycemia, so careful monitoring of blood glucose concentrations during intravenous administration of dextrose solutions is necessary to avoid long-term adverse effects. Hypoglycemia in newborns may lead to prolonged seizures, coma and brain damage. Hyperglycemia is associated with intraventricular hemorrhage, delayed bacterial and fungal infections, retinopathy of prematurity, necrotizing enterocolitis, bronchopulmonary dysplasia, prolonged hospitalization and mortality.
In order to avoid a potentially fatal overdose of intravenous drugs in newborns, special attention must be paid to the route of administration. For the treatment of “symptomatic” hypoglycemia, a 10% glucose solution is preferred. At the same time it is necessary to constantly monitor the blood glucose level and adjust it if necessary. It should be taken into account that newborns with different pathologies have different requirements for exogenous glucose. Abrupt cessation of infusion may cause hypoglycemia, so the dose of glucose is reduced gradually, stop titrating the glucose solution when the child remains normoglycemic when glucose is injected at a rate of 4 mg/kg/min.
When a syringe pump is used for intravenous drug administration to newborns, the solution container should not be left attached to the syringe.
If an infusion pump is used, all system clamps must be closed before removing the system from the pump or disconnecting it, regardless of any device in the system that prevents free fluid flow.
Intravenous infusion devices and other drug administration equipment should be monitored regularly.
If the product contains corn-derived dextrose, it is contraindicated in patients with known intolerance to corn or corn products because of possible following hypersensitivity symptoms: anaphylactic reactions, chills, and fever.
For preparations in containers:
The containers should be disposed of after a single use.
Dispose of each unused dose.
Do not recombine partially used containers.
Impact on the ability to drive:
Not applicable (due to inpatient use of the drug only).
Contraindications
Contraindications
Decompensated diabetes mellitus and non-sugar diabetes; hyperosmolar coma; hemodilution and extracellular hyperhydration or hypervolemia; hyperglycemia and hyperlactatemia: Severe renal failure (with oliguria or anuria); uncompensated heart failure; generalized edema (including pulmonary and cerebral edema) and cirrhosis of the liver with ascites; other known forms of glucose intolerance (such as metabolic stress); hypersensitivity to the drug components; administration of the solution within the first 24 h after head trauma; use of the same infusion system as for hemotransfusion because of risk of hemolysis and thrombosis; patients with known intolerance to corn or corn products (when receiving dextrose from corn); contraindications to any drugs added to glucose solution.
With caution:
Diabetes mellitus, intracranial hypertension, hyponatremia, pediatric age.
Side effects
Side effects
Adverse reactions (ARs) are grouped by system and organ according to the MedDRA Dictionary and the WHO Frequency Classification of HP:
Very common (⥠1/10)
Frequent (⥠1/100 to < 1/10)
/p>
Not often (⥠1/1000 to < 1/100)
Rarely (⥠1/10000 to < 1/1000)
Very rarely (< 1/10000)
Frequency unknown – (frequency cannot be determined from available data).
Immune system disorders
Frequency unknown: anaphylactic reactions, hypersensitivity.
Metabolism and nutrition disorders
Prevalence unknown: disorders of water-electrolyte balance (hypokalemia, hypomagnesemia and hypophosphatemia), hyperglycemia, hemodilution, dehydration, hypervolemia.
Cardiac disorders
Prevalence unknown: acute left ventricular failure.
Vascular disorders
Prevalence unknown: venous thrombosis, phlebitis.
Skin and subcutaneous tissue disorders
Prevalence unknown: increased sweating.
Renal and urinary tract disorders
Prevalence unknown: polyuria.
General disorders and disorders at the injection site
Prevalence unknown: chills, fever, infection at the injection site, irritation at the injection site, extravasation, soreness at the injection site.
Laboratory and instrumental data
Prevalence unknown: glucosuria,
The undesirable reactions may be related to the drug that was added to the solution. The likelihood of other adverse reactions depends on the properties of the specific drug added.
If adverse reactions occur, the administration of the solution should be discontinued, the patient’s condition should be evaluated, and adequate measures should be taken.
Overdose
Overdose
Symptoms: Prolonged infusion of the drug can lead to hyperglycemia, glucosuria, hyperosmolarity, osmotic diuresis, and dehydration. Rapid infusion may create fluid accumulation in the body with hemodilution and hypervolemia, and if the body’s ability to oxidize glucose is increased, rapid administration may cause hyperglycemia. There may also be a decrease in plasma potassium and inorganic phosphate.
When dextrose infusion solution is used to dilute and dissolve other medications for intravenous administration, clinical signs and symptoms of overdose may be related to the properties of the medications used.
Treatment: If symptoms of overdose occur, suspend administration of the solution, assess the patient’s condition, administer short-acting insulin, and administer supportive symptomatic therapy if necessary.
Similarities
Similarities
Additional information
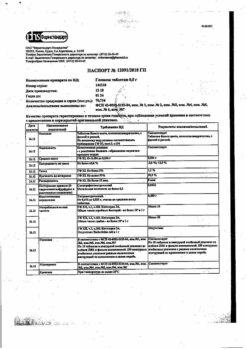
| Weight | 0.556 kg |
|---|---|
| Shelf life | 2 years. |
| Conditions of storage | In a dry place at a temperature of 5 to 30 ° C. Store out of reach of children. Freezing of the drug is allowed as long as the container remains airtight. |
| Manufacturer | Hematec, Russia |
| Medication form | solution for infusion |
| Brand | Hematec |
Other forms…
Related products
Buy Glucose, 5% 500 ml with delivery to USA, UK, Europe and over 120 other countries.