No products in the cart.
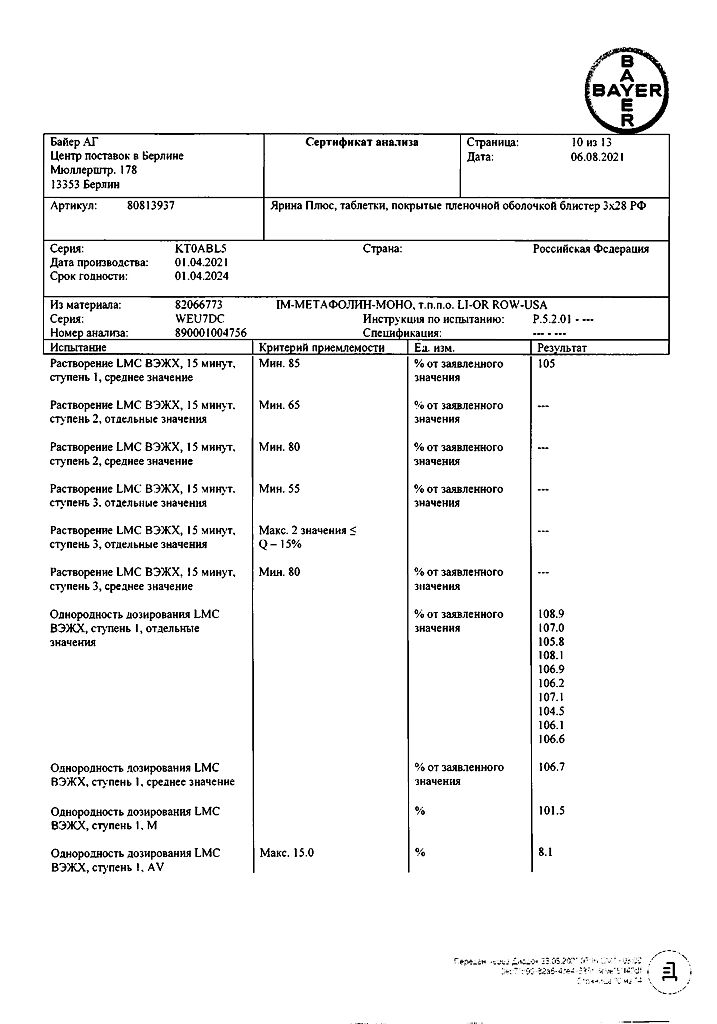
Yarina Plus, 84 pcs.
€94.85 €79.04
EAN: 4029668001712
SKU: 216545
Categories: Contraceptive, Gynecology and Obstetrics, Hormonal, Medicine
Description
Yarina®Plus is a low-dose monophasic combined estrogen/gestagen contraceptive consisting of hormone tablets and adjunctive tablets containing calcium levomepolate.
The contraceptive effect of Yarina®Plus is mainly due to suppression of ovulation and increased cervical secretion viscosity.
In women taking combined oral contraceptives (OCs), the cycle becomes more regular, pain, intensity and duration of menstrual bleeding decrease, and as a result the risk of iron deficiency anemia decreases. There is also evidence of a decreased risk of endometrial and ovarian cancer.
Two post-registration studies were conducted to assess the risk of VTE with Yarin® (ethinylestradiol/drospirenone at doses of 0.03 mg/3 mg). The first prospective observational study showed that the incidence of VTE in women using Yarina®, with or without other VTE risk factors, was in the same range as for women using levonorgestrel and other OCs. A second prospective controlled database study comparing women using Yarin® with women using other OCs also confirmed similar rates of VTE among all cohorts of women.
Drospirenone in Yarina® Plus has antimineralocorticoid activity and helps prevent hormone-dependent fluid retention, which may be seen in weight loss and decreased likelihood of peripheral edema.
Drospirenone also has anti-androgenic activity and helps to reduce acne (acne), oily skin and hair (seborrhea). These features of drospirenone should be considered when choosing a contraceptive for women with hormone-dependent fluid retention, as well as women with acne and seborrhea. In its characteristics drospirenone is similar to natural progesterone produced by the female body.
When the drug is used correctly, the Perl index (a measure of the number of pregnancies in 100 women using the contraceptive in a year) is less than 1. If the pill is missed or used incorrectly, the Perl Index may increase.
The acidic form of calcium levomepholate is identical in structure to naturally occurring L- 5-methyltetrahydrofolate (L-5-methyl-THF), the major folate form found in food. The average plasma concentration of L-5-methyltetrahydrofolate in people who do not use foods fortified with folic acid is about 15 nmol/L.
Levomefolate, unlike folic acid, is a biologically active form of folate. Because of this it is absorbed better than folic acid. Levomefolate is indicated to meet the increased demand and to ensure the necessary content of folate in women during pregnancy and during breastfeeding.
The introduction of calcium levomepholate as part of an oral contraceptive reduces the risk of fetal neural tube defects if a woman becomes pregnant immediately after discontinuation of contraception (or, in very rare cases, when using oral contraception).
Indications
Indications
Contraception
- Contraception designed primarily for women with symptoms of hormone-dependent fluid retention.
- Contraception and treatment of moderate acne (acne vulgaris).
- Contraception in women with folate deficiency.
.
Composition
Composition
Permicidal film-coated tablets (active combined)
1 tablet contains:
active ingredients:
ethinylestradiol (micronized, in the form of betadex clathrate) 30 mcg,
drospirenone (micronized) 3 mg,
calcium levomepholate (micronized) 451 µg
excipients:
Lactose monohydrate – 45.319 mg,
microcrystalline cellulose – 24.8 mg,
croscarmellose sodium – 3.2 mg,
Hyprolose (5 cP) – 1.6 mg,
Magnesium stearate – 1.6 mg.
coating composition:
orange varnish – 2 mg or (alternatively):
Hypromellose (5 cP) – 1.0112 mg,
Macrogol 6000 – 202.4 µg,
talc – 202.4 µg,
titanium dioxide – 527.1 µg,
iron oxide yellow dye – 44.6 µg,
iron oxide red dye – 12.3 µg.
Pills, film-coated (auxiliary vitamin)
1 tablet contains:
active ingredients:
calcium levomepholate (micronized) 451 mg
excipients:
Lactose monohydrate – 48.349 mg,
microcrystalline cellulose – 24.8 mg,
croscarmellose sodium – 3.2 mg,
Hyprolose (5 cP) – 1.6 mg,
Magnesium stearate – 1.6 mg.
coating composition:
light orange varnish – 2 mg or (alternatively):
Hypromellose (5 cP) – 1.0112 mg,
Macrogol 6000 – 202.4 µg,
talc – 202.4 µg,
titanium dioxide – 572.3 µg,
iron oxide yellow dye – 8.9 µg,
iron oxide red dye – 2.8 µg.
.
How to take, the dosage
How to take, the dosage
The tablets should be taken orally in the order listed on the package, every day at the same time, without chewing, with a small amount of water. Take 1 tablet / day continuously for 28 days. The tablets in the next pack should be taken as soon as the previous pack is finished.
Bleeding withdrawal usually begins 2 to 3 days after starting the inactive pills and may not end before taking the pills from the next package.
The package of Yarina® Plus includes 1 or 3 blisters that contain 21 active tablets and 7 adjunct tablets (last row). The package also includes a calendar of seven self-adhesive strips with the names of the days of the week marked on them. You need to choose the strip with the first day of the week when you start taking the pills. For example, if you have pills that start on a Wednesday, use the strip that starts with “Wed.
The strip should be placed along the top of the package, so the first day is above the pill with the arrow that says “Start. This will show which day of the week each pill should be taken.
Starting Yarina® Plus
Plus.If you have not taken any hormonal contraceptive in the previous month, start Yarina® Plus on the first day of your menstrual cycle (ie.i.e. on the first day of menstrual bleeding). The drug Yarina® Plus starts working immediately, so there is no need to use additional barrier methods of contraception.
It is permitted to start taking the drug on days 2-5 of the menstrual cycle, but in this case it is recommended to use an additional barrier method of contraception for the first 7 days of taking the pills from the first package.
When switching from other combination contraceptives, a vaginal ring or transdermal patch When switching from contraceptives containing only gestagens (“mini-pills,” injectable forms, implant), or from a gestagen-releasing intrauterine therapy system it is possible to switch from the “mini-pili” to Yarina® Plus on any day (without a break), from the implant or IUD with gestagen – on the day of its removal, from the injectable contraceptive – on the day when the next injection is to be made. In all cases, it is necessary to use an additional barrier method of contraception during the first 7 days of taking the pills. After an abortion (including spontaneous) in the first trimester of pregnancy the drug may be started immediately. If this condition is met, the woman does not need additional contraception. After childbirth (if no breast-feeding) or abortion (including spontaneous abortion) in the second trimester of pregnancy, it is recommended that the drug not be started until 21-28 days after childbirth (if no breast-feeding) or after an abortion in the second trimester. If it is begun later, it is necessary to use additionally a barrier method of contraception during the first 7 days of reception of tablets. If sexual intercourse took place before the start of taking Yarina® Plus, it is necessary to rule out pregnancy or wait for the first menstruation. Missing pills Missing inactive pills can be ignored. However, they should be discarded to avoid inadvertently prolonging the period of inactive pills. The following recommendations apply only to skipping active pills: If any active pill is less than 12 h late, the contraceptive protection of Yarina® Plus is maintained. You should take the missed pill as soon as possible, and the next pills should be taken at the usual time. If any active tablet is missed for more than 12 h, contraceptive protection may be reduced. The more consecutive pills missed and the closer the miss is to the beginning or end of the pill, the greater the chance of pregnancy. The following two basic rules can guide this: 1. Taking the drug should never be interrupted, for more than 7 days. 2. To achieve adequate suppression of hypothalamic-pituitary-ovarian regulation, 7 days of continuous active pills are required. Accordingly, if the delay in taking active pills is more than 12 h (the interval from taking the last pill is more than 36 h), the following can be recommended: First week of taking the drug The missed pill should be taken as soon as possible, as soon as the woman remembers it (even if this means taking two pills at once). The next pills should be taken at the usual time. In addition, an additional barrier method of contraception (for example, a condom) should be used for the next 7 days. If sexual intercourse took place in the 7 days before skipping the pill, it is necessary to consider the possibility of pregnancy. The second week of taking the drug The missed pill must be taken as soon as the woman remembers it (even if that means taking two pills at once). The next pills should be taken at the usual time. If the pill regimen is followed for the 7 days preceding the first missed pill, no additional contraceptive measures are necessary. Otherwise, and if two or more pills are missed, additional barrier methods of contraception should be used for 7 days. The third week of taking the drug The risk of pregnancy increases because of the approaching phase of taking inactive pills. One of the following two options must be strictly adhered to: If all pills were taken correctly in the 7 days preceding the first missed pill, there is no need to use additional contraceptive methods. If you take a missed pill, follow steps 1 or 2; If the pills were not taken correctly in the 7 days before the first missed pill, you must use an additional barrier method (such as a condom) for the next 7 days, in which case step 1 must be used for the missed pill. 1. The missed pill must be taken as soon as possible as soon as the woman remembers it (even if this means taking two pills at the same time). The next pills are taken at the usual time until the orange (active) pills in the package run out. The seven light orange (auxiliary) tablets should be discarded and the orange (active) tablets in the new pack should be taken immediately. Until the orange (active) tablets from the second pack are finished, bleeding cancellation is unlikely, but there may be a mucous discharge and/or breakthrough bleeding. 2. Interrupt the orange (active) pills in the current pack, then take a break for 7 days or less (including days of missed pills), after which the new pack should be started. If a woman has missed the orange (active) pills and no bleeding cancellation has occurred while taking the light orange (adjuvant) pills, it should be verified that she is not pregnant. Recommendations in gastrointestinal disorders In severe gastrointestinal disorders, absorption may be incomplete, so an additional barrier method of contraception should be used. If vomiting or diarrhea develops within 3 to 4 hours of taking the active pill, recommendations for skipping the pill should be followed. If a woman does not want to change her usual regimen and postpone the start of her menstruation to another day of the week, an additional active pill should be taken from a different package. Delaying the onset of menstrual-like bleeding . To delay the onset of menstrual bleeding, skip the seven inactive (light orange) pills in the current pack and start taking the active (orange) pills in the next pack of Yarina® Plus. If the woman has taken all the active pills from the second package, she should also take 7 inactive (light orange) pills and immediately start taking the pills from the new package. In this way the cycle can be prolonged, if you wish, for as long as you wish, up to 3 weeks, including until all the active pills of the second package have been taken. If you want menstrual bleeding to begin earlier, you should stop taking the active (orange) pills in the second pack, discard it and take a break of no more than 7 days, then start taking the pills from the new pack. In this case, menstrual bleeding will start approximately 2-3 days after taking the last active (orange) tablet from the second pack. You may experience menses and/or breakthrough bleeding while taking Yarina® Plus from the second package. Change the day menstrual bleeding starts If a woman takes the pill as recommended, menstrual bleeding will occur on approximately the same day every 4 weeks. If a woman wants to change the day her menstrual bleeding starts, she should stop taking the inactive (light orange) pills for as many days as she wants to change the start of her menstrual bleeding. For example, if a woman usually starts her cycle on a Friday and she wants it to start on a Tuesday (3 days earlier), she would start taking the pills in the next package 3 days earlier than usual, that is, to stop taking the last 3 inactive (light orange) pills of the current package and start taking the pills of the next package. The fewer inactive (light orange) pills a woman takes, the more likely it is that menstrual bleeding will not occur. When taking Yarina® Plus from the next package, a woman may experience menses and/or breakthrough bleeding. Stopping Yarina® Plus Yarina® Plus can be stopped at any time. Other contraceptive methods should be taken care of if pregnancy is not planned. If you do plan to get pregnant, you should simply stop taking the medicine. Special categories of patients The effectiveness and safety of Yarina® Plus have been studied in women of reproductive age. The efficacy and safety of the drug in postpubertal age to 18 years are expected to be similar in women after 18 years of age. The use of the drug is contraindicated until the menstrual cycle is established. The drug is not indicated after the onset of menopause. The drug is contraindicated in women with severe liver function disorders. The drug is contraindicated in women with severe renal impairment and acute renal failure.
Interaction
Interaction
The effect of other drugs on the drug Yarina®Plus
Possible interaction with drugs that induce microsomal enzymes, which may result in increased clearance of sex hormones, which, in turn, may lead to breakthrough uterine bleeding and/or reduction of contraceptive effect.
Women who are treated with these drugs in addition to Yarina® Plus are advised to temporarily use a barrier method of contraception or choose another non-hormonal method of contraception. The barrier method of contraception should be used during the entire period of taking concomitant drugs, and for 28 days after their withdrawal. If the barrier method of contraception ends later than the orange (active) tablets in the Yarina® Plus package, you should skip the light orange (adjuvant) tablets and start taking the tablets from the new Yarina® Plus package.
Medications that increase the clearance of Yarina® Plus (which weaken effectiveness by inducing enzymes): phenytoin, barbiturates, primidone, carbamazepine, rifampicin, and possibly also oxcarbazepine, topiramate, felbamate, griseofulvin, and drugs containing St. John’s wort.
Medications with different effects on clearance of Yarina® Plus: Many HIV or hepatitis C virus protease inhibitors and non-nucleoside reverse transcriptase inhibitors can either increase or decrease plasma concentrations of estrogen or progestins when used together with Yarina® Plus. In some cases this effect can be clinically significant.
Medications that decrease the effectiveness of calcium levomepolate: Some medications reduce plasma folate concentrations and decrease folate efficacy by inhibiting the dihydrofolate reductase enzyme (e.g., methotrexate, trimethoprim, sulfasalazine, and triamterene) or by reducing folate absorption (e.g., colestyramine) or by unknown mechanisms (e.g., antiepileptic drugs carbamazepine, phenytoin, phenobarbital, primidone, and valproic acid).
Medications that reduce the clearance of combined oral contraceptives (enzyme inhibitors): Strong to moderate CYP3A4 inhibitors, such as azole-group antifungals (e.g., itraconazole, voriconazole, fluconazole), verapamil, macrolide group antibiotics (e.g., clarithromycin, erythromycin), diltiazem and grapefruit juice may increase plasma concentrations of estrogen or progestin, or both.
Etoricoxib at doses of 60 and 120 mg/day when combined with combined oral contraceptives containing 0.035 mg ethinylestradiol has been shown to increase plasma concentrations of ethinylestradiol by 1.4 and 1.6 times, respectively.
The effect of combined oral contraceptives or calcium levomepholate on other drugs
The combined oral contraceptives may affect the metabolism of other drugs, resulting in an increase (e.g., cyclosporine) or decrease (e.g., lamotrigine) in their plasma and tissue concentrations.
In vitro drospirenone is able to slightly or moderately inhibit the cytochrome P450 enzymes CYP1A1, CYP2C9, CYP2C19 and CYP3A4.
Based on in vivo interaction studies in female volunteers taking omeprazole, simvastatin, or midazolam as marker substrates, we can conclude that clinically significant effects of 3 mg drospirenone on drug metabolism mediated by cytochrome P450 enzymes are unlikely.
In vitro, ethinylestradiol is a reversible inhibitor of CYP2C19, CYP1A1 and CYP1A2 and an irreversible inhibitor of CYP3A4/5, CYP2C8 and CYP2J2. In clinical trials, administration of a hormonal contraceptive containing ethinylestradiol has resulted in no or only a slight increase in plasma concentrations of CYP3A4 substrates (e.g., midazolam), whereas plasma concentrations of CYP1A2 substrates may increase slightly (e.g., theophylline) or moderately (e.g., melatonin and tizanidine).
The folate may modify the pharmacokinetics or pharmacodynamics of some drugs that influence folate metabolism, e.g., antiepileptic drugs (phenytoin), methotrexate or pyrimethamine, which may be accompanied by a decrease (generally reversible if the dose of the folate-improving drug is increased) in their therapeutic effect. Administration of folate against the background of treatment with these drugs is recommended mainly to reduce the toxicity of the latter.
In patients with normal renal function the combined use of drospirenone and ACE inhibitors or NSAIDs has no significant effect on plasma potassium concentrations. However, the combined use of Yarina®Plus with aldosterone antagonists or potassium-saving diuretics has not been studied. In such cases, the plasma potassium concentration should be monitored during the first cycle of administration.
Special Instructions
Special Instructions
If any of the conditions, diseases, and risk factors listed below are present, the potential risks and expected benefits of Yarina® Plus should be carefully weighed on an individual basis and discussed with the woman before she decides to start taking this medication.
Cardiovascular disease
Here is some epidemiological evidence for the use of Yarina® Plus. There is epidemiologic evidence of an increased incidence of venous and arterial thrombosis and thromboembolisms (such as deep vein thrombosis, pulmonary embolism, myocardial infarction, stroke) when taking combined oral contraceptives. These diseases are rare.
The risk of venous thromboembolism (VTE) is highest in the first year of use of these drugs. An increased risk is present after initial use of combined oral contraceptives or renewed use of the same or different combined oral contraceptives (after a break of 4 weeks or more between doses). Data from a large prospective study involving 3 groups of patients show that this increased risk is predominantly present during the first 3 months.
The overall risk of VTE in patients taking low-dose combination oral contraceptives (< 50 µg ethinylestradiol) is 2-3 times higher than in nonpregnant patients not taking combined oral contraceptives, yet this risk remains lower compared with the risk of VTE in pregnancy and childbirth.
VTE can be fatal (1-2% of cases).
VTE, manifesting as deep vein thrombosis or pulmonary embolism, can occur with any combination oral contraceptive.
It is extremely rare for thrombosis of other blood vessels, such as hepatic, mesenteric, renal, cerebral veins and arteries, or retinal vessels, to occur with the use of combined oral contraceptives. There is no consensus on the association between the occurrence of these events and the use of combined oral contraceptives.
The symptoms of deep vein thrombosis (DVT) include unilateral swelling of the lower extremity or along the vein of the lower extremity, pain or discomfort in the lower extremity only when upright or walking, localized temperature rise in the affected lower extremity, redness or discoloration of the skin on the lower extremity.
The symptoms of pulmonary artery thromboembolism (TELA) include difficulty or rapid breathing; sudden cough, including coughing with hemoptysis; sharp chest pain, which may increase with deep breaths; anxiety; severe dizziness; and rapid or irregular heartbeat. Some of these symptoms (e.g., shortness of breath, coughing) are nonspecific and may be misinterpreted as signs of other more or less severe events (e.g., respiratory tract infection).
Arterial thromboembolism can lead to stroke, vascular occlusion, or myocardial infarction. Symptoms of stroke: sudden weakness or loss of sensation in the face, upper or lower extremities, especially on one side of the body; sudden confusion, problems with speech and comprehension; sudden one- or two-sided loss of vision; sudden gait disturbance, dizziness, loss of balance or coordination of movements; sudden, severe or prolonged headache for no apparent reason; loss of consciousness or fainting with or without an epileptic seizure. Other signs of vascular occlusion: sudden pain, swelling and mild bruising of the extremities, “acute abdominal” symptomcomplex.
Symptoms of myocardial infarction: pain, discomfort, pressure, heaviness, a feeling of compression or distension in the chest, in the arm or behind the chest; discomfort with irradiation to the back, cheekbone, throat, arm, stomach; cold sweat, nausea, vomiting or dizziness, marked weakness, anxiety or shortness of breath; rapid or irregular heartbeat.
Arterial thromboembolism can be life-threatening or fatal.
In women with a combination of several risk factors or high severity of one of them (e.g., complicated valvular heart disease, uncontrolled arterial hypertension, extensive surgery with prolonged immobilization), their mutual reinforcement should be considered. In such cases, the total value of the existing risk factors increases. In this case the use of Yarina® Plus is contraindicated.
The risk of thrombosis (venous and/or arterial) and thromboembolism is increased:
– with age;
– in smokers (the risk increases with more cigarettes or greater age, especially in women over 35);
if:
– obesity (BMI greater than 30 kg/m2);
– indications in family history (e.g., venous or arterial thromboembolism ever in a close relative or parent at a relatively young age). If there is a hereditary or acquired predisposition, a woman should be referred to a specialist for a decision about the possibility of using Yarina® Plus;
– prolonged immobilization, serious surgical intervention, any surgery on the lower extremities or extensive trauma. In these situations, it is advisable to discontinue Yarina® Plus (if surgery is planned, at least 4 weeks before) and not to resume for 2 weeks after the end of immobilization;
– dyslipoproteinemia;
– arterial hypertension;
– migraine;
– heart valve disease;
– atrial fibrillation.
The possible role of varicose veins and superficial thrombophlebitis in venous thromboembolism remains controversial.
The increased risk of thromboembolism in the postpartum period should be considered.
Peripheral circulatory disorders may also be seen in diabetes mellitus, systemic lupus erythematosus, hemolytic-uremic syndrome, chronic inflammatory bowel disease (Crohn’s disease or IBD) and sickle cell anemia.
An increase in the frequency and severity of migraines during the use of Yarina®Plus (which may precede cerebrovascular disorders) may be grounds for immediate discontinuation of this drug.
The biochemical indicators indicating an inherited or acquired predisposition to venous or arterial thrombosis include the following: Activated protein C resistance, hyperhomocysteinemia, antithrombin III deficiency, protein C deficiency, protein S deficiency, phospholipid antibodies (cardiolipin antibodies, lupus anticoagulant).
When evaluating the risk-benefit ratio, consider that adequate treatment of the condition may reduce the associated risk of thrombosis. It should also be considered that the risk of thrombosis and thromboembolism in pregnancy is higher than with low-dose oral contraceptives (< 50 mcg ethinylestradiol).
Tumors
The most significant risk factor for cervical cancer is persistent papillomavirus infection. There have been reports of some increased risk of cervical cancer with long-term use of combined oral contraceptives. However, the association with taking combined oral contraceptives has not been proven. The possibility of an association of these findings with cervical disease screening and with patterns of sexual behavior (less frequent use of barrier methods of contraception) is discussed.
A meta-analysis of 54 epidemiological studies showed that there is a slightly increased relative risk of breast cancer diagnosed in women currently taking combined oral contraceptives (relative risk 1.24). The increased risk gradually disappears within 10 years of stopping these drugs. Because breast cancer is rare in women under 40 years of age, the increase in breast cancer diagnoses in women currently taking the combined oral contraceptives or who have recently taken them is small relative to the overall risk of the disease. Its association with the use of combined oral contraceptives has not been proven. The observed increase in risk may be a consequence of close monitoring and earlier diagnosis of breast cancer in women who use combined oral contraceptives. Women who have ever used combined oral contraceptives are found to have earlier stages of breast cancer than women who have never used them.
In rare cases, development of benign and, in extremely rare cases, malignant hepatic neoplasms has been observed with combined oral contraceptives, which in some patients led to life-threatening intra-abdominal bleeding.
If severe abdominal pain, enlargement of the liver, or signs of intra-abdominal bleeding occur, this should be considered when making a differential diagnosis.
Other conditions
Clinical studies have shown no effect of drospirenone on plasma potassium concentrations in patients with mild to moderate renal impairment. However, in patients with impaired renal function and baseline potassium concentration at the upper limit of normal, the risk of hyperkalemia with the use of drugs that lead to potassium retention in the body cannot be excluded.
Women with hypertriglyceridemia (or a family history of this condition) may have an increased risk of pancreatitis when taking combined oral contraceptives.
While small increases in BP have been described in many women taking combined oral contraceptives, clinically significant increases have been rare. However, if a persistent, clinically significant increase in BP develops during the use of Yarina® Plus, the drug should be discontinued and treatment for arterial hypertension should be initiated. The drug can be continued if normal BP values are achieved with hypotensive therapy.
The following conditions have been reported to develop or worsen with both pregnancy and combined oral contraceptives, but their association with taking combined oral contraceptives has not been proven: Jaundice and/or pruritus associated with cholestasis; gallstone formation; porphyria; systemic lupus erythematosus: hemolytic-uremic syndrome; Sydenham’s chorea; pregnancy herpes; hearing loss associated with otosclerosis. Cases of Crohn’s disease and ulcerative colitis have also been described against the background of combined oral contraceptives.
In women with hereditary forms of angioedema, exogenous estrogens may cause or worsen symptoms of angioedema.
Acute or chronic liver dysfunction may require discontinuation of Yarina® Plus until liver function returns to normal. Recurrent cholestatic jaundice, which develops for the first time during pregnancy or during previous use of sex hormones, requires discontinuation of Yarina® Plus.
While combined oral contraceptives may affect insulin resistance and glucose tolerance, it is not necessary to change the therapeutic regimen in diabetic patients using Yarina® Plus. However, women with diabetes mellitus should be closely monitored during the use of this drug.
Sometimes chloasma may develop, especially in women with a history of pregnancy chloasma. Women with a history of chloasma should avoid prolonged sun exposure and exposure to ultraviolet radiation while taking Yarina® Plus.
The folate may mask vitamin B12 deficiency.
Doclinical safety data
Preclinical data from standard multiple-dose toxicity studies, as well as genotoxicity, carcinogenic potential, and reproductive toxicity, do not indicate any particular risk to humans. However, we should keep in mind that sex hormones can promote the growth of some hormone-dependent tissues and tumors.
Laboratory tests
The administration of Yarina® Plus may affect the results of some laboratory tests, including liver, kidney, thyroid and adrenal function, plasma transport protein concentrations, carbohydrate metabolism, clotting and fibrinolysis parameters. The changes usually do not go beyond the normal values. Drospirenone increases plasma renin activity and aldosterone concentration, which is associated with its anti-mineralocorticoid effect.
There is a theoretical possibility of increased plasma potassium concentrations in women receiving Yarina® Plus concomitantly with other drugs that may increase plasma potassium levels. These drugs include angiotensin II receptor antagonists, potassium-saving diuretics, and aldosterone antagonists. However, in studies evaluating the interaction of drospirenone with ACE inhibitors or indomethacin, no significant difference was found between plasma potassium concentrations compared with placebo.
Decreased efficacy
The efficacy of Yarina® Plus may be reduced in the following cases: skipping pills, gastrointestinal distress or as a result of drug interactions.
Frequency and severity of menstrual bleeding
. Irregular (acyclical) bleeding and vaginal bleeding (spotting or breakthrough uterine bleeding) may occur with Jarina® Plus, especially during the first months of use. You should use hygiene products and continue taking the pills as usual. Any irregular bleeding should be evaluated after an adjustment period of approximately 3 cycles.
If irregular bleeding recurs or develops after previous regular cycles, a thorough evaluation should be performed to rule out malignancy or pregnancy.
Some women may not develop a bleeding discontinuation during a break in the pill. If Yarina® Plus was taken as recommended, it is unlikely that the woman is pregnant. However, if irregular use of Yarina® Plus and no two consecutive bleeding cancellations occur, the drug cannot be continued until pregnancy is ruled out.
Medical examinations
. Before starting or resuming the use of the drug it is necessary to review the life history, family history of the woman, conduct a thorough physical examination (including measurement of BP, heart rate, determination of BMI, breast examination), gynecological examination, cervical cytology (Papanicolaou test), exclude pregnancy. When resuming the use of Yarina® Plus, the scope of additional examinations and the frequency of follow-up examinations are determined individually, but at least once every 6 months.
The woman should be warned that Yarina® Plus does not protect against HIV infection and other sexually transmitted diseases.
Conditions requiring medical advice
Any change in health, especially the occurrence of the conditions listed under “Contraindications” and “Caution;
A localized thickening in the breast;
At the same time as other medicines (see “Drug Interactions”).
If prolonged immobility is expected (e.g., lower extremity in a cast), or if hospitalization or surgery is planned (at least 3-4 weeks before the anticipated surgery);
If unusually heavy vaginal bleeding – The pill was missed in the first week of the bottle and sexual intercourse occurred 7 days or less before that time;
If I do not have another menstrual bleeding for 2 consecutive periods or I suspect pregnancy (do not start the pills from the next bottle until you have talked to your doctor).
The pills should be stopped and a doctor should be consulted immediately if there are possible signs of thrombosis, myocardial infarction, or stroke: unusual cough; unusually severe pain behind the chest, extending to the left arm; sudden shortness of breath, unusual, severe and prolonged headache or migraine attack; partial or complete loss of vision or double vision; slurred speech; sudden changes in hearing, smell or taste; dizziness or fainting; weakness or loss of sensation in any part of the body; severe stomach pain; severe pain in a lower extremity or sudden swelling in either lower extremity.
Influence on driving and operating ability
There have been no reports of adverse effects of Yarina® Plus on psychomotor reaction speed; no studies of the effect of the drug on psychomotor reaction speed have been conducted.
Contraindications
Contraindications
Yarina Plus is contraindicated in the presence of any of the conditions/diseases listed below. If any of these conditions/diseases develop for the first time while taking the drug, it should be stopped immediately.
- Thrombosis (venous and arterial) and thromboembolism at present or in the history (including deep vein thrombosis, pulmonary embolism, myocardial infarction, stroke), cerebrovascular disorders.
- Conditions preceding thrombosis (including transient ischemic attacks, angina pectoris), current or history.
- The presence of multiple or significant risk factors for venous or arterial thrombosis.
- Hepatic failure and severe liver disease (until normalization of liver function tests).
- Severe and/or acute renal failure.
- Liver tumors (benign or malignant), current or history.
- Migraine with focal neurological symptoms, current or history
- Diabetes mellitus with vascular complications.
- Hormone-dependent malignancies (including genital or mammary glands) detected or suspected.
- Vaginal bleeding of unclear genesis.
- High sensitivity or intolerance to any of the components of Yarina Plus.
- Yarina Plus contains lactose, so it is contraindicated in patients with rare hereditary lactose intolerance, lactase deficiency or glucose-galactose malabsorption.
- Pregnancy or suspected pregnancy.
- Breastfeeding period.
With caution
The potential risks and expected benefits of Yarina Plus should be evaluated on a case-by-case basis if the following diseases/conditions and risk factors are present:
- Risk factors for thrombosis and thromboembolism: Smoking, obesity, dyslipoproteinemia, controlled arterial hypertension, migraine without focal neurological symptoms, uncomplicated heart valve defects, hereditary predisposition to thrombosis (thrombosis, myocardial infarction or cerebrovascular disease at a young age in any of the immediate family members);
- Other conditions in which peripheral circulatory disorders may be noted: Diabetes mellitus without vascular complications, systemic lupus erythematosus, hemolytic-uremic syndrome, Crohn’s disease and ulcerative colitis, sickle cell anemia, superficial vein phlebitis;
- Hereditary angioedema;
- Hypertriglyceridemia:
- Liver disease that is not a contraindication (see “Contraindications”);
- .Diseases that first appeared or worsened during pregnancy or on previous use of sex hormones (e.g., jaundice and/or pruritus associated with cholestasis, cholelithiasis, otosclerosis with hearing impairment, porphyria, herpes of pregnancy, Sydenham’s chorea);
- Postpartum period.
.
Side effects
Side effects
immune system disorders:frequency unknown – hypersensitivity reactions.
Metabolism and nutrition: infrequent – change in body weight, fluid retention.
Psychiatric disorders:often – depressed mood; infrequent – change in libido; frequency unknown – mood swings.
Nervous system disorders:often – headache, migraine.
Visual side:frequent unknown – contact lens intolerance.
Hearing organ:recent – hypoacusis.
Cardiovascular system disorders: infrequent – increased BP, decreased BP; rarely – thromboembolism.
In the respiratory system: rarely – bronchial asthma.
Gastrointestinal disorders:often – nausea; infrequently – vomiting; frequency unknown – abdominal pain, diarrhea.
Skin and subcutaneous tissue disorders: infrequent – acne, eczema, pruritus, alopecia; frequency unknown – rash, urticaria, erythema nodosa, erythema multiforme.
Gender and mammary gland side: often – pain in the mammary glands (including breast engorgement), mammary gland soreness, colic (including vaginal discharge), candida vulvovaginitis, absence of menstrual-like bleeding, painful menstrual-like bleeding, heavy menstrual-like bleeding, scant menstrual-like discharge, absence of menstrual-like bleeding, acyclic bleeding (usually reduced with long-term use of the drug); infrequent – vaginitis; rarely – discharge from the mammary glands; frequency unknown – enlargement of the mammary glands.
.
Overdose
Overdose
No cases of overdose of Yarina® Plus have been reported.
Symptoms that may occur in case of overdose: nausea, vomiting, mucous bloody vaginal discharge or metrorrhagia (more often in young women).
Treatment: There is no specific antidote, symptomatic treatment should be carried out. Calcium levomepholate and its metabolites are identical to folate in food products, the daily consumption of which is not harmful to the body. Calcium levomepholate administration at the dose of 17 mg per day (37 times more than the dose contained in 1 tablet of the preparation Yarina® Plus) during 12 weeks was well tolerated.
Pregnancy use
Pregnancy use
The drug is contraindicated during pregnancy. If pregnancy is detected while taking Yarina Plus, the drug should be stopped immediately.
The data on the results of taking Yarina Plus during pregnancy are limited, and it is not possible to draw any conclusions about the negative effects of the drug on pregnancy, fetal health and the newborn baby.
At the same time, extensive epidemiologic studies have found no increased risk of birth defects in children born to women who have taken OCs before pregnancy or teratogenic effects in cases of reckless use of OCs in early pregnancy. No specific epidemiological studies have been conducted for YarinaPlus.
Lactation
The drug is contraindicated during breast-feeding. Taking OCs may decrease the amount of breast milk and change its composition, so their use is not recommended until you stop breastfeeding. A small amount of sex hormones and/or their metabolites may be excreted with milk, but there is no evidence of adverse effects on the health of the baby.
.
Additional information
| Weight | 0.034 kg |
|---|---|
| Shelf life | 2 years |
| Conditions of storage | At a temperature not higher than 25 ° C. Keep out of reach of children. |
| Manufacturer | Bayer Weimar GmbH & Co. KG, Germany |
| Medication form | tablet set |
| Brand | Bayer Weimar GmbH & Co. KG |
Related products
Gynecology and Obstetrics
Gynecology and Obstetrics
Buy Yarina Plus, 84 pcs. with delivery to USA, UK, Europe and over 120 other countries.