No products in the cart.
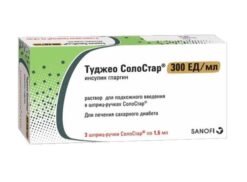
Tugeo SoloStar, 300 units/ml 1.5 ml cartridges in SoloStar syringe pens 5 pcs
€1.00
Out of stock
(E-mail when Stock is available)
Description
Type 2 Diabetes, Type 1 Diabetes
Diabetes mellitus in adults requiring insulin treatment.
Active ingredient
Active ingredient
Insulin glargine
Composition
Composition
1 ml of the solution contains:
the active ingredient:
insulin glargine 300 IU (10.91 mg);
components:
methacresol (m-cresol) – 2.70 mg,
zinc chloride – 0.19 mg (corresponding to 0.09 mg of zinc), glycerol (85%) – 20 mg, <
Sodium hydroxide – to pH 4.0,
Hydrochloric acid – to pH 4.0,
Injectable water – to 1.0 ml.
How to take, the dosage
How to take, the dosage
Units of Tugeo SoloStar® (insulin glargine 300 IU/ml) refer only to Tugeo SoloStar and are not equivalent to other units expressing the potency of other insulin analogues. Tugeo SoloStar should be administered p/k once daily at any time of the day, preferably at the same time. Tugeo SoloStar when administered once daily allows for flexibility in the injection schedule: If necessary, patients can have the injection within 3 hours before or 3 hours after their usual time of administration.
In all patients with diabetes mellitus, monitoring of blood glucose concentrations is recommended.
The initiation of Tugeo SoloStar:
- Patients with type 1 diabetes. Tugeo SoloStar should be used once daily in combination with insulin administered with meals and requires individual dose adjustment.
- Patients with type 2 diabetes. The recommended starting dose is 0.2 IU/kg once daily, followed by individual dose adjustment.
Conversion from 100 U/ml insulin glargine to Tugeo SoloStar and vice versa from Tugeo SoloStar® to 100 U/ml insulin glargine
The 100 U/ml insulin glargine and Tugeo SoloStar are not bioequivalent and are not directly interchangeable.
- Tojeo SoloStar can be switched from insulin glargine 100 units/mL to Tugeo SoloStar at a unit per unit rate, but a higher dose of Tugeo SoloStar may be required to achieve the target range of plasma glucose concentrations.
- Tojeo SoloStar switched to 100 units/ml insulin glargine to reduce the risk of hypoglycemia, the dose should be reduced (approximately 20%), followed by dose adjustments if necessary.
We recommend careful metabolic monitoring during and in the first few weeks after switching from one of these drugs to another.
Transitioning from other basal insulins to Tugeo SoloStar
. Transition from treatment regimen with intermediate and long-acting insulins to treatment regimen with Tugeo SoloStar may require change of basal insulin dose and correction of simultaneously conducted hypoglycemic therapy (change of doses and time of administration of short-acting insulins or fast-acting insulin analogues, or doses of non-insulin hypoglycemic agents).
- Change from daily doses of basal insulin to daily doses of Tugeo SoloStar at a rate of one unit of the previously given basal insulin dose.
- Tugeo SoloStar is recommended as an initial dose of 80% of the total daily dose of basal insulin that is discontinued when changing from twice daily basal insulin doses to a single dose of Tugeo SoloStar. Patients with high doses of insulin, due to their antibodies to human insulin, may have an improved response to Tugeo SoloStar.
Careful metabolic monitoring is recommended during the transition to Tugeo SoloStar and for several weeks thereafter.
Interaction
Interaction
A number of medications affect glucose metabolism, which may require insulin dose adjustment and particularly close monitoring if used concomitantly with insulins.
Drugs that may increase the hypoglycemic effect of insulin and the propensity to develop hypoglycemia
Oral hypoglycemic agents, angiotensin-converting enzyme inhibitors (ACEs), salicylates, disopyramide; fibrates, fluoxetine, monoamine oxidase inhibitors (MAOIs), pentoxifylline, propoxifen, sulfonamide antibiotics.
The concomitant administration of these drugs with insulin glargine may require adjustment of the insulin dose.
Drugs that may weaken the hypoglycemic effect of insulin
Glucocorticosteroids, danazol, diazoxide, diuretics, sympathomimetics (such as adrenaline, salbutamol, terbutaline); glucagon, isoniazid, phenothiazine derivatives, somatotropic hormone, thyroid hormones, estrogens and gestagens (such as in hormonal contraceptives), protease inhibitors and atypical neuroleptics (such as olanzapine and clozapine).
The concomitant use of these medications with insulin glargine may require adjustment of the insulin dose.
Beta-adrenoblockers, clonidine, lithium salts, and ethanol may both enhance and weaken the hypoglycemic effects of insulin. Pentamidine in combination with insulin may cause hypoglycemia, which sometimes changes to hyperglycemia.
Sympatholytic drugs – Sympathomimetic drugs such as beta-adrenoblockers, clonidine, guanethidine and reserpine may reduce or lack signs of adrenergic counterregulation (sympathetic nervous system activation in response to hypoglycemia).
Interaction with pioglitazone
When using pioglitazone in combination with insulin, cases of heart failure have been reported, especially in patients at risk of heart failure (see section “Special Precautions”). In case of appearance or aggravation of cardiac symptoms, the use of pioglitazone should be discontinued.
.
Special Instructions
Special Instructions
Patients should have the skills to self-monitor their diabetes, including monitoring blood glucose concentrations, as well as adhering to proper injection technique and being able to manage hypoglycemia and hyperglycemia. Insulin therapy requires constant alertness to the possibility of hyperglycemia or hypoglycemia.
If blood glucose control is insufficient or if there is a tendency toward hypo- or hyperglycemia, accurate compliance with the prescribed dosing regimen, adherence to the site of administration, correct technique of hypodermic injections and handling of the SoloStar syringe, and consideration of all other factors that may contribute to this condition should be given before proceeding with a dosing adjustment.
Contraindications
Contraindications
- high sensitivity to insulin glargine or any of its excipients
- under 18 years of age (due to lack of clinical data confirming the efficacy and safety of the drug in children and adolescents).
Side effects
Side effects
The adverse reactions (HP) listed below were observed during clinical studies conducted with Tugeo SoloStar® and during clinical use of insulin glargine 100 units/mL.
These HPs are presented by organ system (as classified by the Medical Dictionary of Regulatory Affairs (MedDRA)) according to the following World Health Organization (WHO) recommended frequency gradations: Very common (≥10%); common (≥1%; < 10%); infrequent (≥0.1%; < 1%); rare (≥0.01%; < 0.1%); very rare (< 0.01%), frequency unknown (the incidence of HP could not be determined from available data).
Metabolic and nutritional disorders
Hypoglycemia
Hypoglycemia, the most common adverse reaction with insulin therapy, can occur if the insulin dose is too high compared to the need for it.
As with other insulins, episodes of severe hypoglycemia, especially recurrent ones, can lead to neurological impairment. Episodes of prolonged and severe hypoglycemia can be life threatening for patients.
In many patients, signs and symptoms of neuroglycopenia (feeling of fatigue, inadequate fatigue or weakness, decreased ability to concentrate, drowsiness, visual disturbances, headache, nausea, confusion or loss of consciousness, seizure syndrome) are preceded by signs of adrenergic counter-regulation (sympathoadrenal system activation in response to hypoglycemia): feeling of hunger, irritability, nervous excitement or tremor, restlessness, pale skin, “cold” sweat, tachycardia, pronounced palpitations. Usually, the faster hypoglycemia develops, and the more severe it is, the more pronounced are the symptoms of adrenergic counterregulation.
Visual disturbances
Significant improvement in glycemic control may cause temporary visual impairment due to temporary impairment of ocular lens turgor and refractive index.
Long-term improvement in glycemic control reduces the risk of progression of diabetic retinopathy. However, as with any insulin regimen, intensification of insulin therapy with dramatically improved glycemic control may be associated with a temporary worsening of the course of diabetic retinopathy.
In patients with proliferative retinopathy, especially those not treated with photocoagulation, episodes of severe hypoglycemia may result in transient vision loss.
Skin and subcutaneous tissue disorders
As with treatment with any other insulin drugs, lipodystrophy may develop at the injection site, which may slow down local absorption of insulin. When using insulin therapy regimens that include insulin glargine, lipodystrophy was observed in 1-2% of patients, and lipoatrophy was observed infrequently. Constant change of injection sites within the body areas recommended for subcutaneous insulin injection may help to reduce the severity of this reaction or prevent its development.
Musculoskeletal and connective tissue disorders
Very rare: Myalgia.
General disorders and disorders at the site of administration
Local allergic reactions at the site of administration
As with any insulin therapy, these reactions include skin redness, pain, itching, urticaria, rash, edema and inflammation. In clinical studies conducted with Tugeo SoloStar® in adult patients, the incidence of all injection site reactions in patients treated with Tugeo SoloStar® (2.5%) was similar to that in patients treated with insulin glargine 100 units/ml (2.8%). Most minor reactions at the site of insulin administration usually go away within a few days or a few weeks.
Systemic allergic reactions
Allergic reactions of the immediate type to insulin are rare. These reactions to insulin (including insulin glargine) or excipients may be accompanied by, for example, generalized skin reactions, angioedema (Quincke’s edema), bronchospasm, decreased blood pressure, and shock, and may be life-threatening.
Other reactions
The use of insulin may cause the formation of antibodies to it. In clinical studies comparing Tugeo SoloStar® and insulin glargine 100 units/ml, antibody formation to insulin was observed with equal frequency in both treatment groups.
As with other insulins, in rare cases the presence of such insulin antibodies may require a change in insulin dose to reverse the tendency to develop hypoglycemia or hyperglycemia.
In rare cases, insulin may cause sodium retention and edema, particularly when previously inadequate metabolic control is improved with intensified insulin therapy.
Children
The safety profile for children and adolescents younger than 18 years of age has not been established at this time.
Overdose
Overdose
Symptoms
Insulin overdose (excess insulin in relation to food intake, energy expenditure, or both) can lead to severe and sometimes prolonged and life-threatening hypoglycemia.
Treatment
Moderate episodes of hypoglycemia are usually managed by oral administration of rapidly digestible carbohydrates. It may be necessary to change the dosing regimen of the drug, the diet, or physical activity.
Episodes of more severe hypoglycemia manifested by coma, seizures or neurological disorders may be controlled by intramuscular or subcutaneous administration of glucagon or intravenous infusion of concentrated dextrose (glucose) solution. Prolonged intake of carbohydrates and monitoring by a specialist may be necessary, since after a visible clinical improvement, a relapse of hypoglycemia is possible.
.
Additional information
| Weight | 0.200 kg |
|---|---|
| Manufacturer | Sanofi-Aventis Deutschland GmbH, Germany |
| Medication form | solution |
| Brand | Sanofi-Aventis Deutschland GmbH |
Other forms…
Related products
Buy Tugeo SoloStar, 300 units/ml 1.5 ml cartridges in SoloStar syringe pens 5 pcs with delivery to USA, UK, Europe and over 120 other countries.