No products in the cart.
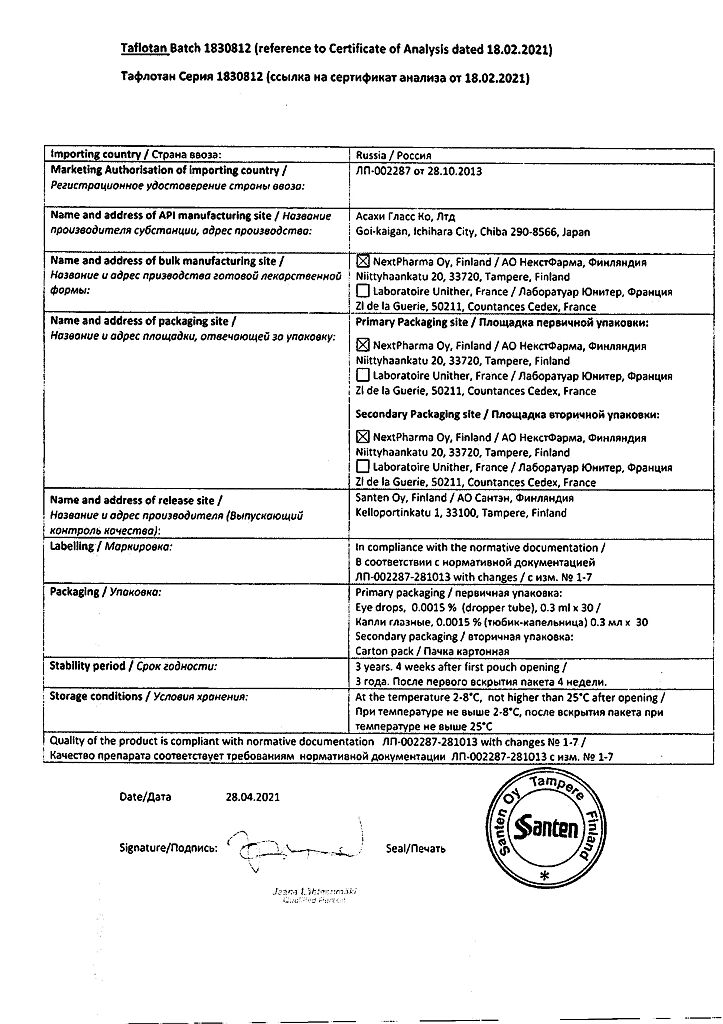
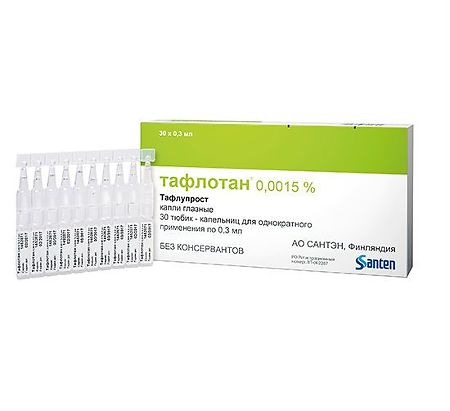
Taflotan, eye drops 0.0015% 0.3 ml 30 pcs
€25.81 €21.51
Description
Tafluprost is a fluorinated analogue of prostaglandin F2α. As its biologically active metabolite, tafluprost acid is highly active and selective for the human FP-prostanoid receptor. The affinity of tafluprost acid to the FP-receptor is 12 times higher than the affinity of latanoprost. Pharmacodynamic studies in monkeys have shown that tafluprost reduces intraocular pressure by increasing uveoscleral outflow of aqueous humor.
Pharmacodynamic Effect
The experiments in monkeys with normal and elevated intraocular pressure (IOP) have demonstrated that tafluprost is an effective drug for reducing IOP. In a study examining the IOP-lowering effects of tafluprost metabolites, tafluprost acid alone was found to significantly lower IOP.
The study, on rabbits treated for 4 weeks with tafluprost ophthalmic solution, 0.0015%, once daily, showed that blood flow in the optic disc was significantly (15%) increased compared to baseline, when measured at day 14 and 28 using laser speckle flowography.
The clinical effect
The decrease in intraocular pressure begins within 2-4 hours after the first instillation of the drug, and the maximum effect is achieved after about 12 hours. The duration of the effect lasts for at least 24 hours. Leading studies on the use of tafluprost containing the preservative benzalkonium chloride have shown that tafluprost is effective as monotherapy and also has an additive effect when used as an additional therapy to timolol. In a 6-month study, tafluprost, at various time points during the day, demonstrated a significant, IOP-lowering effect: 6 to 8 mmHg, compared with latanoprost, which reduced IOP by 7 to 9 mmHg.
In another 6-month clinical trial, tafluprost reduced IOP by 5 to 7 mmHg and timolol by 4 to 6 mmHg. The IOP-lowering effect of tafluprost also persisted when the duration of these studies was increased to 12 months. In a 6-week study, the IOP-lowering effect of tafluprost was compared with that of its indifferent filler when used in combination with timolol. Compared with baseline values (measured after 4 weeks of treatment with timolol), the additional IOP-lowering effect was 5-6 mm Hg in the timolol-tafluprost group and 3-4 mm Hg in the timolol-idifferent filler group. In a small cross-sectional study, with a 4-week treatment period, the drug forms with and without the preservative showed a similar IOP-lowering effect of more than 5 mm Hg.
In addition, in a 3-month study in the United States, when comparing, the formulation of tafluprost without preservative with timolol. also without preservative, tafluprost was found to reduce IOP by 6.2-7.4 mmHg at different time points, whereas values for timolol varied between 5.3 and 7.5 mmHg.
Pharmacokinetics
Absorption
. After instillation of tafluprost eye drops, 0.0015% in a tube dropper, without preservative, once daily, one drop in both eyes for 8 days, its plasma concentrations were low and had a similar profile on days 1 and 8. Plasma concentrations peaked 10 minutes after instillation and declined to a level lower than the lower limit of detection (10 pg/ml) in less than an hour after administration. The mean Cmax (26.2 and 26.6 pg/ml) and AUCo-last (394.3 and 431.9 pg/ml) values were almost identical on days 1 and 8, indicating that within the first week of treatment, a stable drug concentration was already achieved. No statistically significant differences in systemic bioavailability were observed between dosage forms with and without a preservative.
In a study on rabbits, the absorption of tafluprost into aqueous humor, after a single instillation of tafluprost ophthalmic solution, 0.0015% with and without a preservative, was comparable.
Distribution
In a study on monkeys, there was no specific distribution of radioactively labeled tafluprost in the iris, ciliary body, or ocular vasculature, including the retinal pigment epithelium, indicating a low affinity of the drug for melanin pigment.
Autoradiographic study in rats showed that the highest concentration of radioactivity was observed in the cornea, followed by the eyelids, sclera and iris. Systemically, radioactivity spread to the lacrimal system, palate, esophagus, gastrointestinal tract, kidneys, liver, gallbladder, and bladder. The in vitro binding of tafluprost acid to human serum albumin is 99% for 500 ng/mL of tafluprost acid.
Biotransformation
. The major pathway of metabolism of tafluprost in humans tested in vitro is hydrolysis to form the pharmacologically active metabolite, tafluprost acid, which is then mstabolized by glucuronidation or beta-oxidation to form pharmacologically inactive 1,2-dinor and 1,2,3,4-tetranor tafluprost acids, which can be glucuronidated or hydroxylated. The cytochrome P450 enzyme system (CYP) is not involved in metabolism of tafluprost acid. In a study performed on rabbit corneal tissue with refined enzymes, carboxylesterase was found to be the major esterase responsible for ester hydrolysis of tafluprost acid. Butyrylcholinesterase, but not acetylcholinesterase, can also contribute to hydrolysis.
In a rat study, after a single instillation of 3H-tafluprost (0.005% ophthalmic solution, 5 µl/eye) in both eyes for 21 days, about 87% of the total radioactive dose was detected in the feces. About 27-38% of the total dose was excreted with the urine, and about 44-58%, with feces.
Indications
Indications
to reduce elevated intraocular pressure in patients with open-angle glaucoma and ocular hypertension;
as monotherapy in patients who are indicated for preservative-free eye drops, or who have an insufficient response to first-line drugs, or who cannot tolerate first-line drugs or have contraindications to these drugs;
as an additional therapy to beta blockers.
Pharmacological effect
Pharmacological effect
Tafluprost is a fluorinated analogue of prostaglandin F2α. Tafluprost acid, being its biologically active metabolite, has high activity and selectivity towards the human FP-prostanoid receptor. The affinity of tafluprost acid for the FP receptor is 12 times higher than the affinity of latanoprost. Pharmacodynamic studies in monkeys showed that tafluprost reduces intraocular pressure by increasing uveoscleral outflow of aqueous humor.
Pharmacodynamic effect
Experiments in monkeys with normal and elevated intraocular pressure (IOP) demonstrated that Tafluprost is an effective drug for lowering IOP. In a study examining the IOP-lowering effect of tafluprost metabolites, it was found that only tafluprost acid significantly reduced IOP.
A study in rabbits treated for 4 weeks with tafluprost ophthalmic solution, 0.0015%, once daily, showed that optic disc blood flow increased significantly (15%) compared with baseline, when measured at days 14 and 28 using laser speckle flowgraphy.
Clinical effect
The decrease in intraocular pressure begins within 2-4 hours after the first installation of the drug, and the maximum effect is achieved after approximately 12 hours. The effect lasts for at least 24 hours. Leading studies on the use of tafluprost, which contains the preservative benzalkonium chloride, have shown that tafluprost is effective as monotherapy and also has an additive effect when used as an additional therapy to timolol. In a 6-month study, tafluprost, at various time points throughout the day, demonstrated a significant IOP-lowering effect: 6 to 8 mmHg. Art., compared with latanoprost, which reduces IOP by 7-9 mm Hg. Art..
In another 6-month clinical trial, tafluprost reduced IOP by 5-7 mmHg and timolol by 4-6 mmHg. Art.. The IOP-lowering effect of tafluprost also persisted when the duration of these studies was increased to 12 months. In a 6-week study, the IOP-lowering effect of tafluprost was compared with the effect of its indifferent vehicle when used in combination with timolol. Compared to baseline values (measurements taken after a 4-week course of treatment with timolol), the additional IOP-lowering effect was 5-6 mmHg. in the timolol-tafluprost group and 3-4 mm Hg. in the timolol-differential filler group. In a small crossover study with a 4-week treatment period, preservative-free and preservative-free formulations demonstrated similar IOP-lowering effects of greater than 5 mmHg.
In addition, in a 3-month study in the United States, a preservative-free formulation of tafluprost was compared with timolol. also without a preservative, it was found that tafluprost reduced IOP by 6.2-7.4 mmHg. at different time points, while values for timolol varied between 5.3 and 7.5 mmHg.
Pharmacokinetics
Absorption
After installation of tafluprost eye drops, 0.0015% in a dropper tube, without preservative, once a day, one drop in both eyes for 8 days, its plasma concentrations were low and had a similar profile on days 1 and 8. Plasma concentrations peaked 10 minutes after administration and decreased to levels below the lower limit of detection (10 pg/mL) less than an hour after drug administration. The average values of Cmax (26.2 and 26.6 pg/ml) and AUCo-last (394.3 and 431.9 pg/min/ml) were almost the same on days 1 and 8, indicating that already during the first week of treatment, a stable drug concentration was achieved. No statistically significant differences in systemic bioavailability were identified between dosage forms with and without preservatives.
In a study in rabbits, the absorption of tafluprost into the aqueous humor after a single administration of tafluprost ophthalmic solution, 0.0015% with and without preservative, was comparable.
Distribution
In a study in monkeys, there was no specific distribution of radiolabeled tafluprost in the iris, ciliary body or choroid, including the retinal pigment epithelium, indicating a low affinity of the drug for melanin pigment.
An autoradiographic study in rats showed that the highest concentration of radioactivity was observed in the cornea, followed by the eyelids, sclera and iris. Systemically, radioactivity spread to the lacrimal apparatus, palate, esophagus, gastrointestinal tract, kidneys, liver, gall bladder and bladder. The binding of tafluprost acid to human serum albumin in vitro is 99% for 500 ng/ml tafluprost acid.
Biotransformation
The main route of metabolism of tafluprost in humans, tested in vitro, is hydrolysis to form a pharmacologically active metabolite, tafluprost acid, which is then metabolized through glucuronidation or beta-oxidation to form the pharmacologically inactive 1,2-dinor and 1,2,3,4-tetranor acids of tafluprost, which can be glucuronidated or hydroxylated. The cytochrome P450 (CYP) enzyme system is not involved in the metabolism of tafluprost acid. In a study conducted on rabbit corneal tissue with refined enzymes, it was revealed that the main esterase responsible for the ester hydrolysis of tafluprost acid is carboxylesterase. Butyrylcholinesterase, but not acetylcholinesterase, may also contribute to hydrolysis.
Removal
In a study in rats, after a single administration of 3H-tafluprost (0.005% ophthalmic solution, 5 µl/eye) in both eyes for 21 days, approximately 87% of the total radioactive dose was recovered in feces. About 27-38% of the total dose was excreted in the urine, and about 44-58% in feces.
Special instructions
Special instructions
Before starting treatment, patients should be warned about the possibility of excessive eyelash growth, darkening of the skin of the eyelids and increased pigmentation of the irises. Some of these changes may be permanent, and this may lead to differences in the appearance of the eyes if only one eye is treated.
Changes in iris pigmentation occur slowly and may remain unnoticeable for several months. Changes in eye color are observed mainly in patients with irises of mixed colors, for example, if the eyes are brown-blue, gray-brown, yellow-brown or green-brown. There is a likely risk of lifelong heterochromia if only one eye is treated.
There is no experience with tafluprost in cases of neovascular, angle-closure, narrow-angle or congenital glaucoma. There is only limited experience with tafluprost in patients with aphakia, pigmentary or pseudoexfoliative glaucoma.
Caution is recommended when treating tafluprost in patients with aphakia, pseudophakia, damaged posterior lens capsule or anterior chamber lenses, or patients with established risk factors for the development of cystoid macular edema or iritis/uveitis.
There is no experience with the use of the drug in patients with severe asthma. Therefore, patients in this group should be treated with caution.
Benzalkonium chloride, which is commonly used as a preservative in ophthalmic preparations, has been reported to cause punctate keratopathy and/or toxic ulcerative keratopathy. Since Taflotan vials contain benzalkonium chloride, careful monitoring is necessary in cases of frequent or prolonged use in patients with dry eyes, as well as in cases where the cornea is at risk.
Benzalkonium chloride may also cause eye irritation and discoloration of soft contact lenses. Contact of the drug with soft contact lenses should be avoided. Remove contact lenses before using the drug and reinsert them no earlier than 15 minutes after instillation.
Impact on the ability to drive vehicles and operate machinery
Tafluprost does not affect the ability to drive a car or operate machinery. As with any other ophthalmic drug, short-term blurred vision may occur after installation of the drug. In this case, the patient must wait until vision is fully restored before driving or operating mechanical equipment.
Active ingredient
Active ingredient
Tafluprost
Composition
Composition
1 ml eye drops contains:
active ingredients:
tafluprost 15 mcg;
excipients:
glycerol – 22.5 mg,
sodium hydrogen phosphate dihydrate – 2 mg,
disodium edetate – 0.5 mg,
polysorbate 80 – 0.75 mg,
hydrochloric acid and/or sodium hydroxide (for pH adjustment),
water for d/i – up to 1 ml.
Pregnancy
Pregnancy
Women of childbearing potential/contraception
Women of childbearing potential should not use Taflotan unless they are using adequate contraception.
Pregnancy
There is insufficient data on the use of tafluprost in pregnant women. Tafluprost may have adverse pharmacological effects on pregnancy and/or the fetus/children. Animal studies have demonstrated toxic effects on the reproductive system. Therefore, Taflotan should not be used during pregnancy unless there are no other treatment options.
Breastfeeding
It is not known whether tafluprost or its metabolites pass into human breast milk. A study in rats showed excretion of tafluprost into breast milk after topical administration. Therefore, Taflotan should not be used during breastfeeding.
Fertility
In female and male rats, mating ability and fertility remained unchanged when Tafluprost was administered up to 100 mcg/kg/day intravenously.
Contraindications
Contraindications
Hypersensitivity to tafluprost or any of Taflotan’s inert excipients.
Side Effects
Side Effects
In clinical studies, over 1,400 patients were treated with preservative tafluprost, either as monotherapy or as an add-on drug to timolol 0.5%. The most frequently reported treatment-related side effect was ocular hyperemia. It was observed in approximately 13% of patients participating in clinical trials of tafluprost in Europe and the USA. In most cases, hyperemia was moderate and led to treatment discontinuation in an average of 0.4% of patients. In a 3-month phase III study in the USA, when comparing tafluprost 0.0015% without preservative with timolol, also without preservative, ocular hyperemia was observed in 4.1% (13/320) of patients receiving Tafluprost. The following treatment-related side effects were reported during clinical trials of Tafluprost in Europe and the USA after their maximum extension to 24 months:
Ophthalmological
Common (> 1/100 to < 1/10): eye itching, eye irritation, eye pain, conjunctival/ocular hyperemia, eyelash changes (increased length, thickness and number of eyelashes), dry eye syndrome, foreign body sensation in the eye, eyelash discoloration, eyelid erythema, superficial punctate keratitis, photophobia, increased lacrimation, blurred vision, decreased visual acuity vision, and increased pigmentation of the iris.
Uncommon (> 1/1000 to < 1/100): eyelid pigmentation, eyelid swelling, asthenopia, conjunctival edema, eye discharge, blepharitis, anterior chamber inflammation, ocular discomfort, anterior chamber flare, conjunctival pigmentation, conjunctival follicles, allergic conjunctivitis, and atypical sensation in the eye.
Nervous system disorders
Common (> 1/100 to < 1/10): headache
Disorders of the skin and subcutaneous tissues
Uncommon (> 1/1000 to < 1/100): eyelid hypertrichosis
Interaction
Interaction
No cross-interactions with other drugs should be expected since systemic concentrations of tafluprost are extremely low after eye instillation. No special studies have been conducted to study the specific cross-interactions of tafluprost with other medical products.
In clinical studies, tafluprost was used concomitantly with timolol, and there was no evidence of cross-interactions.
Overdose
Overdose
Symptoms: There have been no reports of overdose.
After instilling the drug into the eye, an overdose is unlikely.
In case of overdose, treatment should be symptomatic.
Storage conditions
Storage conditions
At 2–8 °C
Shelf life
Shelf life
3 years
Manufacturer
Manufacturer
NextPharma, Finland
Additional information
| Shelf life | 3 years |
|---|---|
| Conditions of storage | At 2-8 °C |
| Manufacturer | NextPharma, Finland |
| Medication form | eye drops |
| Brand | NextPharma |
Related products
Buy Taflotan, eye drops 0.0015% 0.3 ml 30 pcs with delivery to USA, UK, Europe and over 120 other countries.