No products in the cart.
Description
Pharmacotherapeutic group: Antiviral [HIV] medicine.
ATX code:
J05AG Nenucleosides – reverse transcriptase inhibitors
J05AG03 Efavirenz
Pharmacological properties
/p>
Pharmacodynamics
Efavirenz is a non-nucleoside reverse transcriptase inhibitor (NNRTI) of HIV-1. Efavirenz is a non-competitive HIV-1 reverse transcriptase inhibitor and does not significantly inhibit HIV-2 reverse transcriptase or human cellular DNA polymerases (alpha, beta, gamma and delta).
HIV sensitivity in vitro. The clinical significance of HIV-1 sensitivity to efavirenz in vitro has not been established. The in vitro antiviral efficacy of efavirenz was evaluated on lymphoblast cell lines, peripheral blood mononuclear cells and macrophage/monocyte cultures. The concentration of efavirenz required for 90 to 95% inhibition (IC90-95) of laboratory-adapted wild-type strains and zidovudine-resistant clinical isolates ranged from 0.46 to 6.8 nmol/L.
Efavirenz showed synergistic activity in cell culture in combination with the nucleoside reverse transcriptase inhibitors (NRTIs) zidovudine and didanosine and the protease inhibitor indinavir.
Resistance. The antiviral efficacy of efavirenz in cell culture against virus strains with amino acid substitutions in the reverse transcriptase at positions 48, 108, 179, 181 or 236, as well as against strains with amino acid substitutions in the protease, was similar to that of wild-type virus strains. The only substitutions that resulted in the highest resistance to efavirenz in cell culture were the substitution of leucine for isoleucine at position 100 (L100I, 17-22-fold resistance) and lysine for asparagine at position 103 (K103N, 18-33-fold resistance). A more than 100-fold decrease in viral susceptibility to the drug was observed for HIV varieties expressing the K103N substitution in addition to other amino acid substitutions in the reverse transcriptase.
K103N is the most commonly observed substitution in reverse transcriptase in viral isolates obtained from patients who had a significant increase in viral particles after treatment withdrawal in clinical trials of efavirenz in combination with indinavir or in the combination of zidovudine with lamivudine. Substitutions in reverse transcriptase at positions 98, 100, 101, 101, 108, 138, 188, 190, and 225 were also observed, but less frequently and often only in combination with K103N. The type of amino acid substitutions in the reverse transcriptase associated with efavirenz resistance was independent of the other antiviral drugs used in combination with efavirenz.
Cross-resistance. A study of the cross-resistance profiles of efavirenz, nevirapine and delavirdine on cell cultures showed that K103N substitution results in loss of susceptibility to all three non-nucleoside reverse transcriptase inhibitors. Two of the three delavirdin-resistant clinical isolates studied had cross-resistance to efavirenz and contained the K103N substitution. The third isolate, which had a substitution in the reverse transcriptase at position 236, had no cross-resistance to efavirenz.
Viral isolates isolated from peripheral blood mononuclei of patients enrolled in clinical trials of efavirenz in whom therapy was ineffective (increased number of viral particles) were examined for susceptibility to NNRTIs. Thirteen isolates that had been previously characterized as resistant to efavirenz were also found to be resistant to nevirapine and delavirdine. Five of these NNRTI-resistant isolates were found to contain a K103N substitution or a valine to isoleucine substitution at position 108 (V1081) in the reverse transcriptase. Among the isolates tested after ineffective efavirenz therapy, three isolates remained sensitive to efavirenz on cell cultures and also had sensitivity to nevirapine and delavirdine.
The likelihood of cross-resistance between efavirenz and protease inhibitors is low because of the different target enzymes. Cross-resistance between efavirenz and nucleoside reverse transcriptase inhibitors is also unlikely due to different target binding sites and mechanisms of action.
Pharmacokinetics
Intake
In healthy volunteers, the maximum plasma concentration (Cmax) of efavirenz of 1.6 to 9.1 µM was reached 5 hours after a single oral administration of the drug at doses ranging from 100 mg to 1600 mg. A dose-dependent increase in maximum concentration (Smh) and area under the curve “concentration-time” was observed when taking the drug in doses up to 1600 mg; at the same time, there was no proportional relationship between the degree of increase in these indicators with the dose, suggesting that at higher doses absorption is reduced. The time to reach Plasma Cmax (3-5 hours) did not change after multiple doses of the drug, and the equilibrium plasma concentration was reached after 6-7 days.
In HIV-infected patients during the steady state period, the mean Cmax, minimum concentration (Cmin) and area under the concentration-time curve have a linear relationship with the daily dose. In 35 patients treated with efavirenz at a dose of 600 mg once daily, Cmax at equilibrium concentration was 12.9 ± 3.7 μM, Cmin was 5.6 ± 3.2 μM, and the area under the concentration-time curve was 184 ± 73 μM per hour.
The effect of food on absorption
Efavirenz can be taken regardless of meals. Taking efavirenz with food may increase its effects and lead to an increased incidence of adverse reactions. Bioavailability of a single dose of Efavirenz 600 mg in healthy volunteers increased by 22% and 17%, respectively, when taking the tablets with a meal with normal or high fat content compared to taking the same dose of the drug on an empty stomach. Efavirenz is recommended to be taken before bedtime on an empty stomach.
Distribution
Efavirenz is highly bound to plasma proteins (approximately 99.5 to 99.75%), primarily to albumin. In HIV-infected patients (N = 9) who received efavirenz in doses of 200 to 600 mg once a day for at least one month the drug concentration in cerebrospinal fluid was 0.26 to 1.19% (0.69% on average) of the corresponding concentration in blood plasma. This figure is approximately 3 times higher than the concentration of non-protein bound (free) fraction of efavirenz in blood plasma.
Metabolism
The clinical and in vitro studies using human liver microsomes have shown that efavirenz is metabolized primarily by the cytochrome P450 system to hydroxylated derivatives, which then bind to glucuronic acid to form glucuronides. These metabolites are mostly inactive against HIV-1. In vitro studies suggest that CYP3A4 and CYP2B6 are the main isoenzymes involved in the metabolism of efavirenz. In vitro studies showed that efavirenz in concentrations corresponding to those in plasma inhibits CYP2C9, CYP2C19 and CYP3A4 isoenzymes of cytochrome P450 system. In in vitro studies efavirenz did not inhibit CYP2E1 isoenzyme and inhibited CYP206 and CYP1A2 isoenzymes only in concentrations much higher than those in clinical practice.
Efavirenz has been shown to induce enzymes of the cytochrome P450 system, leading to induction of its own metabolism. When multiple doses of 200-400 mg per day for 10 days, a lower degree of cumulation of the drug was observed than expected (22-42% lower) and a shorter final elimination half-life of 40 – 55 hours (the elimination half-life of a single dose is 52 – 76 hours). The degree of induction of CYP3A4 isoenzyme is similar with efavirenz 400 mg and 600 mg doses. Pharmacokinetic interactive studies have shown that daily administration of efavirenz 400 mg or 600 mg in combination with indinavir does not cause a further decrease in the area under the concentration-time curve of indinavir compared to cases where a dose of efavirenz 200 mg was administered.
Efavirenz has a relatively long elimination half-life, ranging from 52 to 76 hours after a single dose and 40 to 55 hours after long-term use. Approximately 14% to 34% of the isotope-labeled dose of efavirenz is detected in the urine; less than 1% of the dose of efavirenz is excreted unchanged by the kidneys.
Pharmacokinetics in special patient groups
Hepatic impairment
. When efavirenz was administered once, a two-fold increase in its half-life was observed in one patient with severe hepatic impairment (Child-Pugh class C), indicating an increased degree of cumulation in these cases. Repeated administration of efavirenz showed no significant effect of liver damage on efavirenz pharmacokinetics in patients with mild hepatic impairment (Child-Pugh class A) compared to patients in the control group. There are currently insufficient data to conclude whether moderate to severe hepatic impairment (Child-Pugh class B and C) affects the pharmacokinetics of efavirenz (see Contraindications, Caution).
Renal Impairment
The pharmacokinetics of efavirenz in patients with renal impairment have not been studied, but because less than 1% of the dose of efavirenz is excreted unchanged by the kidneys, renal impairment should not significantly affect efavirenz excretion (see section “Cautionary Note”).
Gender and race
The pharmacokinetic parameters of efavirenz are similar in men and women as well as in patients of different racial backgrounds.
Age
There are no pharmacokinetic differences in patients 65 years of age or older and younger patients, although clinical studies of efavirenz have not included a sufficient number of patients 65 years of age or older.
Children
The use of efavirenz in children under 3 years of age and patients weighing less than 13 kg has not been studied. Pharmacokinetic parameters of efavirenz in children and adults were similar. In 49 children who received a dose of efavirenz equivalent to 600 mg (dose was calculated based on body weight), Cmax was 14.2 μM, Cmin was 5.6 μM and the area under the concentration-time curve was 218 μM per hour.
Indications
Indications
Active ingredient
Active ingredient
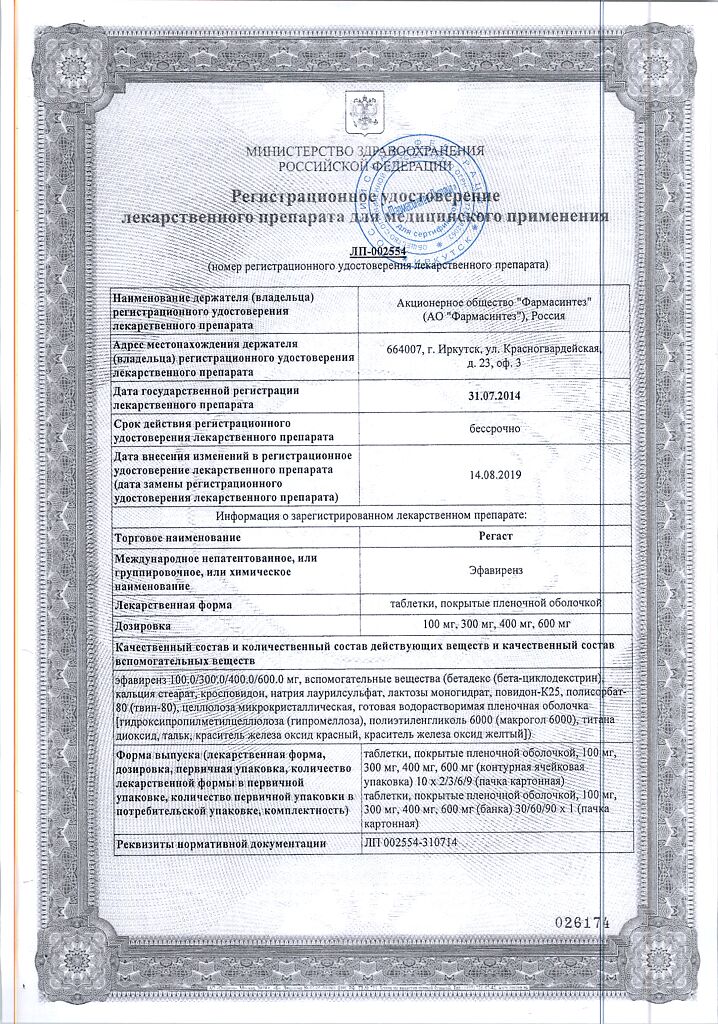
Composition
Composition
For 1 tablet:
active ingredient: Efavirenz 600 mg
excipients:
Core: Betadex (beta-cyclodextrin) – 12.0 mg; calcium stearate – 6.0 mg; crosspovidone – 72.0 mg; sodium lauryl sulfate – 21.0 mg; lactose monohydrate – 372.0 mg; povidone K 25 – 24.0 mg; polysorbate-80 (Tween 80) – 9.0 mg, microcrystalline cellulose – 54.0 mg.
Film jacket: Prepared water-soluble film jacket – 30.0 mg (Shell composition: hydroxypropyl methylcellulose (hypromellose)- 74.2%, polyethylene glycol 6000 (Macrogol 6000) – 14.3%, titanium dioxide-3.5%, talc-2.3%, iron oxide red dye-1.4%, iron oxide yellow dye-4.3%).
How to take, the dosage
How to take, the dosage
Over the mouth, the drug is recommended to be taken before going to bed on an empty stomach.
The therapy should be prescribed by a physician experienced in the treatment of HIV infection.
Adults: 600 mg once daily as part of combination therapy with protease inhibitors and/or nucleoside reverse transcriptase inhibitors (NRTIs).
Combination therapy:
When used concomitantly with rifampicin in patients with body weight 50 kg or more, the dose of efavirenz should be increased to 800 mg/day. When administered concomitantly with efavirenz no dose adjustment of rifampicin is required.
In concomitant use of efavirenz and voriconazole, the maintenance dose of voriconazole should be increased to 400 mg every 12 hours and the dose of efavirenz should be reduced to 300 mg once daily (see section “Interaction with other medicinal products”). After discontinuation of voriconazole therapy, the initial dose of efavirenz (600 mg) should be used.
Companion antiretroviral therapy: Efavirenz should be used as part of combination therapy with other antiretrovirals.
Adolescents and children with a body weight of 40 kg or more: 600 mg once daily as part of combination therapy with a protease inhibitor and/or NRTI.
Children aged 3 years and older with a body weight of 13 to 40 kg: Recommendations for use of efavirenz with a protease inhibitor and/or NRTI are in Table 1.
Table 1. Doses for children when prescribing efavirenz once daily
The use of efavirenz in children under 3 years of age and patients weighing less than 13 kg has not been studied.
Patients with renal impairment
The pharmacokinetics of efavirenz in patients with renal impairment have not been studied, but since less than 1% of the dose of efavirenz is excreted unchanged by the kidneys, renal impairment should not significantly affect efavirenz excretion (see section “Cautionary Notes. See section “Special Precautions”).
Patients with hepatic impairment
In patients with mild hepatic impairment, no dose adjustment of efavirenz is required. However, patients should be monitored for timely detection of dose-dependent adverse reactions, especially in nervous system, (see section “Special Precautions”).
In patients with moderate hepatic impairment, use of the drug is not recommended, since there is insufficient data to determine whether dose adjustment is necessary in these cases.
Interaction
Interaction
Special Instructions
Special Instructions
Efavirenz should not be used as the sole treatment for HIV infection, nor should it be added as the sole agent to an ineffective therapy regimen.
With therapy, the risk of HIV transmission to others through sexual intercourse or blood cannot be ruled out. Because of this, appropriate precautions should be taken.
The concomitant use of efavirenz with fixed combinations containing efavirenz, emtricitabine and tenofovir disoproxil fumarate is not recommended unless dose adjustments are required (e.g., when used concomitantly with rifampicin). When prescribing drugs to be taken concomitantly with efavirenz, the physician should refer to the relevant “Instructions for medical use” for these drugs. If any of the antiretrovirals in combination therapy are withdrawn due to suspected intolerance, all antiretrovirals should be considered for withdrawal at the same time. All antiretrovirals that have been withdrawn should be restarted as soon as symptoms of intolerance have disappeared.
Interrupted monotherapy followed by repeated doses of antiretrovirals is not recommended because of the increased likelihood of selection of mutagenic viruses resistant to therapy.
The use of efavirenz with Ginkgo biloba extracts is not recommended.
Efavirenz with food can increase its effects and the incidence of adverse reactions. Therefore, it is recommended that the drug be taken before going to bed on an empty stomach.
Skin rash: Clinical studies of efavirenz have reported mild to moderate rashes that usually disappear with continued therapy. Administration of appropriate H1-histamine receptor blockers and/or glucocorticosteroid drugs may improve tolerability and contribute to the early disappearance of the rash. Severe rash accompanied by blistering, desquamation or ulceration occurred in less than 1% of patients taking efavirenz. Erythema multiforme or Stevens-Johnson syndrome occurred in 0.14% of cases. If patients develop a severe rash accompanied by blistering, desquamation involving mucous membranes or fever, efavirenz should be stopped immediately. If therapy with efavirenz is discontinued, discontinuation of other antiretrovirals should be considered to avoid the emergence of therapy-resistant virus
The rash occurred in 26 of 57 children (46%) who received efavirenz for 48 weeks, with three patients experiencing a severe rash. Prescribing H1-histamine receptor blockers before starting efavirenz therapy in children to prevent rash may be appropriate.
Psychiatric symptoms: There are data on the occurrence of psychiatric adverse events in patients treated with efavirenz. Patients with a history of mental disorders are at increased risk of serious mental adverse events. There are also post-registration data on cases of suicide, delusions and psychosis-like behavior. Patients should be warned that if they develop these symptoms, they should contact their physician immediately. The physician should determine if these symptoms may be related to taking efavirenz, and if this relationship is confirmed, assess the patient’s risk to continue therapy versus the potential benefit of taking the drug (see section on Caution).
Nervous system symptoms: patients receiving efavirenz at a dose of 600 mg once daily in clinical trials often have the following symptoms: dizziness, insomnia, somnolence, decreased concentration, dream abnormalities, and other adverse events occur. Nervous system symptoms are usually observed during the first or second day of therapy and in most cases disappear after the first 2-4 weeks. Patients should be informed that such symptoms, if they occur, usually disappear with continuation of therapy and are not a sign of possible mental disorders, which are less common.
Immune reconstitution syndrome: HIV-infected patients with severe immunodeficiency may develop an inflammatory response to asymptomatic or residual opportunistic infections during initiation of antiretroviral therapy, which can cause serious deterioration or exacerbation of symptoms. Typically, such reactions occur in the first weeks or months after initiation of antiretroviral therapy. The most significant examples are cytomegalovirus retinitis, generalized and/or focal mycobacterial infection, and pneumonia caused by Pneumocystis jiroveci (formerly Pneumocystis carinii). Any symptoms of inflammation need to be identified and treated if necessary.
Autoimmune diseases (e.g., Graves’ disease) have been observed against the background of immune reconstitution, but the timing of the primary manifestations varied, and the disease could occur many months after the start of therapy. Lipodystrophy and metabolic disorders
Combination antiretroviral therapy is associated with redistribution of body fat (lipodystrophy) in HIV-infected patients, including depletion of peripheral and facial subcutaneous fat, its accumulation in the intraperitoneal space, internal organs, back of the neck (“buffalo hump”) and hypertrophy of the mammary glands. Combination antiretroviral therapy can cause metabolic abnormalities such as hypertriglyceridemia, hypercholesterolemia, insulin resistance, hyperglycemia and hyperlactatemia.
Osteonecrosis
Cases of osteonecrosis have been reported, especially in patients with common risk factors (corticosteroid use, alcohol use, acute immunosuppression, increased mass index), advanced HIV infection or on long-term combination antiretroviral therapy. Patients should be advised to see a physician if they experience joint pain, stiffness in the joints, or difficulty moving.
Patient special groups
Hepatic disorders: efavirenz is contraindicated in patients with severe hepatic impairment (Child-Pugh class C) (see section “Contraindications”) and is not recommended in patients with moderate hepatic impairment because there are insufficient data to determine whether dose adjustments are necessary in these cases. Due to the intensive metabolism of efavirenz by the cytochrome P450 system and limited clinical experience with efavirenz in patients with chronic liver disease, the drug should be administered with caution in patients with mild hepatic impairment (see section “Caution”). Patients should be monitored for the timely detection of dose-dependent adverse reactions, especially those involving the nervous system. Laboratory tests should also be performed at intervals to evaluate the liver.
The safety and efficacy of efavirenz have not been confirmed in patients with a history of significant liver impairment. Patients with chronic hepatitis B and C who are taking combination antiretroviral therapy (ART) are at risk of serious adverse liver reactions that may be fatal. Patients with a history of liver dysfunction, including chronic active hepatitis, have an increased incidence of liver dysfunction during combination ART, so such patients should be monitored according to the standard regimen. In patients with worsening liver disease or with a sustained increase in serum transaminases greater than 5 times the upper limit of normal, the benefit of continued efavirenz therapy should be weighed against the possible risk of hepatotoxicity. In these patients, consideration should be given to whether to discontinue or withdraw ART.
When concomitant use of other drugs with known hepatotoxicity, monitoring of “liver” enzyme activity is recommended. Patients with hepatitis B or C should also follow the hepatitis B or C drug prescribing instructions for use when prescribing combined antiviral therapy.
Renal impairment: The pharmacokinetics of efavirenz in patients with renal impairment have not been studied; however, since less than 1% of efavirenz is excreted unchanged by the kidneys, renal impairment should not significantly affect efavirenz excretion.
There is no experience of use in patients with severe renal impairment; therefore, monitoring to assess the safety of therapy is recommended in this group of patients when using the drug.
Elderly patients: Since a small number of elderly patients have been included in clinical trials, it is not possible to suggest that the effect of the drug in elderly patients is different from that in younger patients (see section on Pharmacokinetics).
In children: The use of efavirenz in children younger than 3 years of age or those weighing less than 13 kg has not been studied. There is evidence that the pharmacokinetics of efavirenz may be altered in very young children.
Convulsions: In patients receiving efavirenz, seizures have been observed very rarely, including patients with a history of seizures. In patients receiving concomitant anticonvulsants with preferential metabolism in the liver, such as phenytoin, carbamazepine and phenobarbital, their plasma concentrations should be monitored periodically. Caution should be exercised when prescribing the drug in patients with a history of seizures (see sections “Caution” and “Side effects”).
“Liver” enzymes: In patients with a history of diagnosed or suspected hepatitis B and C and patients taking drugs associated with toxic effects on the liver, regular monitoring of the activity of “liver” enzymes is recommended. In patients with a sustained increase in serum transaminase activity exceeding 5 times the upper limit of normal, the benefit of continued therapy with efavirenz should be weighed against the possible risk of hepatotoxicity (see section “Adverse effects”).
Cholesterol: Blood cholesterol concentrations should be monitored in patients taking efavirenz (see section on side effects).
Interaction with cannabinoid test: efavirenz does not bind to cannabinoid receptors, but there have been reports of false positive urine cannabinoid test results in uninfected volunteers receiving efavirenz. False-positive test results have only been observed with the CEDIA DAU Multi-Level TIS assay, which is used for screening, and have not been observed with other cannabinoid assays, including, tests used to confirm positive results.
Effects on driving and operating ability
There have been no studies designed to examine the effects on driving and operating ability of devices. Efavirenz may cause dizziness, impaired attention, and/or insomnia. Patients should be warned that if they develop any of these symptoms, they should avoid driving and operating devices.
Contraindications
Contraindications
Side effects
Side effects
Overdose
Overdose
Pregnancy use
Pregnancy use
Additional information
| Weight | 0.055 kg |
|---|---|
| Shelf life | 2 years. Do not use after the expiry date printed on the package. |
| Conditions of storage | In the original manufacturer's package at a temperature not exceeding 25 ° C. Keep out of reach of children. |
| Manufacturer | Pharmasintez JSC, Russia |
| Medication form | pills |
| Brand | Pharmasintez JSC |
Related products
Buy Regast, 600 mg 30 pcs. with delivery to USA, UK, Europe and over 120 other countries.