No products in the cart.
Reduxin Forte, 850 mg+10 mg 30 pcs
€70.74 €60.95
Description
Pharmacotherapeutic group
Hypoglycemic agent of oral biguanide group. An agent for the treatment of obesity.
ATX code: A08A and A10BA02
Pharmacodynamics
Metformin
. An oral hypoglycemic drug of the biguanide group, reduces hyperglycemia without resulting in hypoglycemia. Unlike sulfonylurea derivatives, it does not stimulate insulin secretion and does not cause hypoglycemic effect in healthy people. Increases the sensitivity of peripheral receptors to insulin and glucose utilization by cells. Inhibits gluconeogenesis in the liver. Delays absorption of carbohydrates in the intestine and stimulates the production of GTP-1 (physiological appetite regulator). Metformin stimulates glycogen synthesis by acting on glycogen synthase. It increases transport capacity of all types of membrane glucose transporters. In addition, it has a favorable effect on lipid metabolism: it decreases concentrations of total cholesterol, low-density lipoproteins and triglycerides.
During metformin administration body weight remains stable or decreases moderately.
Sibutramine
It is a prodrug and shows its effect in vivo due to metabolites (primary and secondary amines) that inhibit monoamine reuptake (serotonin, noradrenaline and dopamine). The increase of neurotransmitters in synapses increases the activity of central 5NT-serotonin and adrenergic receptors and contributes to the physiological regulation of appetite by increasing the feeling of satiety and reducing the need for food, as well as increasing thermoproduction (internal energy expenditure). By activating β-adrenoceptors indirectly, sibutramine affects brown adipose tissue. Reduction of body weight when taking sibutramine is accompanied by an increase in serum concentration of high density lipoproteins (HDL) and a decrease in triglycerides, total cholesterol, low density lipoproteins (LDL) and uric acid.
Sibutramine and its metabolites do not affect the release of monoamines, do not inhibit monoamine oxidase (MAO); They have no affinity to a large number of neurotransmitter receptors, including serotonin receptors (5-HT1, 5-HT1A, 5-HT1B, 5-HT2C), adrenergic (β1, β2, β3, α1, α2), dopamine (D1, D2), muscarinic, histamine (H1), benzodiazepine and glutamate NMDA receptors.
Simultaneous use of metformin and sibutramine increases the effectiveness of therapy in obese patients. By regulating appetite, reducing hunger, increasing energy expenditure and regulating lipid and carbohydrate metabolism, Reduxin® Forte reduces human body weight and restores metabolic health.
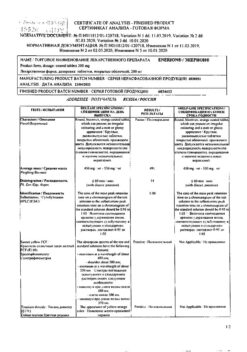
Clinical efficacy and safety (Results of clinical trials)
In a clinical trial in Reduxin® Forte group the percentage of patients who achieved clinically significant weight loss ≥5% during 3 months of therapy (early responders to therapy) exceeded 90%. During 6 months of therapy 91.67% of patients in the Reduxin® Forte group achieved a weight loss of 10% or more. The decrease of body weight was accompanied by clinically significant reduction of waist circumference and improvement of lipid profile, which proves the effectiveness of the drug in reducing the risk of complications and meets the main objectives of treatment of obesity.
No negative effect of Reduxin® Forte on the cardiovascular system parameters was observed during the study in patients with obesity.
Pharmacokinetics
absorption
After oral administration metformin is completely absorbed from the gastrointestinal tract. With concomitant food intake, metformin absorption is reduced and delayed. Absolute bioavailability is 50-60%. Maximum plasma concentration (Cmax) is approximately 2 µg/ml or 15 µmol and is reached after 2.5 hours.
Distribution
Metformin is rapidly distributed in body tissues. Virtually not bound to plasma proteins.
Metabolism
Subject to little metabolism.
Elimation
It is excreted by the kidneys. Metformin clearance in healthy subjects is 400 ml/min (4 times higher than creatinine clearance (CK)), indicating active tubular secretion.
The half-life (T1/2) is approximately 6.5 h.
Pharmacokinetics in special clinical cases
In patients with renal insufficiency T1/2 is increased, there is a risk of metformin cumulation in the body.
Sibutramine
absorption
After oral administration is rapidly absorbed from the GI tract by at least 77 %. During “primary passage” through the liver, it undergoes biotransformation under the influence of CYP3A4 isoenzyme to form two active metabolites (monodesmethylsibutramine (M1) and didesmethylsibutramine (M2)). After a single dose of 15 mg, maximum blood concentration (Cmax) of monodesmethylsibutramine (M1) is 4 ng/ml (3.2-4.8 ng/ml), didesmethylsibutramine (M2) – 6.4 ng/ml (5.6-7.2 ng/ml). Cmax is reached in 1.2 h (sibutramine), 3-4 h (active metabolites). Simultaneous intake of food decreases Cmax of metabolites by 30% and increases the time to reach it by 3 h without changing the area under the curve “concentration-time” (AUC).
Distribution
Rapidly distributed in tissues. Protein binding is 97% (sibutramine) and 94% (M1 and M2). Equilibrium concentration of active metabolites in blood is reached within 4 days after the start of treatment and is approximately 2 times higher than the concentration in plasma after a single dose.
Metabolism and excretion
Active metabolites undergo hydroxylation and conjugation to form inactive metabolites, which are excreted mainly by the kidneys. The half-life of sibutramine is 1.1 h, M1 – 14 h, M2 – 16 h.
Pharmacokinetics in special clinical cases
The currently available data do not indicate the existence of clinically significant differences in pharmacokinetics in men and women.
Pharmacokinetics in the elderly
Pharmacokinetics in elderly healthy subjects (mean age 70 years) are similar to those in young adults.
Kidney failure
Renal failure has no effect on the AUC of active metabolites M1 and M2, except for metabolite M2 in patients with end-stage renal failure on dialysis.
Hepatic failure
Patients with moderate hepatic failure after a single dose of sibutramine have a 24% higher AUC of active M1 and M2 metabolites than in healthy subjects.
Indications
Indications
Reduxin® Forte is indicated for correction of body weight and improvement of lipid and carbohydrate metabolism in patients:
- with a body mass index (BMI) greater than 30 kg/m2 (alimentary obesity);
- with a BMI of 27 kg/m2 or more in combination with type 2 diabetes and dyslipidemia;
.
Active ingredient
Active ingredient
Metformin, Sibutramine
Composition
Composition
Each 850 mg + 10 mg tablet contains:
Active ingredients:
metformin hydrochloride, 850.0 mg; sibutramine hydrochloride monohydrate, 10.0 mg;
Auxiliary substances:
Microcrystalline cellulose, croscarmellose sodium, povidone K-25, magnesium stearate;
Sheet film excipients:
Prepared coating system Opadray II 85F30656 blue (polyvinyl alcohol, macrogol, titanium dioxide, talc, brilliant blue dye with aluminum varnish, indigo carmine dye with aluminum varnish, iron oxide yellow dye).
Each tablet with a dosage of 850 mg + 15 mg containsit:
Active ingredients:
metformin hydrochloride, 850.0 mg; sibutramine hydrochloride monohydrate, 15.0 mg;
Auxiliary substances:
Microcrystalline cellulose, croscarmellose sodium, povidone K-25, magnesium stearate;
Sheet film excipients:
Prepared coating system Opadray II 85F48105 white (polyvinyl alcohol, macrogol, talc, titanium dioxide).
How to take, the dosage
How to take, the dosage
The drug Reduxin® Forte is administered orally once a day. The dose is set individually depending on tolerability and clinical efficacy.
The recommended initial dose is 850 mg + 10 mg per day.
The drug should be taken in the morning, without chewing and with plenty of fluid (a glass of water). The drug can be taken both on an empty stomach and in combination with a meal. The dose can be increased up to 850 mg + 15 mg, if during a month the body weight loss by 2 kg or more has not been achieved, but not earlier than after 4 weeks from the beginning of the treatment.
Treatment with Reduxin® Forte should not be continued for more than 3 months in patients who didn’t achieve 5 % of body weight reduction from the initial level when taking the drug in maximum dose within 3 months.
In patients with obesity without additional carbohydrate metabolism disorders Reduxin® Forte administration is recommended during 6 months in order to develop correct eating habits and maintain the achieved result of weight loss.
Treatment with Reduxin® Forte should not be continued if during the further therapy after the achieved weight loss the patient again gains 3 kg or more in body weight.
Long-term use of the drug is recommended to reduce body weight by 5-10% and maintain the result, which reduces health risks and improves the course of diseases associated with obesity.
Treatment with Reduxin® Forte should be combined with diet and physical exercises under the supervision of a physician with practical experience in the treatment of obesity.
The duration of continuous treatment should not exceed 1 year.
Interaction
Interaction
Metformin
Contraindicated combinations
Iodine-containing radiopaque agents: Against a background of functional renal insufficiency in diabetic patients, radiological examination with iodine-containing radiopaque contrast agents may cause the development of lactoacidosis. Metformin should be discontinued depending on renal function 48 hours before or at the time of radiology with iodine-containing radiopaque agents and not resumed until 48 hours after the study, provided that renal function has been assessed as normal during the examination.
Unrecommended combinations
Alcohol: acute alcohol intoxication increases the risk of lactoacidosis, especially in cases:
- insufficient diet, following a low-calorie diet;
- hepatic insufficiency.
Alcohol and medications containing ethanol should be avoided while taking the drug.
Combinations requiring caution
Danazol: Simultaneous administration of danazol is not recommended to avoid the hyperglycemic effects of the latter. If treatment with danazolol is necessary and after discontinuation of the latter, metformin dose adjustment is required with monitoring of blood glucose concentrations.
Chlorpromazine: when taken in high doses (100 mg per day) increases blood glucose concentration, reducing insulin release. When treating with neuroleptics and after discontinuation of the latter it is required to correct the dose of the drug under control of blood glucose concentration.
Glucocorticosteroids (GCS) of systemic and local action decrease glucose tolerance and increase blood glucose concentration, sometimes causing ketosis. Metformin dose adjustment is required during treatment with GCS and after discontinuation of GCS under control of blood glucose concentration.
Diuretics: concomitant use of “loop” diuretics may lead to lactoacidosis due to possible functional renal failure. Metformin should not be administered if IQ is below 60 mL/min.
Beta2-adrenomimetics administered as injections: increase blood glucose concentration due to beta2-adrenoreceptor stimulation. In this case it is necessary to control blood glucose concentration. If necessary, the prescription of insulin is recommended.
In case of concomitant use of the above drugs, more frequent monitoring of blood glucose concentrations may be required, especially at the beginning of treatment. If necessary, the dose of metformin may be adjusted during treatment and after discontinuation.
Angiotensin-converting enzyme inhibitors and other hypotensive drugs may decrease blood glucose concentration. If necessary, the dose of metformin should be adjusted.
Phenothiazides, glucagon, estrogens, oral contraceptives, phenytoin, sympathomimetics, nicotinic acid, isoniazid, “slow” calcium channel blockers, levothyroxine sodium may decrease the hypoglycemic effect of metformin. Concomitant use with cimetidine reduces the excretion rate of metformin, which may lead to lactoacidosis. In healthy volunteers, concomitant use of metformin and propranolol, as well as when using metformin and ibuprofen, no changes in their pharmacokinetic parameters were observed. Metformin may decrease the effect of indirect anticoagulants.
Organic cation transporter substrates 1 and 2 (OCT1 AND OCT2)
Metformin is a substrate of organic cations OCT1 and OCT2. When co-administered with metformin:
- OST1 inhibitors (such as verapamil) may decrease the hypoglycemic effects of metformin.
- OST1 inducers (such as rifampicin) may increase gastrointestinal absorption of metformin and increase its hypoglycemic effects.
- OST2 inhibitors (such as cimetidine, dolutegravir, ranolazine, trimethoprim, vandetanib, izavuconazole) may decrease the renal excretion of metformin and lead to increased plasma concentrations.
OCT1 and OCT2 inhibitors (such as crizotinib, olaparide) may decrease the hypoglycemic effects of metformin.
Concomitant use of metformin with sulfonylurea derivatives, insulin, acarbose, salicylates may cause hypoglycemia.
Nifedipine increases absorption and Cmax of metformin.
Cationic drugs (amiloride, digoxin, morphine, procainamide, quinidine, quinine, ranitidine, triamterene, trimethoprim and vancomycin) that are secreted in the renal tubules compete with metformin for tubular transport systems and may increase its Cmax.
Sibutramine
Microsomal oxidation inhibitors, including CYP3A4 isoenzyme inhibitors (ketoconazole, erythromycin, cyclosporine, etc.) increase plasma concentrations of sibutramine metabolites with increased heart rate and clinically insignificant increase of QT interval.
Rifampicin, macrolide antibiotics, phenytoin, carbamazepine, phenobarbital and dexamethasone may accelerate metabolism of sibutramine.
The simultaneous use of several drugs that increase serotonin plasma levels can lead to serious interactions. So-called serotonin syndrome may develop in rare cases with concomitant use of sibutramine with selective serotonin reuptake inhibitors (drugs for treatment of depression), with some drugs for treatment of migraine (sumatriptan, dihydroergotamine), with potent analgesics (pentazocine, pethidine, fentanyl), or anti-cough drugs (dextromethorphan). Sibutramine does not affect the effect of oral contraceptives.
In concomitant use of sibutramine and alcohol no increase in the negative effects of alcohol has been noted. However, alcohol is absolutely not combined with the recommended dietary measures when taking sibutramine.
When concomitant use with sibutramine of other drugs affecting hemostasis or platelet function, the risk of bleeding increases. Drug interaction when using sibutramine concomitantly with drugs that increase blood pressure and heart rate has not been fully studied. This group of drugs includes decongestants, anti-cough, anti-inflammatory and anti-allergic drugs containing ephedrine or pseudoephedrine. Therefore, caution should be exercised when taking these drugs concomitantly with sibutramine.
The co-administration of sibutramine with weight loss drugs acting on the central nervous system or drugs for the treatment of mental disorders is contraindicated.
Special Instructions
Special Instructions
Lactoacidosis
Lactoacidosis is a rare but serious (high mortality in the absence of emergency treatment) complication that can occur due to metformin cumulation. Cases of lactoacidosis when taking metformin occurred mainly in diabetic patients with severe renal insufficiency.
Other associated risk factors such as decompensated diabetes mellitus, ketosis, prolonged fasting, alcoholism, liver failure, and any condition associated with severe hypoxia should be considered. This may help reduce the incidence of lactoacidosis.
The risk of lactoacidosis should be considered if nonspecific signs such as muscle cramps accompanied by dyspeptic symptoms, abdominal pain and marked asthenia are present. Lactoacidosis is characterized by acidotic dyspnea, abdominal pain, and hypothermia, followed by coma. Diagnostic laboratory indicators are decreased blood pH (less than 7.25), plasma lactate content over 5 mmol/L, elevated anion gap and lactate/pyruvate ratio. If metabolic acidosis is suspected, discontinue the drug and consult a physician immediately.
Surgery
The use of Reduxin® Forte should be discontinued 48 h before elective surgery and can be continued not earlier than 48 h after on condition that renal function was found normal during the examination.
Kidney function
Since metformin is excreted by the kidneys, CK should be determined before starting Reduxin® Forte and regularly thereafter: At least once a year in patients with normal renal function, and 2-4 times a year in elderly patients, as well as in patients with CK at the lower limit of normal.
Particular caution should be exercised if renal function may be impaired in elderly patients, if hypotensive drugs, diuretics or non-steroidal anti-inflammatory drugs are used concomitantly.
Patients are advised to continue on a diet with even carbohydrate intake during the day. Patients with excessive body weight are recommended to continue a hypocaloric diet (but not less than 1000 kcal/day).
It is recommended to perform regular standard laboratory tests to control diabetes.
Caution is recommended when using Reduxin® Forte in combination with insulin or other hypoglycemic agents (including sulfonyl derivatives.
Treatment with Reduxin® Forte should be performed within a complex therapy of weight loss under the supervision of a physician with practical experience in the treatment of obesity. Complex therapy includes changes in diet and lifestyle as well as increasing physical activity. An important component of therapy is to create the prerequisites for lasting changes in eating habits and lifestyle, which are necessary to maintain the achieved weight loss even after withdrawal of drug therapy. As part of therapy with Reduxin® Forte patients need to change their lifestyle and habits in such a way that after treatment completion to ensure the maintenance of the achieved weight loss. Patients should clearly understand that failure to comply with these requirements will lead to repeated weight gain and repeated visits to the attending physician.
Blood pressure and heart rate should be measured in patients taking Reduxin® Forte. During the first 3 months of treatment these parameters should be checked every 2 weeks, and then monthly. If during two consecutive visits an increase in resting heart rate ≥10 beats per minute or systolic/diastolic pressure ≥10 mm Hg is detected, the treatment should be stopped. In patients with arterial hypertension whose blood pressure is above 145/90 mm Hg during hypotensive therapy, this monitoring should be performed particularly carefully and, if necessary, at shorter intervals. In patients whose blood pressure exceeded 145/90 mm Hg twice during repeated measurements, treatment with Reduxin® Forte should be suspended (see section “Side effects”, subsections “Cardiac disorders”, “Vascular disorders”).
In patients with sleep apnea syndrome it is necessary to monitor the blood pressure especially carefully.
Special attention is required during simultaneous administration of QT interval prolonging drugs. These drugs include H1-histamine receptor blockers (astemizole, terfenadine); antiarrhythmic drugs that prolong the QT interval (amiodarone, quinidine, flecainide, mexiletine, propafenone, sotalol); gastrointestinal motility stimulator cisapride; pimozide, sertindol and tricyclic antidepressants. This also refers to conditions that may cause prolongation of QT interval, such as hypokalemia and hypomagnesemia (see section “Interaction with other medicinal products”).
The interval between taking MAO inhibitors (including furazolidone, procarbazine, selegiline) and Reduxin® Forte should be at least 2 weeks.
Although there is no established relation between sibutramine intake and development of primary pulmonary hypertension, however, taking into account well-known risks of drugs of this group, special attention should be paid to such symptoms as progressive dyspnea (respiratory distress), chest pain and leg edema during regular medical monitoring.
In case of missed dose of the drug Reduxin® Forte double dose should not be taken at the next dose, it is recommended to continue further administration of the drug according to the prescribed scheme.
In coadministration of sibutramine and other serotonin reuptake inhibitors there is an increased risk of bleeding. Sibutramine should be used with caution in patients prone to bleeding, as well as those taking drugs that affect hemostasis or platelet function.
Although there are no clinical data on addiction to sibutramine, one should find out whether the patient has a history of drug dependence, and pay attention to possible signs of drug abuse.
Impact on ability to drive vehicles and mechanisms
Administration of Reduxin® Forte may limit the ability to drive vehicles and mechanisms. During the use of the drug Reduxin® Forte, caution should be exercised when driving vehicles and engaging in other potentially dangerous activities that require high concentration and speed of psychomotor reactions.
.
Synopsis
Synopsis
Dosage 850 mg + 10 mg
Biconvex oval tablets with a separating ridge on one side, coated with a blue film. Cross section shows almost white kernel.
Dosage 850 mg + 15 mg
Biconvex oval tablets with a separating line on one side, coated with white film. On the cross section the core is almost white.
Contraindications
Contraindications
- high sensitivity to the drug’s components;
- diabetic ketoacidosis, diabetic precoma, diabetic coma;
- renal dysfunction (creatinine clearance (CK) less than 45 ml/min;
- liver dysfunctionRenal dysfunction (creatinine clearance (CK) less than 45 ml/min);
- disordered liver function;
- acute conditions with risk of renal dysfunction: Dehydration (in diarrhea, vomiting), severe infectious diseases, shock;
- cardiovascular disease (history and current): coronary heart disease (myocardial infarction (MI), angina pectoris), chronic heart failure in decompensation, peripheral artery occlusive disease, tachycardia, arrhythmia, cerebrovascular disease (stroke, transient cerebrovascular disorders);
- Uncontrolled arterial hypertension (blood pressure (BP) above 145/90 mmHg). hypertension (BP over 145/90 mm Hg) (see also Cautions);
- clinically manifest acute and chronic diseases that can lead to tissue hypoxia (e.g. respiratory failure, heart failure, acute MI);
- chronic alcoholism, acute ethanol poisoning;
- thyrotoxicosis;
- doble prostatic hyperplasia;
- pheochromocytoma;
- closed-angle glaucoma;
- extensive surgical operations and trauma (when insulin therapy is indicated)
- lactoacidosis (incl.ч.
- Pregnancy and breastfeeding;
- Above 18 years of age or older than 65 years;
- Period less than 48 hours before and 48 hours after radioisotopic or radiological studies with iodine contrast media;
- Hypocaloric diet (less than 1000 kcal/d);
- presence of organic causes of obesity (e.g., hypothyroidism);
- serious eating disorders – anorexia nervosa or bulimia nervosa;
- psychiatric illness;
- Gilles de la Tourette syndrome (generalized tics);
- concurrent use of MAO inhibitors (e.g., phentermine, fenfluramine, dexfenfluramine, ethylamphetamine, ephedrine) or their use for 2 weeks before and 2 weeks after sibutramine is finished taking Other drugs acting on the central nervous system that inhibit serotonin reuptake (e.g., antidepressants, neuroleptics); tryptophan pills; and other centrally acting drugs for weight loss or treatment of mental disorders.
With caution
The drug should be used in the following conditions: history of arrhythmias; chronic circulatory insufficiency; coronary artery disease (including in anamnesis), except coronary heart disease (MI, angina pectoris); glaucoma, except for closed-angle glaucoma; cholelithiasis; arterial hypertension (controlled and in anamnesis); neurological disorders, including mental retardation and seizures (including in anamnesis).history); epilepsy; renal dysfunction (CK 45-59 ml/min); motor and verbal tics in the history; susceptibility to bleeding; disorders of blood clotting; taking drugs that affect hemostasis or platelet function; people over 60 years who perform heavy physical work, due to the increased risk of lactoacidosis.
Side effects
Side effects
Definition of frequency of side effects: very frequently (³1/10), frequently (³1/100, < 1/10), infrequently (³1/1000, < 1/100), rarely (³1/10 000,
< 1/1000), very rarely (< 1/10 000). Side effects are presented in decreasing order of importance.
Metformin
Metabolic and nutritional disorders: very rare – lactoacidosis; with prolonged use, decreased absorption of vitamin B12 is possible. Decrease of concentration of vitamin B12 must be taken into account in patients with megaloblastic anemia.
Nervous system disorders: often – disorders of taste.
Gastrointestinal disorders: very often – nausea, vomiting, diarrhea, abdominal pain, lack of appetite. These symptoms most often occur during the initial period of treatment and in most cases spontaneously disappear. Slowly increasing the dose may improve gastrointestinal tolerance.
Hepatic and biliary tract disorders: very rare – hepatic impairment, hepatitis, after cancellation of metformin these adverse events disappear completely.
Skin and subcutaneous tissue disorders: very rare – skin reactions such as erythema, itching, rash.
Sibutramine
The most frequent side effects occur at the beginning of treatment (in the first 4 weeks). Their severity and frequency lessen over time. Side effects are generally mild and reversible.
Nervous system disorders: very often – dry mouth and insomnia, often – headache, dizziness, anxiety, paresthesia, as well as changes in taste.
Chronic disorders: often – tachycardia, palpitations.
Vascular disorders: increase in blood pressure, vasodilation. A moderate increase of resting blood pressure by 1-3 mm Hg and a moderate increase of pulse by 3-7 beats per minute are observed. In some cases, a more pronounced increase in blood pressure and increased heart rate are not excluded. Clinically significant changes in blood pressure and pulse are mostly registered at the beginning of treatment (during the first 4-8 weeks). Gastrointestinal tract disorders: very often – loss of appetite and constipation, often – nausea and exacerbation of hemorrhoids. With a tendency to constipation in the first few days you need to monitor the evacuatory function of the intestine. If constipation occurs, stop taking it and take a laxative.
Skin and subcutaneous tissue disorders: often – increased sweating.
In single cases during treatment with sibutramine the following adverse clinically significant events have been described: Dysmenorrhea, edema, flu-like syndrome, skin itching, back pain, abdominal pain, paradoxical increase in appetite, thirst, rhinitis, depression, somnolence, emotional lability, anxiety, irritability, nervousness, acute interstitial nephritis, bleeding, Schoenlein-Henoch purpura (skin hemorrhages), seizures, plateletopenia, transient increase in activity of “liver” enzymes in blood.
The use of Reduxin® Forte in patients with high blood pressure: see sections “Contraindications” and “Cautions”.
In post-marketing studies of sibutramine, additional adverse reactions have been described, listed below by organ system:
Immune system disorders: hypersensitivity reactions (from mild skin rashes and urticaria to angioedema (Quincke’s edema) and anaphylaxis).
Mental disorders: psychosis, suicidal ideation, suicide and mania. If these conditions occur, the drug should be discontinued.
Nervous system disorders: convulsions, short-term memory disorders. Visual disorders: blurred vision (“shroud before eyes”). Cardiac disorders: atrial fibrillation.
Gastrointestinal disorders: diarrhea, vomiting.
Skin and subcutaneous tissue disorders: alopecia.
Renal and urinary tract disorders: urinary retention.
Gender and mammary gland disorders: disorders of ejaculation/orgasm, impotence, menstrual cycle disorders, uterine bleeding.
.
Overdose
Overdose
Metformin
Symptoms: At a dose of 85 g of metformin (42.5 times the maximum daily dose) no hypoglycemia was observed, but the development of lactoacidosis was noted.
Significant overdose or associated risk factors can lead to the development of lactoacidosis.
Treatment: In case of signs of lactocidosis the drug treatment should be stopped immediately, the patient should be urgently hospitalized and, after determining the lactate concentration, the diagnosis should be confirmed. The most effective measure for elimination of lactate and metformin from the body is hemodialysis. Asymptomatic treatment is also carried out.
Sibutramine
There are extremely limited data on sibutramine overdose. The most common adverse reactions associated with overdose are: tachycardia, increased blood pressure, headache, dizziness. It is necessary to inform your attending physician in case of suspected overdose.
Treatment: there is no specific treatment or antidotes. It is necessary to perform general measures: to ensure free breathing, to monitor the state of the cardiovascular system, as well as, if necessary, to carry out supportive symptomatic therapy. Timely use of activated charcoal, as well as gastric lavage can reduce sibutramine intake into the body. Patients with high blood pressure and tachycardia may be prescribed β-adrenoblockers. The effectiveness of forced diuresis or hemodialysis has not been established. In case of overdose, the drug Reduxin® Forte should be stopped immediately.
Pregnancy use
Pregnancy use
Since there are not enough conclusive studies on the safety of the effect of sibutramine on the fetus, this drug is contraindicated during pregnancy. Women of reproductive age should use contraceptives while taking the drug Reduxin® Forte.
It is contraindicated to use the drug Reduxin® Forte during breast-feeding.
Additional information
| Weight | 0.063 kg |
|---|---|
| Shelf life | 3 years. Do not use after the expiration date. |
| Conditions of storage | Store in a place protected from light at a temperature not exceeding 25 °С. The drug should be kept out of reach of children. Sibutramine belongs to the list of potent substances, approved by Decree of the Government of the Russian Federation of 29.12.2007 № 964. . |
| Manufacturer | Biokhimik JSC, Russia |
| Medication form | pills |
| Brand | Biokhimik JSC |
Other forms…
Related products
Buy Reduxin Forte, 850 mg+10 mg 30 pcs with delivery to USA, UK, Europe and over 120 other countries.