No products in the cart.
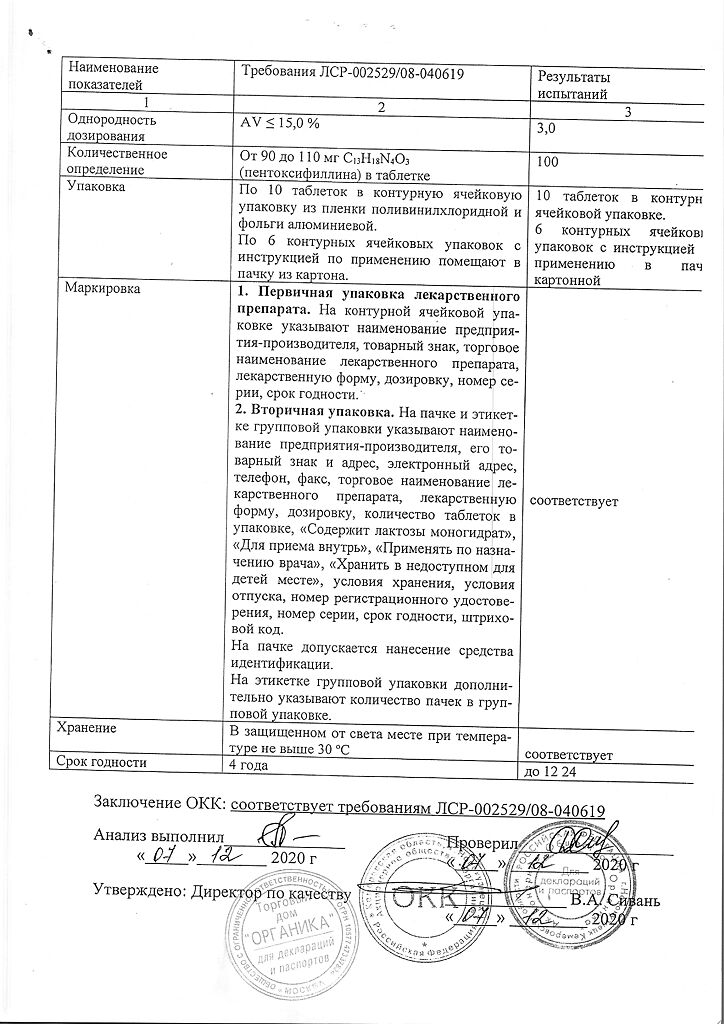
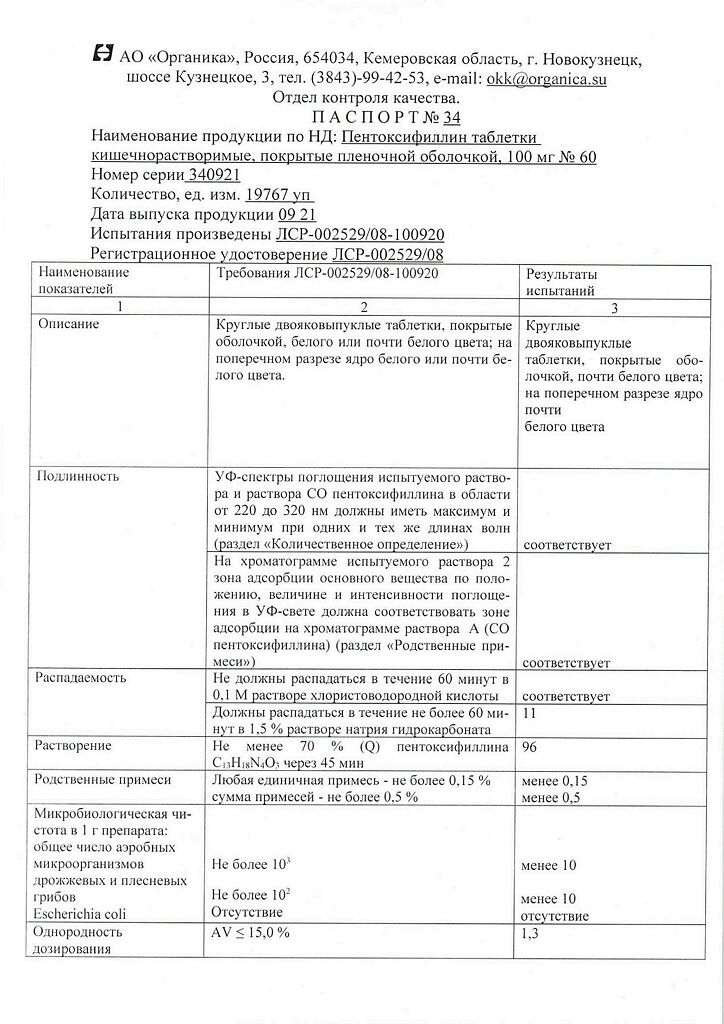
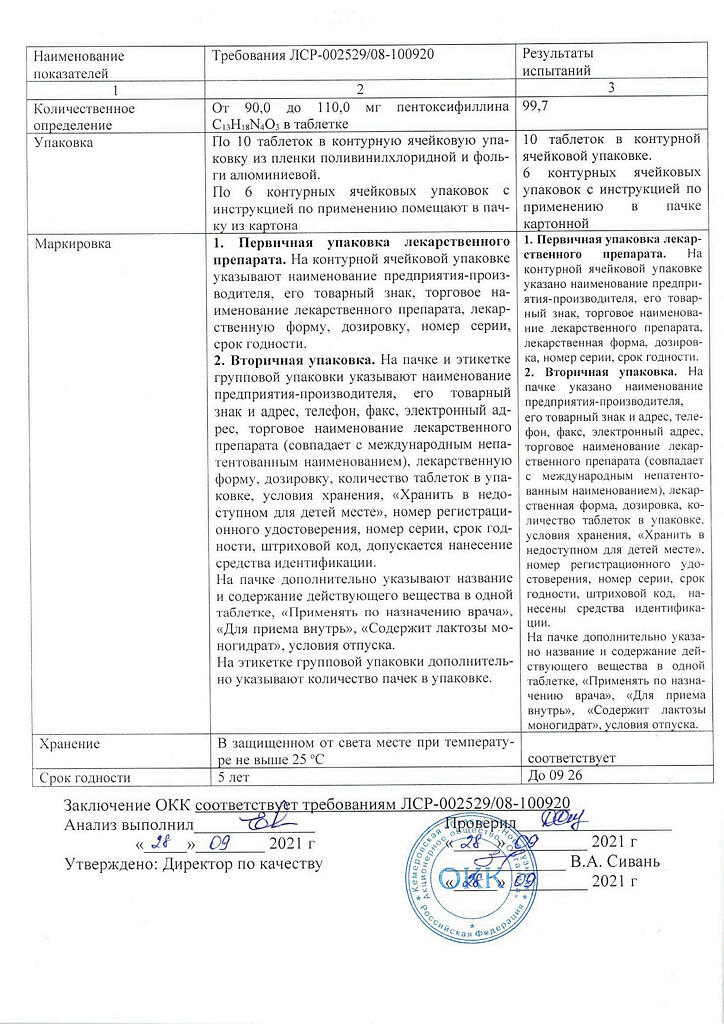
Pentoxifylline, 100 mg 60 pcs
€6.18 €5.15
Description
Pentoxifylline is a derivative of xanthine. It improves microcirculation and rheological properties of blood. The mechanism of action is associated with inhibition of phosphodiesterase and increase of cyclic 3,5 adenosine monophosphate (3,5-AMP) in platelets and adenosine triphosphate (ATP) in red blood cells with simultaneous saturation of energy potential, which in turn leads to vasodilation, reduction of total peripheral vascular resistance, increase of systolic and minute blood volume without significant change in heart rate.
Dilating coronary arteries increases oxygen delivery to the myocardium (minor antianginal effect), pulmonary vessels – improves blood oxygenation.
In intravenous administration leads to increased collateral circulation, increasing the volume of blood flowing through the unit section.
Limits blood viscosity, causes platelet disaggregation, increases the elasticity of red blood cells (by influencing the pathologically altered deformability of red blood cells). Improves microcirculation in areas of impaired circulation.
In case of occlusive lesions of the peripheral arteries (“intermittent” claudication), leads to the prolongation of walking distance, eliminates night cramps of the calf muscles and pain at rest.
Pharmacokinetics
The drug is rapidly metabolized in the liver after administration. During metabolism two main metabolites are formed: 1-(5-hydroxyhexyl)-3,7-dimethylxanthine (metabolite I) and 1-(3-carboxypropyl)-3,7-dimethylxanthine (metabolite V), which have similar activity to pentoxifylline. In 1.5-2 hours after infusion, plasma concentrations of metabolites I and V are, respectively, 5 and 8 times higher than those of the parent substance. By 8 hours the concentration of pentoxifylline and its metabolites in blood is significantly reduced (up to 10% of the initial).
The elimination half-life is from 30 minutes to 1.5 hours. It is excreted mainly by the kidneys (94%) in the form of metabolites (mainly metabolite V), by the intestine (4%). 90% of the dose is excreted during the first 4 hours. 2% of the drug is excreted unchanged. Pentoxifylline and its metabolites do not bind to plasma proteins.
It is excreted with the breast milk.
In severe renal dysfunction, excretion of the metabolites is delayed. In impaired liver function, prolongation of the elimination half-life and increased bioavailability are noted.
Indications
Indications
peripheral circulatory disorders caused by atherosclerosis, diabetes mellitus (diabetic angiopathy);
chronic cerebrovascular accidents of ischemic origin;
atherosclerotic and dyscirculatory encephalopathies; angiopathy (paresthesia, Raynaud’s disease);
trophic tissue disorders due to impaired arterial or venous microcirculation (trophic ulcers, postthrombophlebitic syndrome, frostbite, gangrene);
obliterating endarteritis;
acute, subacute and chronic circulatory failure in the retina or choroid;
hearing impairment of vascular origin.
Pharmacological effect
Pharmacological effect
Pentoxifylline is a xanthine derivative. Improves microcirculation and rheological properties of blood. The mechanism of action is associated with inhibition of phosphodiesterase and an increase in the content of cyclic 3,5 adenosine monophosphate (3,5-AMP) in platelets and adenosine triphosphate (ATP) in erythrocytes with simultaneous saturation of energy potential, which in turn leads to vasodilation, a decrease in total peripheral vascular resistance, an increase in systolic and minute blood volume without a significant change in heart rate.
By expanding the coronary arteries, it increases the delivery of oxygen to the myocardium (minor antianginal effect), and the blood vessels of the lungs improve blood oxygenation.
When administered intravenously, it leads to increased collateral circulation and an increase in the volume of blood flowing through a sectional unit.
Reduces blood viscosity, causes platelet disaggregation, increases the elasticity of red blood cells (due to the effect on the pathologically altered deformability of red blood cells). Improves microcirculation in areas of poor circulation.
With occlusive lesions of the peripheral arteries (“intermittent” claudication), it leads to an increase in walking distance, elimination of night cramps of the calf muscles and pain at rest.
Pharmacokinetics
The drug after administration is quickly metabolized in the liver. During the metabolism, two main metabolites are formed: 1-(5-hydroxyhexyl)-3,7-dimethylxanthine (metabolite I) and 1-(3-carboxypropyl)-3,7-dimethylxanthine (metabolite V), which have activity similar to pentoxifylline. 1.5-2 hours after infusion, the concentration of metabolites I and V in the blood plasma is, respectively, 5 and 8 times higher than the concentration of the original substance. By the 8th hour, the concentration of pentoxifylline and its metabolites in the blood decreases significantly (up to 10% of the initial value).
The half-life is from 30 minutes to 1.5 hours. It is excreted mainly by the kidneys (94%) in the form of metabolites (mainly metabolite V), and by the intestines (4%). in the first 4 hours up to 90% of the dose is eliminated. 2% of the drug is excreted unchanged. Pentoxifylline and its metabolites do not bind to plasma proteins.
Excreted in breast milk.
In severe renal impairment, the elimination of metabolites is slowed down. If liver function is impaired, there is an increase in half-life and increased bioavailability.
Active ingredient
Active ingredient
Pentoxifylline
Composition
Composition
Active ingredient:
pentoxifylline – 100 mg;
Excipients:
milk sugar (lactose),
potato starch,
stearic acid,
polyvinylpyrrolidone (povidone),
copolymer methacrylic acid – ethyl acrylate 1: 1 (collicut MAE-100 R),
macrogol-4000 (polyethylene oxide-4000),
talc,
titanium dioxide pigment (titanium dioxide),
azorubine (carmoisine)
Contraindications
Contraindications
Hypersensitivity to pentoxifylline, other methylxanthine derivatives or other ingredients of the finished dosage form, Porphyria; acute myocardial infarction; massive bleeding; hemorrhages in the retina of the eye; cerebral hemorrhage, acute hemorrhagic stroke; severe coronary or cerebral atherosclerosis; severe heart rhythm disturbances; pregnancy; breastfeeding period; age under 18 years (efficacy and safety have not been established).
With caution: the drug is prescribed to patients with atherosclerosis of the cerebral and/or coronary vessels, especially in cases of arterial hypotension and cardiac arrhythmias, heart failure, and liver failure. You should also be careful when prescribing Pentoxifylline to patients with peptic ulcers of the stomach and duodenum, and to patients who have recently undergone surgery (risk of bleeding).
For patients with labile blood pressure and a tendency to arterial hypotension and patients with severe renal impairment, the dose is increased gradually and selected individually
Side Effects
Side Effects
From the central nervous system: headache, dizziness; anxiety, sleep disorders; convulsions.
From the skin and subcutaneous tissue: hyperemia of the facial skin, “flushes” of blood to the skin of the face and upper chest, swelling, increased fragility of nails.
From the digestive system: dry mouth, decreased appetite, intestinal atony, exacerbation of cholecystitis, cholestatic hepatitis.
From the senses: blurred vision, scotoma.
From the cardiovascular system: tachycardia, arrhythmia, cardialgia, progression of angina, decreased blood pressure.
From the hematopoietic organs and hemostasis system: thrombocytopenia, leukopenia, pancytopenia, hypofibrinogenemia; bleeding from blood vessels of the skin, mucous membranes. stomach, intestines.
Allergic reactions: itching, skin hyperemia, urticaria, angioedema, anaphylactic shock.
Laboratory indicators: increased activity of liver transaminases (ALT, AST, LDH) and alkaline phosphatase.
Interaction
Interaction
Pentoxifylline enhances the effect of heparin, fibrinolytic drugs, theophylline, antihypertensive and hypoglycemic agents (both insulin and oral hypoglycemic agents).
Pentoxifylline may enhance the effect of drugs that affect the blood coagulation system (indirect and direct anticoagulants, thrombolytics), antibiotics (including cephalosporins – cefamandole, cefoperazone, cefotetan), valproic acid.
Cimetidine increases the concentration of pentoxifylline in the blood plasma (risk of side effects).
Co-administration with other xanthines may lead to excessive nervous agitation in patients.
Overdose
Overdose
Symptoms: nausea, dizziness, cyanosis, tachycardia, marked decrease in blood pressure, redness of the skin, increased body temperature (chills), agitation, areflexia, tonic-clonic convulsions, vomiting “coffee grounds,” arrhythmias, loss of consciousness.
Treatment: symptomatic. Particular attention should be paid to maintaining blood pressure and respiratory function. Convulsions are relieved by administering diazepam. Urgent measures in case of severe anaphylactic reactions (shock):
when primary symptoms appear (sweating, nausea, cyanosis), immediately stop taking the drug;
in addition to other necessary measures, ensure a lower position of the head and upper body and provide freedom for breathing;
urgent medical measures: administer intravenous epinephrine (adrenaline). If necessary, the administration of epinephrine can be repeated.
Storage conditions
Storage conditions
In a dry place, at a temperature not exceeding 30°C.
Shelf life
Shelf life
3 years
Manufacturer
Manufacturer
Organika, Russia
Additional information
| Shelf life | 3 years |
|---|---|
| Conditions of storage | In a dry place, at a temperature not exceeding 30 ° C. |
| Manufacturer | Organika, Russia |
| Medication form | enteric soluble tablets |
| Brand | Organika |
Other forms…
Related products
Buy Pentoxifylline, 100 mg 60 pcs with delivery to USA, UK, Europe and over 120 other countries.