No products in the cart.
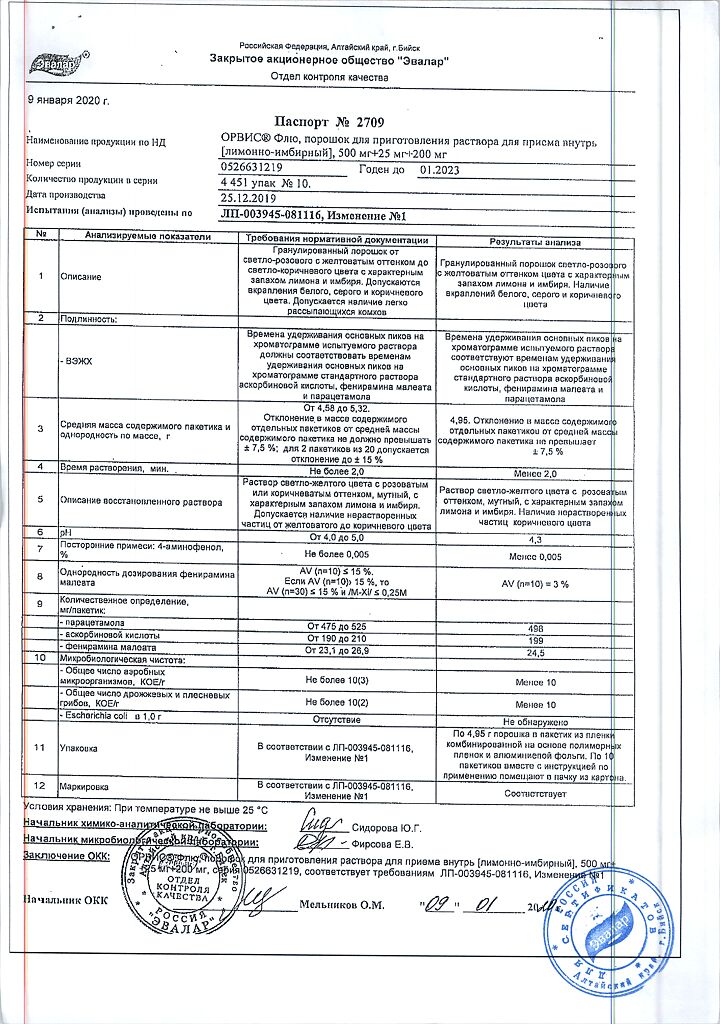
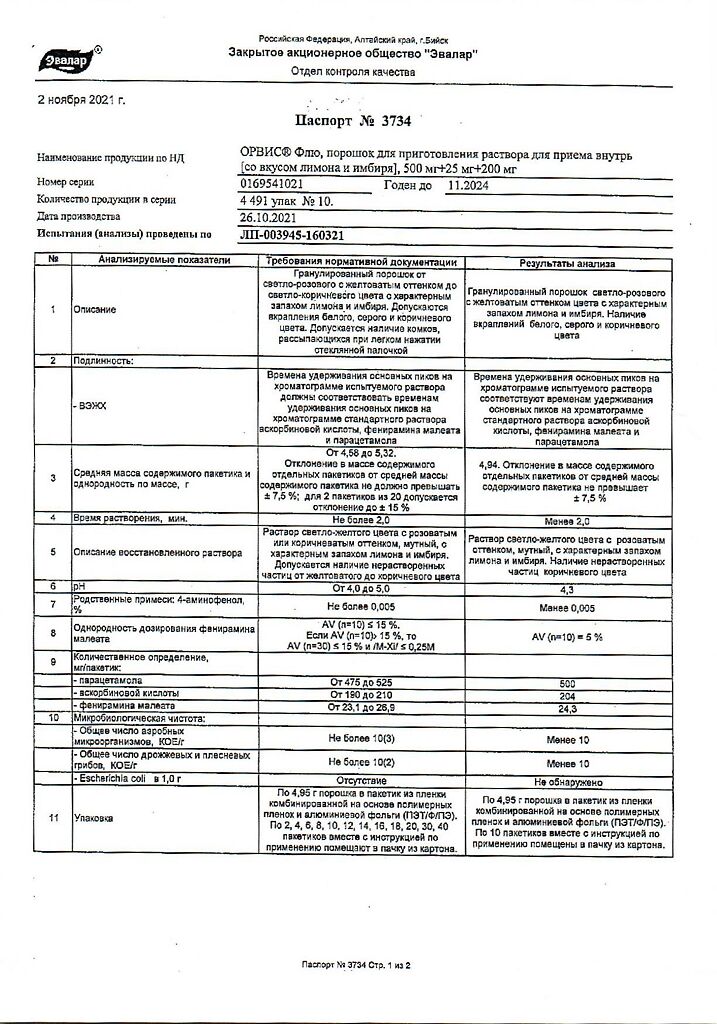
Orvis Flu, 10 pcs.
€8.15 €7.13
Description
Pharmacotherapeutic group:
Pharmacotherapy for symptoms of acute respiratory diseases (ARI) and “colds” (analgesic non-narcotic + H1-histamine receptor blocker + vitamin).
The ATX code: N02BE51
Pharmacological properties
Pharmacodynamics
A combination drug containing paracetamol, pheniramine and ascorbic acid.
Paracetamol is a non-narcotic analgesic, blocks cyclooxygenase, mainly in the central nervous system, affecting the centers of pain and thermoregulation; it has analgesic and antipyretic effects.
Pheniramine is a blocker of H1-histamine receptors; it reduces rhinorrhea and lacrimation, eliminates spastic phenomena, edema and hyperemia of the nasal cavity mucosa, nasopharynx and sinus cavities.
Ascorbic acid is involved in the regulation of redox processes, carbohydrate metabolism, blood coagulation, tissue regeneration, the synthesis of steroid hormones, reduces vascular permeability, reduces the need for vitamins B1, B2, A, E, folic acid, pantothenic acid.
It improves the tolerance of paracetamol and prolongs its effects (associated with prolongation of the half-life (T1/2)).
Pharmacokinetics
Paracetamol
After oral administration is quickly absorbed from the gastrointestinal tract: maximum plasma concentrations of the drug are reached after 10-60 minutes.
The drug is rapidly distributed throughout the body tissues and penetrates the blood-brain barrier.
The binding to plasma proteins is insignificant and has no therapeutic value, but increases with increasing dose.
Metabolism occurs in the liver, 80% of the dose taken enters into conjugation reactions with glucuronic acid and sulfates to form inactive metabolites; 17% undergoes hydroxylation to form 8 active metabolites, which conjugate with glutathione to form inactive metabolites.
One of the hydroxylated metabolic intermediates has hepatotoxic effects.
This metabolite is neutralized by conjugation with glutathione, but it can cumulate and in case of paracetamol overdose (150 mg paracetamol/kg or 10 g of oral paracetamol) cause necrosis of hepatocytes.
Extracted by the kidneys as metabolites, mainly as conjugates. Less than 5% of the dose taken is excreted unchanged. T1/2 is 1 to 3 hours.
Pheniramine
It is almost completely absorbed in the digestive tract. The T1/2 from blood plasma is 1 to 1.5 hours. It is eliminated from the body mainly through the kidneys.
Ascorbic acid
It is absorbed in the small intestine. Bioavailability is approximately 70%. Time of reaching the maximum therapeutic concentration after oral administration – 4 hours. It is metabolized mainly in the liver. It is excreted by the kidneys, through the intestine, with sweat, unchanged and as metabolites.
Indications
Indications
It is used for:
– acute respiratory infections
– acute respiratory viral infections (ARI)
– nasopharyngitis (runny nose)
– Flu to relieve the following symptoms:
– elevated body temperature;
– chills;
– headache;
– stuffy nose;
– rhinorrhea;
– lacrimation;
– sneezing;
– pain in muscles and joints.
Active ingredient
Active ingredient
Paracetamol, Pheniramine, Ascorbic acid
Composition
Composition
1 sachet:
Paracetamol 500 mg
Pheniramine maleate 25 mg
Ascorbic acid 200 mg
Excipients:
Maltodextrin – 3507.25 mg
Aspartame 24.75 mg
Sodium citrate – 247.5 mg
Citric acid anhydrous – 49.5 mg
Lemon powder concentrate (lemon juice, maltodextrin, citric acid) – 247.5 mg
Ginger extract dry (ginger root extract, starch, maltodextrin, colloidal silica) – 49.5 mg
Natural lemon flavoring “Lemon” (aroma composition, aroma component, maltodextrin, humiarabic) – 99 mg.
Interaction
Interaction
Ethanol increases the sedative effect of antihistamines (pheniramine), so it should be avoided during treatment.
In addition, ethanol in concomitant use with pheniramine promotes the development of acute pancreatitis.
Pheniramine increases the effect of sedatives:
Morphine derivatives, barbiturates, benzodiazepine derivatives and other tranquilizers, neuroleptics (meprobamate, phenothiazine derivatives), antidepressants (amitriptyline, mirtazapine, mianserine), hypotensive drugs of central action, sedatives belonging to the H1-histamine blockers, baclofen;
In this case, not only the sedative effect increases, but also the risk of side effects of the drug (urinary retention, dry mouth, constipation).
When used in combination with other drugs with anticholinergic properties (other antihistamines, antidepressants of imipramine group, phenothiazine-type neuroleptics, m-cholinoblocking antiparkinsonics, atropine-like antispasmodics, disopyramide) the central atropine-like effects may be increased.
When using the drug together with inducers of microsomal oxidation: barbiturates, tricyclic antidepressants, anticonvulsants (phenytoin), flumecinol, phenylbutazone, rifampicin and ethanol, the risk of hepatotoxic effects increases significantly (due to the paracetamol contained in it).
Glucocorticosteroids when used concomitantly increase the risk of glaucoma.
Concomitant use with salicylates increases the risk of nephrotoxic effects.
Concomitant use with levomycetin (chloramphenicol) increases the toxicity of the latter.
The paracetamol contained in the drug increases the effect of indirect anticoagulants and reduces the effectiveness of uricosuric drugs.
Directions for use
Directions for use
Orally, 1 sachet 2-3 times a day.
Before use, dissolve the contents of one sachet in a glass (200 ml) of hot water (50-60 ° C).
Add sugar, if necessary.
The drug ORVIS Flux can be taken at any time of the day, but the best effect is achieved by taking the drug at bedtime.
The maximum daily dose of paracetamol is 4 g (8 sachets) if the body weight exceeds 50 kg.
The interval between the doses of the drug must be at least 4 hours.
In patients with impaired renal function (creatinine clearance). Maximum therapy duration is 5 days.
If the symptoms do not relieve within 5 days after the beginning of the drug administration, the body temperature remains high or after the initial decrease it suddenly increases again, it is necessary to consult a physician.
Special Instructions
Special Instructions
The drug does not contain sugar and can be used by patients with diabetes.
The drug should not be used simultaneously with other drugs containing paracetamol.
In order to avoid toxic liver damage, paracetamol should not be combined with alcoholic beverages, and patients prone to alcohol abuse.
The risk of liver damage increases in patients with alcoholic hepatitis.
In case of exceeding the recommended doses and with prolonged use psychic dependence on the drug may occur.
To avoid paracetamol overdose, make sure that the total daily dose of paracetamol contained in all medications taken by the patient does not exceed 4 g.
Contraindications
Contraindications
Hypersensitivity to paracetamol, ascorbic acid, pheniramine or any of the excipients.
Pregnancy and breastfeeding.
Erosive and ulcerative lesions of the gastrointestinal tract (acute phase).
Hepatic insufficiency.
Closed-angle glaucoma.
Urinary retention associated with prostate diseases and urinary disorders.
Portal hypertension.
Alcoholism.
Phenylketonuria.
Deficiency of glucose-6-phosphate dehydrogenase enzyme.
Side effects
Side effects
The drug is well tolerated in the recommended doses.
Possible:
Dryness of the oral mucosa.
Nausea, vomiting, abdominal pain, constipation.
Urinary disorders.
Allergic reactions (erythema, skin rash, pruritus, urticaria, Quincke’s edema, anaphylactic shock).
Bronchospasm.
Drowsiness, impaired accommodation, palpitations, orthostatic hypotension, dizziness, impaired coordination, tremor.
Agitation, nervousness, insomnia, confusion, hallucinations, concentration disorders (more common in elderly patients), mydriasis.
Stevens-Johnson syndrome, toxic epidermal necrolysis (Lyell’s syndrome), acute generalized exanthematous pustulosis.
Hepatotoxic effect, nephrotoxicity.
Anemia, leukopenia, agranulocytosis, thrombocytopenia.
In case of adverse reactions, stop taking the drug and consult a physician.
Overdose
Overdose
Signs of acute paracetamol poisoning are anorexia, nausea, vomiting, pain in the epigastric region, increased sweating, pale skin, drowsiness, metabolic acidosis (including lactoacidosis).
The overdose threshold may be lowered in elderly patients and children, in patients taking certain drugs (e.g., inducers of microsomal liver enzymes), alcohol, or those suffering from exhaustion.
In 1-2 days there are signs of liver dysfunction.
In severe cases liver failure, hepatonecrosis, encephalopathy and coma develop and may be fatal.
Signs of pheniramine poisoning are convulsions, impaired consciousness, coma.
If symptoms of poisoning occur, stop using the drug immediately and seek medical attention.
Gastric lavage, enterosorbents (activated charcoal), prescription of antidote acetylcysteine intravenously or orally (if possible, during the first 10 hours after overdose), symptomatic treatment are recommended.
Pregnancy use
Pregnancy use
Due to the lack of animal studies and clinical trials on the use of the combination of paracetamol, ascorbic acid and pheniramine during pregnancy, administration of the drug in this group of patients is not recommended.
It is unknown whether the active ingredients of the drug penetrate into the breast milk. Administration of the drug ORVIS Flu during breastfeeding is not recommended.
Breast-feeding should be stopped if needed.
Similarities
Similarities
Fervex, Rinzasip for children
Additional information
| Weight | 0.078 kg |
|---|---|
| Shelf life | 3 years |
| Conditions of storage | At a temperature not higher than 25 ° C. Keep out of reach of children. |
| Manufacturer | Evalar, Russia |
| Medication form | Powder for preparation of solution for oral administration |
| Brand | Evalar |
Other forms…
Related products
Buy Orvis Flu, 10 pcs. with delivery to USA, UK, Europe and over 120 other countries.