No products in the cart.
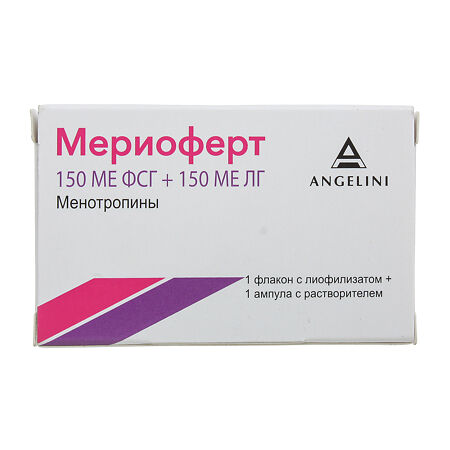
Meriofert, lyophilizate 150 me fsg+150 me lg
€80.55 €67.13
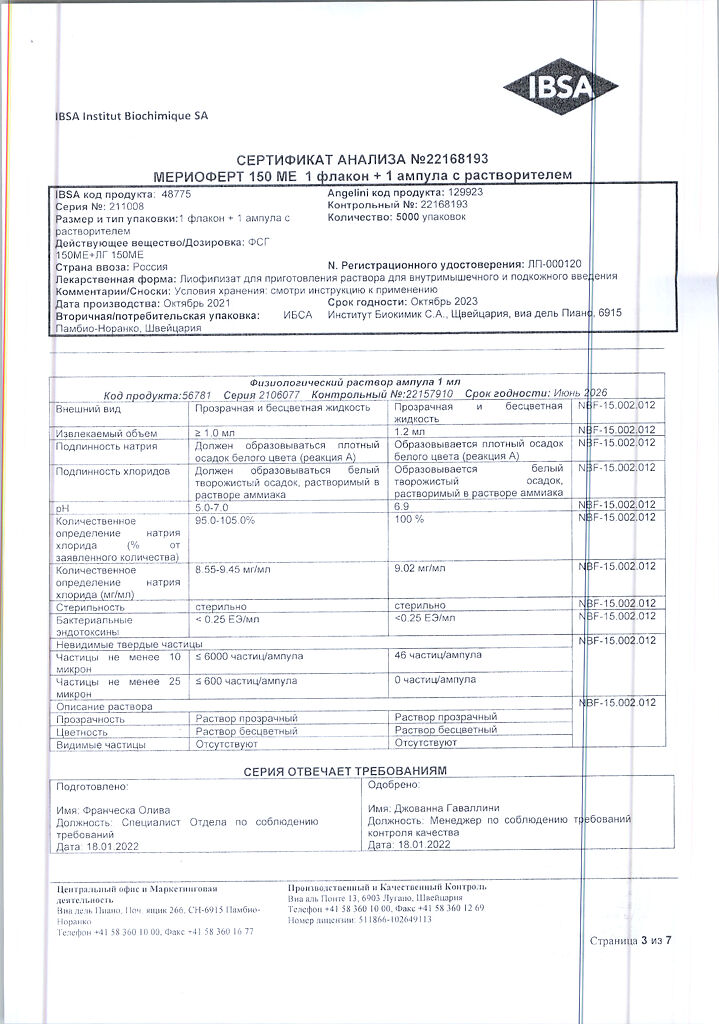
EAN: 7612291483825
SKU: 326218
Categories: Gynecology and Obstetrics, Infertility treatment IVF, Medicine
Description
Meriofert is a highly purified human menopausal gonadotropin (hMG) preparation. It belongs to the group of menotropins. The ratio of the biological activity of follicle stimulating hormone (FSH) and luteinizing hormone (LH) is 1:1. The drug is obtained from the urine of postmenopausal women.
The specific receptors for gonadotropins are present only in the tissues of the genital organs. In the ovaries, LH binds to receptors on the surface of theca cells and the corpus luteum, as well as to granulosa cells of large follicles.
FSH binds to receptors on the surface of granulosa cells of small follicles in the ovaries and Sertoli cells in the testes.
In women, Meriofert stimulates growth and maturation of ovarian follicles, increases the concentration of estrogens, and stimulates endometrial proliferation. In men, it stimulates spermatogenesis in azoospermia and oligoasthenospermia.
Indications
Indications
In women:
– Anovulation (including polycystic ovarian syndrome (PCOS) when clomiphene therapy is ineffective).
– Controlled ovarian hyperstimulation for the induction of multiple follicle growth in assisted reproductive technology (ART).
In men:
Stimulation of spermatogenesis in azoospermia and oligoasthenospermia caused by congenital or acquired hypogonadotropic hypogonadism (in combination with human chorionic gonadotropin (hCG) preparation).
Active ingredient
Active ingredient
Menotropins
Composition
Composition
1 vial of lyophilizate contains:
The active ingredient is highly purified human menopausal gonadotropin hMG (menotropin) 75 ME FSH+75 ME LH, 150 ME FSH+150 ME LH.
Ancillary Component – lactose monohydrate 10.00 mg
1 ampoule with solvent contains:
Sodium chloride (apyrogenic for injection) 9 mg,
water for injection to 1 ml.
Interaction
Interaction
Pharmacodynamic
Meriofert may be administered alone or in combination with gonadotropin-releasing hormone (GnRH) agonists or antagonists
The combined use of Meriofert with other drugs used for ovulation stimulation (e.g. HCG, clomiphene) may increase follicular response. Co-administration with GnRH agonists may require increasing the dose of menotropin.
Pharmaceutical
Meriofert should not be mixed with other medications in the same syringe.
Directions for use
Directions for use
Meriofert is administered intramuscularly or subcutaneously with periodic change of injection site. Subcutaneous method of administration is preferred because it provides the greatest absorption of the drug substance. Therapy with Meriofert should only be carried out under the supervision of a physician with appropriate specialization and experience in infertility treatment.
The solution is prepared immediately before injection using the included solvent. The doses of the drug described below are based on FSH and are the same for both subcutaneous and intramuscular administration.
In women, the dose of the drug is set individually depending on the response of the ovaries. This requires monitoring the response of the ovaries to therapy by ultrasound examination (USG) in conjunction with determination of plasma estradiol concentration.
Anovulation (including PCOS when clomiphene therapy is ineffective).
The drug Meriofert may be administered daily. The drug should be started within the first 7 days of the menstrual cycle. The recommended initial dose is 75-150 IU/day. If the ovaries do not react sufficiently, the dose is gradually increased. The recommended interval for increasing the dose should be at least 7 days. The recommended booster dose is 37.5 ME, but no more than 75 ME. The maximum daily dose usually does not exceed 225 ME. If therapeutic effect is not achieved within 4 weeks of treatment, Meriofert injections are stopped and then a new cycle is started with a higher dose of the drug. The patient is recommended to use barrier methods of contraception or abstain from sexual intercourse until the onset of menstruation.
If an adequate ovarian response is achieved the day after the last injection of Meriofert, 5000-10000 ME hCG is injected once to induce ovulation. The patient is advised to have sexual intercourse on the day of hCG injection and the day after the injection. Intrauterine insemination may be used as an alternative method.
If the ovaries overreact, Meriofert should be stopped and the HCG injection should be discontinued.
Treatment should be resumed in the next cycle at a lower dose than the previous cycle.
Controlled ovarian hyperstimulation for the induction of multiple follicle growth in assisted reproductive technology (ART).
The commonly used protocol for hyperstimulation involves administering 150-225 ME of Meriofert daily starting on day 2 or 3 of the menstrual cycle and continuing until sufficient follicle size is achieved. The daily dose is adjusted according to the patient’s response to therapy. The daily dose of the drug should not exceed 450 ME FSH.
24-48 hours after the last injection of Meriofert, one injection of hCG at a dose of 5000 ME-10000 ME is administered to induce final follicle maturation.
Gonadotropin-releasing hormone (aGnRH) agonists are now widely used to prevent the release of endogenous LH. In this case, the use of the drug
Meriofert should be started approximately two weeks after starting treatment with GnRH agonists. Thereafter, both drugs continue to be used together until an adequate level of follicle development is achieved. The dose of Meriofert is adjusted according to the patient’s ovarian response.
In male hypogonadotropic hypogonadism for stimulation of spermatogenesis, Meriofert is prescribed if the previous therapy with hCG drugs caused only an androgenic response without signs of increased spermatogenesis. In this case, treatment is continued by administering 2,000 ME of hCG 2-3 times a week along with injections of Meriofert (75 ME or 150 ME) 2-3 times a week. Treatment under this regimen should be continued for at least 3 months.
If there is no positive effect during this time, treatment may be continued for up to 18 months.
Special Instructions
Influence on ability to operate vehicles and machinery:
Special Instructions
The treatment should be supervised by a physician experienced in infertility treatment.
Before starting Meriofert, an evaluation for hypothyroidism, adrenal insufficiency, hyperprolactinemia, pituitary or hypothalamic tumors; and appropriate specific treatment is recommended.
SGYA
SGYA is a syndrome distinct from uncomplicated ovarian enlargement, whose manifestations vary in severity. It includes significant ovarian enlargement, high serum estrogen concentrations, and increased vascular permeability, which may lead to fluid accumulation in the abdominal, pleural and, rarely, pericardial cavities (in severe SGF). In moderate CGY, the following symptoms are observed: abdominal pain, abdominal bloating, significant ovarian enlargement, weight gain, shortness of breath, oliguria, and gastrointestinal symptoms, including nausea, vomiting, and diarrhea. Severe SHF develops hypovolemia, hemoconcentration, electrolyte disturbances, ascites, hemoperitoneum, hydrothorax, acute respiratory distress syndrome and thromboembolic complications.
An overreaction of the ovaries to gonadotropin administration rarely results in SHF unless hCG is given to induce ovulation. Therefore, in cases of ovarian hyperstimulation, hCG should not be administered and the patient should be warned to abstain from intercourse or use barrier methods of contraception for at least 4 days. HCG can progress rapidly (within 24 hours to several days), becoming a serious medical complication, so patients should be monitored for at least 2 weeks after HCG injection. Adherence to recommended doses of Meriofert, the administration regimen, and close monitoring of therapy can minimize cases of ovarian hyperstimulation and multiple pregnancies. With ART, aspiration of the contents of all follicles before ovulation can reduce the risk of SGF.
SGF can be more severe and prolonged during pregnancy development. Most commonly, SGY develops after discontinuation of gonadotropin treatment and peaks in severity within 7-10 days of the end of treatment. Typically, SGF passes spontaneously after the onset of menstruation.
With moderate to severe SGF the patient is hospitalized and specific therapy is initiated.
SGF occurs with high frequency in patients with polycystic ovarian syndrome.
Multiple pregnancies.
In multiple pregnancies, there is an increased risk of adverse maternal and perinatal outcomes. Multiple pregnancies are more common with the use of menotropins than with natural conception. In the case of in vitro fertilization (IVF), the likelihood of a multiple pregnancy depends on the number of embryos injected, their quality and the age of the patient. The patient should be warned about the potential risk of multiple pregnancies before starting treatment.
Pregnancy complications.
The incidence of spontaneous abortions in pregnancies after treatment with Meriofert is higher than in healthy women.
Ectopic pregnancy.
Women with a history of fallopian tube disease, whether they conceive naturally or are treated for infertility, have a high risk of ectopic pregnancy. The prevalence of ectopic pregnancy after IVF is 2 to 5% compared with 1 to 1.5% in the general population.
Novoplasms of the reproductive system.
There have been reports of ovarian and other reproductive organ neoplasms, both benign and malignant, in women who have been treated for infertility with multiple ART techniques. It has not yet been determined whether gonadotropin treatment increases the baseline risk of these tumors in women with infertility.
Congenital malformations
The prevalence of congenital fetal malformations with ART is slightly higher than with natural conception. This is thought to be due to the individual characteristics of the parents (age of the mother, characteristics of the sperm) and multiple pregnancies.
Thromboembolic complications
Women with known risk factors for thromboembolic complications, such as individual or familial predisposition, obesity (body mass index > 30 kg/m2) or thrombophilia may have an increased risk of venous or arterial thromboembolic complications during or after gonadotropin treatment. In such cases, the benefit of their use should exceed the risk.
Note that pregnancy itself also increases the risk of thromboembolic complications.
In men with high FSH concentrations in the blood (indicative of primary hypogonadism), Meriofert is usually ineffective.
Meriofert does not affect the ability to operate vehicles and machinery.
Features
Features
The biological efficacy of hMG is mainly due to the follicle-stimulating component. The pharmacokinetic properties of hMG when administered intramuscularly and subcutaneously have high individual variability.
Intestinal absorption
According to studies conducted for Meriofert, after a single subcutaneous and intramuscular administration of the drug at a dose of 300 ME, the time of reaching maximum plasma concentration of the drug (Tmax) is 22 and 19 hours, respectively.
The bioavailability of the drug when administered subcutaneously is higher than when administered intramuscularly.
Elimination
The drug is mainly excreted by the kidneys. The elimination half-life of Meriofert (300 ME FSH) is approximately 45 hours when administered intramuscularly and 40 hours when administered subcutaneously.
Contraindications With caution:
Presence of risk factors for thromboembolic complications, such as individual or familial predisposition, severe obesity (body mass index >30 kg/m2) or thrombophilia, as there is an increased risk of venous or arterial thrombosis and thromboembolism during or after gonadotropin use. In this case, the benefits of gonadotropin treatment should outweigh the risks of gonadotropin use.
Contraindications
– Hypersensitivity to menotropin and other components of the drug.
– Tumors of the pituitary gland or hypothalamus.
– Decompensated thyroid disease, insufficiency of the adrenal cortex, hyperprolactinemia.
– Age less than 18 years.
In women:
Persistent ovarian enlargement, ovarian cysts (not caused by polycystic ovary syndrome).
A genital abnormality incompatible with pregnancy.
The uterine fibroid incompatible with pregnancy.
Vaginal bleeding of unknown etiology.
Estrogen-dependent tumors (ovarian cancer, uterine cancer, or breast cancer).
Primary ovarian insufficiency.
Pregnancy and breastfeeding.
In men:
Prostate cancer, testicular tumor, androgen-dependent tumors.
Primary testicular insufficiency.
Presence of risk factors for thromboembolic complications, such as individual or familial predisposition, severe obesity (body mass index >30 kg/m2) or thrombophilia, as there is an increased risk of venous or arterial thrombosis and thromboembolism during or after gonadotropin use. In this case, the benefits of gonadotropin treatment should outweigh the risks of gonadotropin use.
Side effects
Side effects
The undesirable adverse reactions observed while taking the drug were mostly mild and transient.
The most common adverse reactions were ovarian cyst formation, injection site reactions, and headache (up to 10% frequency). The most serious adverse reactions were SUI and complications associated with this syndrome.
The main adverse reactions are shown in the table below:
Adverse adverse reactions were classified as follows: very frequent (≥1/10); frequent (≥1/100 to ≤1/10); infrequent (≥1/1000 to ≤1/100); rare (≥1/10000 to ≤1/1000); very rare (≤1/10000).
Organs and systems | Frequency . | Adverse reaction | |
Gastrointestinal tract side /p> | Often | Gastrointestinal syndrome, including nausea, vomiting, diarrhea, intestinal colic and bloating, abdominal pain | General disorders and disorders at the site of administration | Very often | Pain, redness, bruising, swelling, and/or irritation at the injection site |
Nervous system side | Very often | Headache < | |
Genital and breast disorders | Very common | Ovarian enlargement and formation of ovarian cysts | |
Often | Ovarian hyperstimulation syndrome, gynecomastia (in men) < | ||
Rarely | Ovarian torsion | /tr> | |
Cardiovascular side | Very rare | Thromboembolism | |
Immune system side | Very rare | Systemic allergic reactions such as skin redness and skin rash, Quincke’s edema | Systemic allergic reactions such as skin redness and skin rash |
Skin and subcutaneous tissue (in men) | Often |
Overdose
Overdose
In case of overdose, development of SHF and thromboembolic complications is possible. Symptoms of SUI are ovarian enlargement, lower abdominal pain, nausea, vomiting, diarrhea, weight gain, oliguria, ascites, hydrothorax, hemoperitoneum, hemoconcentration, shortness of breath (for more information, see section “Special information”). Symptoms of mild to moderate CGY usually do not require additional treatment and disappear on their own within 2-3 weeks. Severe CGY requires hospitalization in the intensive care units of specialized gynecological hospitals for comprehensive treatment.
Additional information
| Weight | 0.017 kg |
|---|---|
| Shelf life | 2 years. |
| Conditions of storage | Store at a temperature not exceeding 25°C in a light-protected place. The reconstituted solution should be used immediately. Store out of the reach of children. |
| Manufacturer | IBSA Institute Biokimik S.A., Switzerland |
| Medication form | lyophilizate |
| Brand | IBSA Institute Biokimik S.A. |
Related products
Gynecology and Obstetrics
Buy Meriofert, lyophilizate 150 me fsg+150 me lg with delivery to USA, UK, Europe and over 120 other countries.