No products in the cart.
Fosamax, tablets 70 mg 4 pcs
€14.51 €12.57
Out of stock
(E-mail when Stock is available)
Description
Bone fragility, Climax, Osteoporosis
- Treatment of osteoporosis in postmenopausal women to prevent fractures, including Fractures of the hip and vertebral compression fractures;
- Preventing osteoporosis at risk in postmenopausal women in order to reduce the likelihood of developing fractures
- Preventing osteoporosis in postmenopausal women
- treatment and prevention of glucocorticoid-induced osteoporosis in men and women
- treatment of Paget’s disease in men and women.
.
Active ingredient
Active ingredient
Alendronic acid
Composition
Composition
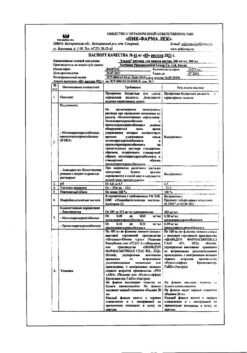
1 tablet contains:
Active substance:
Alendronate sodium 91.37 mg (equivalent to 70 mg of alendronic acid).
Auxiliary substances:
Microcrystalline cellulose 140 mg,
Lactose anhydrous 113.4 mg,
croscarmellose sodium 3.5 mg,
magnesium stearate 1.75 mg.
How to take, the dosage
How to take, the dosage
The recommended dose is one tablet of 70 mg once a week. The optimal duration of bisphosphonate therapy for osteoporosis has not been established. The need for continued bisphosphonate therapy should be evaluated on a regular basis based on the benefit/risk of FOSAMAX® for each patient, especially after 5 or more years of use.
To ensure adequate absorption of alendronate:
FOSAMAX® should be taken at least 30 minutes before the first meal. beverages or daily medication, with plain water only. Other drinks (including mineral water), food and some medicinal products can reduce absorption of alendronate.
To facilitate entry of the tablet into the stomach and reduce the likelihood of local irritation and esophageal irritation/disorders:
- FOSAMAX® should only be taken after rising from bed, with a full glass of water (at least 200 ml);
- Patients should swallow the FOSAMAX® tablet whole. The tablet should not be crumbled, chewed or crumbled in the mouth because of the possibility of mouth and throat ulcers;
- Patients should not lie down before their first meal, which should be at least 30 minutes after taking the tablet;
- Patients should not lie down for at least 30 minutes after taking FOSAMAX®;
- FOSAMAX® should not be taken before bedtime or before getting out of bed.
Patients should take additional calcium and vitamin D supplements if dietary intake is insufficient.
Use in elderly patients: no differences in efficacy or safety profiles of alendronate depending on age have been observed in clinical trials. Therefore, no dose adjustment is required for elderly patients.
Application in renal failure: No dose adjustment is required for patients with glomerular filtration rate (GFR) greater than 35 mL/min.
Alendronate is not recommended for patients with renal insufficiency with a GFR less than 35 mL/min due to insufficient data on its use.
No study of FOSAMAX® 70 mg once-daily in treatment of glucocorticoid-induced osteoporosis was conducted.
Interaction
Interaction
Alendronate absorption may be impaired if the drug is taken simultaneously with beverages, beverages (including mineral water), calcium preparations, antacids and other medicinal products for oral administration. In this regard the interval between taking FOSAMAX® and other oral medicinal products should be at least 30 minutes.
No other clinically relevant drug interactions are expected. In clinical trials, some patients received estrogen (intravaginal, tranedermal, or oral) while taking alendronate. No adverse events associated with their concomitant use have been identified.
Because the use of nonsteroidal anti-inflammatory drugs (NSAIDs) is associated with the development of gastrointestinal erosive ulcers, caution should be exercised when using NSAIDs and alendronate concomitantly.
While no specific interaction studies have been conducted, alendronate has been used concomitantly with a wide range of commonly prescribed medications in clinical studies with no evidence of clinical adverse interactions.
Special Instructions
Special Instructions
The patient should be informed that if symptoms of gastrointestinal damage occur (e.g., pain on swallowing or in the sternum, or if heartburn appears or increases), the drug should be stopped and a physician should be consulted.
The risk of severe adverse esophageal reactions increases in patients who do not take the drug correctly (lying down after taking Fosamax, drinking an incomplete glass of water, continuing to take Fosamax after symptoms of esophageal irritation appear). Therefore, the patient must be clearly informed about the rules of taking the drug.
Patients with exacerbations of upper gastrointestinal disorders (dysphagia, esophageal disorders, gastritis, duodenitis, ulcers) should use Fosamax with caution because of its possible irritating effect on the mucosa and worsening of the underlying disease.
The patient should be informed that if the once-a-week dosage is accidentally missed, 1 tablet should be taken on the morning of the next day. We should not take 2 pills on 1 day, but we should continue to take 1 pill on the day of the week that we have chosen to take it since the start of treatment.
With Fosamax increasing bone mineral content, there may be mild, asymptomatic decreases in serum calcium and phosphate levels (including in patients receiving GCS, who may have decreased calcium absorption).
Patients should take calcium and vitamin D supplements if dietary intake is insufficient.
There were no age differences in the efficacy or safety profile of Fosamax in clinical studies.
In double-blind, multicenter controlled trials, asymptomatic, mild and transient decreases in serum calcium and phosphate levels were observed in 18% and 10% of patients taking Fosamax and 12% and 3% of patients receiving placebo. However, the frequency of decreases in calcium less than 8 mg/dL and phosphate less than 2 mg/dL was similar in both groups.
Contraindications
Contraindications
- Diseases of the esophagus and other factors delaying esophageal emptying, such as strictures or achalasia.
- Inability to sit or stand upright for 30 minutes.
- Hypersensitivity to alendronate or any excipient of the drug.
- Hypocalcemia.
- Hereditary lactase deficiency, glucose-galactose malabsorption.
- Severe mineral metabolism disorders.
- Chronic renal insufficiency (creatinine clearance (CK) Vitamin D deficiency.
- Childhood.
With caution
- Per worsening upper gastrointestinal (GI) conditions such as dysphagia, esophageal disease, gastritis, duodenitis, or peptic ulcer.
- Serious gastrointestinal diseases suffered in the previous 12 months, such as peptic ulcer, gastrointestinal bleeding, or upper GI surgery, except pyloroplasty.
- With a predisposition to hyiocalcemia (hypothyroidism, calcium malabsorption).
Side effects
Side effects
In clinical trials, the following side effects occurred with an incidence of ≥1%:
Digestive system disorders: abdominal pain, dyspepsia, esophageal ulcer, dysphagia, flatulence, constipation, diarrhea, acidic belching, nausea, gastritis, peptic ulcer, including peptic ulcer complicated by bleeding (melena).
Muscular system disorders: myalgia, bone pain, joint pain, muscle cramps.
CNS disorders: headache.
The following side effects have been reported in general clinical practice:
Digestive system side effects: Esophageal erosions or ulcers, nausea, vomiting, gastritis, melena, esophagitis, esophageal stricture, perforation, oropharyngeal ulcer; rarely, gastric and duodenal ulcers (although no association with the drug has been established), local osteonecrosis of the jaw associated primarily with prior tooth extraction and/or local infection (including osteomyelitis), often with slow recovery.
Muscular system disorders: myalgia, bone pain, joint pain (rarely severe), joint swelling, low-energy fractures of the femoral body.
Dermatological reactions: skin rash, erythema, photosensitization, itching, alopecia; rarely – severe skin reactions, including Stevens-Johnson syndrome and toxic epidermal necrolysis.
Allergic reactions: urticaria; rarely – angioedema.
The body in general: transient symptoms of acute phase reactions at the beginning of treatment (myalgia, malaise, asthenia, rarely – fever), hypocalcemia; rarely – peripheral edema.
Senses: rarely – uveitis, scleritis, episcleritis.
CNS disorders: dizziness, systemic dizziness, impaired sense of taste.
Laboratory findings: decrease in serum calcium and phosphate levels (usually mild, asymptomatic and transient) by 18% and 10%, respectively.
Fosamax is generally well tolerated; side effects are usually mild and do not require withdrawal of the drug.
Overdose
Overdose
Symptoms: hypocalcemia, hypophosphatemia, adverse events in the upper gastrointestinal tract, including dipepsia, heartburn, esophagitis, gastritis, gastric and esophageal ulcers.
Treatment: The patient should take milk or antacids to bind alendronate. Vomiting should not be induced to prevent esophageal irritation. Patients should maintain an upright position. There are no data on specific therapy.
.
Pregnancy use
Pregnancy use
Pregnancy use
Alendronate should not be used during pregnancy. There are insufficient data on the use of alendronate in pregnant women.
Animal studies indicate no direct adverse effects during pregnancy, embryonic and fetal development, or postnatal development. Alendronate given to rats during pregnancy caused dystocia due to hypocalcemia.
Application during breastfeeding
There are no data on excretion of alendronate with breast milk. Alendronate should not be administered to women during breastfeeding.
Children
FOSAMAX® should not be used in children less than 18 years of age because of lack of safety and effectiveness data in diseases associated with childhood osteoporosis.
Similarities
Similarities
Foroza, Osterepar, Alendronate
Additional information
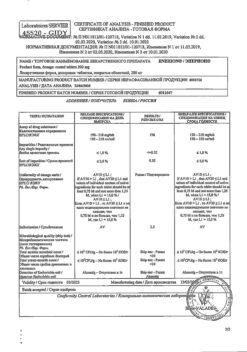
| Weight | 0.040 kg |
|---|---|
| Shelf life | 2 years |
| Conditions of storage | At 15-30 °C |
| Manufacturer | Merck Sharp & Doum B.V., The Netherlands |
| Medication form | pills |
| Brand | Merck Sharp & Doum B.V. |
Related products
Buy Fosamax, tablets 70 mg 4 pcs with delivery to USA, UK, Europe and over 120 other countries.