No products in the cart.
Vancomycin Elfa, 1000 mg powder 20 ml
€6.66 €5.83
Out of stock
(E-mail when Stock is available)
Description Pharmacotherapeutic group: Glycopeptide antibiotic Pharmacodynamics: Pharmacokinetics:
ATC:
J.01.X.A.01 Vancomycin
J.01..X.A Glycopeptide Antibiotics
A tricyclic glycopeptide antibiotic group, isolated from Amycolatopsis orientalis, effective against many gram-positive microorganisms.
The bactericidal effect of vancomycin results from the inhibition of cell wall biosynthesis. In addition, vancomycin can change the permeability of the bacterial cell membrane and RNA synthesis. There is no cross-resistance between vancomycin and antibiotics of other classes.
In vitro vancomycin is active against Gram-positive microorganisms, including Staphylococcus aureus, Staphylococcus epidermidis (including heterogeneous methicillin-resistant strains), Streptococcus pyogenes, Streptococcus pneumoniae (including penicillin-resistant strains).including penicillin-resistant strains), Streptococcus agalactiae, Streptococcus bovis, Streptococcus spp. viridians, Clostridium difficile (including toxigenic strains involved in the development of pseudomembranous colitis) and Corynebacterium spp. Acts bacteriostatic on Enterococcus spp. (including Enterococcus faecalis). Optimum action is at pH 8, the effect decreases sharply when pH is lowered to 6. It is active only against microorganisms that are in the stage of reproduction.
Other microorganisms that are sensitive to vancomycin in vitro include Listeria monocytogenes, Lactobacillus spp, Actinomyces spp, Clostridium spp, Bacillus spp.
In vitro some isolated strains of enterococci and staphylococci show resistance to vancomycin.
The combination of vancomycin and aminoglycosides shows synergism in vitro against many strains of Staphylococcus aureus, Streptococcus spp. (not belonging to enterogroup D), Enterococcus spp., Streptococcus spp. viridians.
Vancomycin is inactive in vitro against Gram-negative microorganisms, mycobacteria, viruses, protozoa and fungi.
Absorption
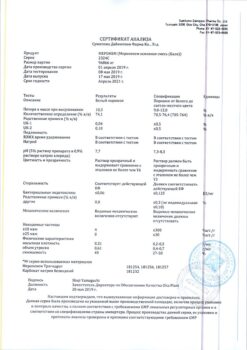
Multiple intravenous injections (IV) of 1 g vancomycin (15 mg/kg; infusion for 60 min) produce mean plasma concentrations of approximately 63 mg/L immediately after completion of infusion. At 2 h after infusion, mean plasma concentrations were about 23 mg/L, and at 11 h, about 8 mg/L.
Multiple infusions of 500 mg (infusion over 30 minutes), produced mean plasma concentrations of about 49 mg/L after completion of the infusions. At 2 h after infusion, mean plasma concentrations were about 19 mg/L and at 6 h, about 10 mg/L. Plasma concentrations of vancomycin in multiple infusions are similar to plasma concentrations in single infusions.
Distribution
The volume of distribution ranges from 0.3 to 0.43 L/kg. As shown by ultrafiltration, at serum vancomycin concentrations of 10 mg/L to 100 mg/L, 55% of vancomycin is detected in a protein-bound state.
After IV administration, vancomycin is detected in pleural, pericardial, ascitic, synovial fluid and atrial auricular tissue, as well as in urine and peritoneal fluid in concentrations that inhibit the growth of microorganisms. In meningitis there is penetration of the drug into the cerebrospinal fluid at therapeutic concentrations. Vancomycin penetrates the placental barrier and is excreted with breast milk.
Metabolism and excretion
Vancomycin is virtually unmetabolized. The average elimination half-life (T1/2) of vancomycin from plasma in patients with normal renal function is 4-6 hours. About 75% of the vancomycin dose is eliminated by the kidneys through glomerular filtration in the first 24 hours. Mean plasma clearance is about 0.058 L/kg/h, and mean renal clearance is about 0.048 L/kg/h. Renal clearance of vancomycin is fairly constant and provides 70-80% excretion.
Pharmacokinetics in special clinical cases
Disordered renal function slows the excretion of vancomycin. In patients with anuria, the mean T1/2 is 7.5 days.
The total systemic and renal clearance of vancomycin may be decreased in elderly patients as a result of natural slowing of glomerular filtration.
.
Indications
Indications
For intravenous infusions
Vancomycin is used for serious or severe infections caused by susceptible organisms, including Staphylococcus spp. (including penicillin-forming and methicillin-resistant strains), Streptococcus spp. (including strains resistant to penicillin), with an allergic reaction to penicillin, with intolerance to other antimicrobial drugs.
Endocarditis
Endocarditis caused by Streptococcus viridans, Streptococcus bovis (monotherapy, combination therapy with aminoglycosides); endocarditis caused by enterococci (including Eterococcus faecalis; as a combination therapy with aminoglycosides for treatment); early endocarditis caused by Staphylococcus epidermidis, Corynebacterium spp. after valve replacement (in combination with rifampicin, aminoglycosides/both antibiotics); prevention of bacterial endocarditis in patients with pathogen resistance to penicillin and heart valve diseases (regardless of their etiology) before surgical interventions in the oral cavity, tonsillectomy, adenoid removal, before catheterization of the bladder, cystoscopy, surgical interventions on the rectum or colon (monotherapy or in combination with aminoglycosides).
– sepsis;
– infections of bones and joints;
– infections of the central nervous system;
– lower respiratory tract infections;
– infections of the skin and soft tissues.
Pharmacological effect
Pharmacological effect
Pharmacotherapeutic group: Antibiotic-glycopeptide
ATX:
J.01.X.A.01 Vancomycin
J.01.X.A Antibiotics of glycopeptide structure
Pharmacodynamics:
An antibiotic of the tricyclic glycopeptide group, isolated from Amycolatopsis orientalis, effective against many gram-positive microorganisms.
The bactericidal effect of vancomycin occurs as a result of inhibition of cell wall biosynthesis. In addition, vancomycin can alter bacterial cell membrane permeability and RNA synthesis. There is no cross-resistance between vancomycin and other classes of antibiotics.
In vitro, vancomycin is active against gram-positive microorganisms, including Staphylococcus aureus, Staphylococcus epidermidis (including heterogeneous methicillin-resistant strains), Streptococcus pyogenes, Streptococcus pneumoniae (including penicillin-resistant strains), Streptococcus agalactiae, Streptococcus bovis, Streptococcus spp. viridians group, Clostridium difficile (including toxigenic strains involved in the development of pseudomembranous colitis) and Corynebacterium spp. Acts bacteriostatically on Enterococcus spp. (including Enterococcus faecalis). The optimum action is at pH 8; when pH decreases to 6, the effect decreases sharply. Actively affects only microorganisms that are in the stage of reproduction.
Other microorganisms that are sensitive to vancomycin in vitro include Listeria monocytogenes, Lactobacillus spp., Actinomyces spp., Clostridium spp., Bacillus spp.
In vitro, some isolated strains of enterococci and staphylococci exhibit resistance to vancomycin.
The combination of vancomycin and aminoglycosides exhibits synergism in vitro against many strains of Staphylococcus aureus, Streptococcus spp. (not belonging to enterogroup D), Enterococcus spp., Streptococcus spp. viridians groups.
Vancomycin is inactive in vitro against gram-negative microorganisms, mycobacteria, viruses, protozoa and fungi.
Pharmacokinetics:
Suction
Repeated intravenous (IV) administration of 1 g of vancomycin (15 mg/kg; infusion over 60 minutes) produces mean plasma concentrations of approximately 63 mg/L immediately after completion of the infusions. At 2 hours after infusion, mean plasma concentrations were about 23 mg/L, and after 11 hours, about 8 mg/L.
Multiple infusions of 500 mg (infusion over 30 minutes) produced mean plasma concentrations of approximately 49 mg/L after completion of the infusions. At 2 hours after infusion, mean plasma concentrations were approximately 19 mg/L, and at 6 hours they were approximately 10 mg/L. Plasma concentrations of vancomycin following multiple doses are similar to plasma concentrations following a single dose.
Distribution
The volume of distribution ranges from 0.3 to 0.43 l/kg. As shown by ultrafiltration, at serum vancomycin concentrations from 10 mg/l to 100 mg/l, 55% of vancomycin is found in a protein-bound state.
After intravenous administration, vancomycin is found in pleural, pericardial, ascitic, synovial fluids and atrial appendage tissue, as well as in urine and peritoneal fluid in concentrations that inhibit the growth of microorganisms. With meningitis, penetration of the drug into the cerebrospinal fluid in therapeutic concentrations is noted. Vancomycin crosses the placental barrier and is excreted in breast milk.
Metabolism and excretion
Vancomycin is practically not metabolized. The average half-life (T1/2) of vancomycin from plasma in patients with normal renal function is 4-6 hours. About 75% of the dose of vancomycin is eliminated by the kidneys due to glomerular filtration in the first 24 hours. The average plasma clearance is about 0.058 L/kg/h, and the average renal clearance is about 0.048 L/kg/h. The renal clearance of vancomycin is fairly constant and ensures its elimination by 70-80%.
Pharmacokinetics in special clinical situations
Impaired renal function slows the elimination of vancomycin. In patients with anuria, the average T1/2 is 7.5 days.
The total systemic and renal clearance of vancomycin may be reduced in elderly patients as a result of a naturally occurring slower glomerular filtration rate.
Special instructions
Special instructions
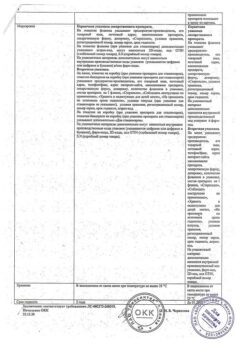
Rapid administration of vancomycin (within minutes) may be accompanied by a significant decrease in blood pressure and, in rare cases, cardiac arrest. Vancomycin should be administered as a diluted solution over at least 60 minutes to avoid adverse reactions associated with rapid infusion.
Patients receiving IV vancomycin should have blood tests and renal function monitored periodically.
When prescribing the drug to newborns (especially premature infants), monitoring the concentration of vancomycin in the blood serum is desirable.
Vancomycin is used for serious or severe infections caused by susceptible organisms, including Staphylococcus spp. (including penicillin-forming and methicillin-resistant strains), Streptococcus spp. (including strains resistant to penicillin) with an allergic reaction to penicillin, intolerance to other antimicrobial drugs.
Vancomycin should be used with caution in patients with renal failure and in patients over 60 years of age (it is advisable to determine vancomycin plasma concentrations), since high, long-term concentrations of the drug in the blood may increase the risk of drug toxicity (maximum vancomycin serum concentrations (Cmax) should not exceed 40 mcg/ml, and minimum concentrations should not exceed 10 mcg/ml; concentrations >80 mcg/ml are considered toxic).
For patients with renal failure, vancomycin dosages should be individualized.
When prescribing the drug, thrombophlebitis may occur; the likelihood of their development can be reduced by slowly administering diluted solutions (2.5-5 g/l) and alternating the sites of drug administration.
There are data on cases of ototoxicity in patients receiving vancomycin. Signs of ototoxicity may be temporary or permanent.
Ototoxicity has been reported to occur most frequently in patients who received high doses of vancomycin; patients who have a history of hearing impairment, or patients who have received concomitant therapy with other ototoxic drugs (eg, aminoglycosides).
Signs of ototoxicity, both temporary and permanent, may occur when using Vancomycin Elfa. Ototoxicity usually occurs in patients receiving high doses of the drug, as well as in patients with hearing loss or concomitant use of other ototoxic drugs.
With concomitant renal failure, the risk of vancomycin ototoxicity increases.
Long-term use of vancomycin can lead to the emergence of resistant strains of bacteria and the development of superinfection. If superinfection develops during therapy, appropriate measures should be taken.
In rare cases, pseudomembranous colitis associated with Clostridium difficile has been reported in patients receiving intravenous vancomycin.
Impact on the ability to drive vehicles. Wed and fur.:
During the period of treatment with the drug, the ability to concentrate may decrease, which should be taken into account when driving vehicles or performing work that requires increased concentration and speed of psychomotor reactions.
Active ingredient
Active ingredient
Vancomycin
Composition
Composition
1 bottle contains:
Active ingredient:
Vancomycin hydrochloride in terms of vancomycin 1000.0 mg.
Pregnancy
Pregnancy
The use of the drug during pregnancy is only for “life-saving” indications, if the expected benefit to the mother outweighs the potential risk to the fetus.
The use of the drug during breastfeeding is contraindicated.
Contraindications
Contraindications
– Breastfeeding period;
– hypersensitivity to vancomycin and other components of the drug;
– neuritis of the auditory nerve.
With caution: Hearing impairment (including a history), renal failure, pregnancy (I, II and III trimester), patients with an allergy to teicoplanin (possibility of cross-allergy).
Side Effects
Side Effects
From the cardiovascular system: cardiac arrest, “flushes”; decreased blood pressure, shock (symptoms are mainly associated with rapid infusion of the drug), vasculitis, thrombophlebitis.
From the digestive system: nausea, pseudomembranous colitis, increased activity of liver transaminases.
From the hematopoietic system: agranulocytosis, eosinophilia, neutropenia, thrombocytopenia, pancytopenia, anemia, leukopenia.
From the urinary system: interstitial nephritis, changes in renal function tests, impaired renal function.
From the senses: ototoxic effects (transient/permanent): tinnitus, dizziness and hearing loss. In most cases, ototoxic effects were observed in patients receiving excess doses of vancomycin, with a history of hearing loss, or in patients receiving concomitant treatment with other drugs with a possible development of ototoxicity, such as aminoglycosides.
Dermatological reactions: exfoliative dermatitis, rash.
Allergic reactions: urticaria, anaphylactoid reactions (associated with rapid infusion of the drug), Stevens-Johnson syndrome, toxic epidermal necrolysis, pruritic dermatosis, benign blistering dermatosis, diffuse exfoliative erythroderma (red man syndrome – redness of the upper body, pain and spasm of the chest and back muscles; after stopping the infusion, reactions are usually disappear within 20 minutes, but sometimes can last up to several hours), a rash accompanied by eosinophilia and systemic manifestations.
Other: drug fever, phlebitis at the injection site, tissue necrosis at the injection site, pain at injection sites, chills.
Interaction
Interaction
With the simultaneous use of vancomycin with local anesthetics, erythema, redness of the skin and anaphylactoid reactions were observed in children, and intracardiac conduction disturbances were observed in adults.
When used simultaneously with general anesthetics and vecuronium bromide, the frequency of side effects increases (risk of decreased blood pressure, development of neuromuscular blockade).
Administration of vancomycin at least 60 minutes before administration of the anesthetic may reduce the likelihood of these reactions.
When simultaneous and/or sequential use of other potentially ototoxic and/or nephrotoxic drugs (aminoglycosides, amphotericin B, acetylsalicylic acid or other salicylates, bacitracin, bumetanide, capreomycin, carmustine, paromomycin, cyclosporine, loop diuretics, polymyxin B, cisplatin, ethacrynic acid) requires carefully monitor the possible development of symptoms of ototoxicity (tinnitus, dizziness and hearing loss) and nephrotoxicity (increased concentrations of creatinine and urea in the blood plasma, hematuria, proteinuria, rash, eosinophilia and eosinophiluria).
Antihistamines, meclozine, phenothiazines, thioxanthenes can mask the symptoms of vancomycin ototoxicity (tinnitus, vertigo).
Vancomycin solution has a low pH, which may cause physical or chemical instability when mixed with other solutions. Mixing with alkaline solutions should be avoided.
Solutions of vancomycin and beta-lactam antibiotics are pharmaceutically incompatible when mixed. The likelihood of precipitation increases with increasing concentrations of vancomycin. The IV system should be thoroughly flushed between use of these antibiotics. In addition, it is recommended to reduce vancomycin concentrations to 5 mg/ml or less.
Overdose
Overdose
Symptoms: increased severity of dose-dependent side effects.
Treatment: symptomatic therapy aimed at maintaining glomerular filtration. Vancomycin is poorly removed by dialysis. There is evidence that hemofiltration and hemoperfusion through a polysulfone ion exchange resin leads to an increase in vancomycin clearance.
Storage conditions
Storage conditions
In a dry place, protected from light, at a temperature of 15 ° C to 25 ° C.
Keep out of the reach of children.
Shelf life
Shelf life
3 years.
Do not use after expiration date.
Manufacturer
Manufacturer
Elfa Laboratories, India
Additional information
| Shelf life | 3 years. Do not use after the expiration date. |
|---|---|
| Conditions of storage | In a dry, light-protected place at a temperature of 15 ° C to 25 ° C. Store out of the reach of children. |
| Manufacturer | Elfa Laboratories, India |
| Medication form | Powder for preparation of solution for infusion |
| Brand | Elfa Laboratories |
Other forms…
Related products
Buy Vancomycin Elfa, 1000 mg powder 20 ml with delivery to USA, UK, Europe and over 120 other countries.