No products in the cart.
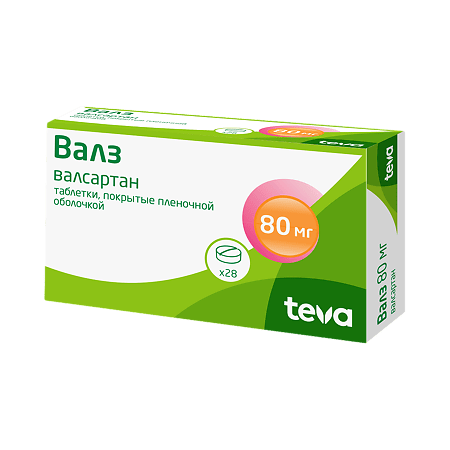
Valz, 80 mg 28 pcs
€10.91 €9.55
Description
Pharmacotherapeutic group: angiotensin II receptor antagonist
ATX code: C09CA03
Pharmacological properties
Pharmacodynamics
p> Valsartan is an active specific angiotensin II receptor antagonist for oral administration. It selectively blocks the AT1 subtype receptors, which are responsible for the effects of angiotensin II. The consequence of blockade of AT1 receptors is an increase in plasma concentration of angiotensin II, which may stimulate unblocked AT2 receptors. Valsartan has no significant agonist activity against AT1 receptors. The affinity of valsartan for AT1 receptors is approximately 20,000 times higher than for AT2 receptors.
Valsartan does not interact with or block other hormone receptors or ion channels that are important in the regulation of cardiovascular function.
The likelihood of coughing with valsartan is very low due to the lack of effect on angiotensin-converting enzyme (ACE), which is responsible for bradykinin degradation.
When comparing valsartan with an ACE inhibitor, the incidence of dry cough was significantly (p < 0.05) lower in patients receiving valsartan than in patients taking an ACE inhibitor (2.6% versus 7.9%, respectively). In the group of patients who had previously developed dry cough when treated with an ACE inhibitor, this adverse event (AE) occurred in 19.5% of cases when treated with valsartan and in 19.0% of cases when treated with a thiazide diuretic, whereas cough occurred in 68.5% of cases when treated with an ACE inhibitor (p < 0.05).
Application in arterial hypertension in patients over 18 years
The treatment of patients with arterial hypertension with valsartan shows a decrease in blood pressure (BP) with no change in heart rate.
After oral administration of a single dose of the drug, the onset of antihypertensive action is seen within 2 hours in most patients, and maximum BP reduction is achieved within 4-6 hours, lasting more than 24 hours. During repeated use of the drug, the maximum BP reduction, regardless of the dose taken, is usually achieved within 2-4 weeks and is maintained at the achieved level during prolonged therapy. In case of concomitant use of the drug with hydrochlorothiazide, a significant additional BP decrease is achieved.
An abrupt discontinuation of valsartan is not accompanied by a significant increase in BP (recoil phenomenon) or other NTs. Patients with arterial hypertension, type 2 diabetes mellitus, and nephropathy taking valsartan at doses of 160-320 mg have a significant reduction in proteinuria (36-44%).
Application after acute myocardial infarction in patients over 18 years of age
. When valsartan is used for 2 years in patients who started taking it between 12 h and 10 days after an acute myocardial infarction (complicated by left ventricular failure and/or left ventricular systolic dysfunction) total mortality, cardiovascular mortality, and time to first hospitalization for exacerbation of chronic heart failure (CHF), recurrent myocardial infarction, sudden cardiac arrest, and stroke (non-fatal) are reduced. The safety profile of valsartan in patients with acute myocardial infarction is similar to that of other conditions.
CHF in patients older than 18 years
. The mechanism of action of valsartan in CHF is based on its ability to eliminate the negative effects of chronic hyperactivation of the renin-angiotensin-aldosterone system (RAAS) and its main effector, angiotensin II, namely, vasoconstriction; fluid retention in the body; cell proliferation, leading to the remodeling of target organs (heart, kidneys, vessels); stimulation of excessive synthesis of hormones that act synergistically with the RAAS (catecholamines, aldosterone, vasopressin, endothelin). Against the background of using valsartan in CHF, preload decreases, pulmonary capillary congestion pressure and diastolic pressure in the pulmonary artery decrease, and cardiac output increases. In addition to hemodynamic effects, valsartan, through indirect blockade of aldosterone synthesis, reduces sodium and water retention in the body.
In general, valsartan leads to fewer hospitalizations for CHF, delays CHF progression, improves NYHA functional class of CHF, increases left ventricular ejection fraction, and decreases signs and symptoms of heart failure and improves quality of life compared with placebo.
Application in patients over 18 years of age with arterial hypertension and impaired glucose tolerance
With valsartan and lifestyle changes, there was a statistically significant reduction in the risk of developing diabetes mellitus in this patient population. Valsartan had no effect on the incidence of fatal cardiovascular events, nonfatal myocardial infarction and ischemic attacks, hospitalizations for heart failure or unstable angina, arterial revascularization, in patients with impaired glucose tolerance and arterial hypertension of different age, gender and race.
Application in children and adolescents 6 to 18 years of age for arterial hypertension
In children and adolescents 6 to 18 years of age, valsartan provides a dose-dependent, smooth reduction in BP. With valsartan, maximum BP reduction, regardless of the dose taken, is usually achieved within 2 weeks, and is maintained during long-term therapy.
Pharmacokinetics
absorption
. After oral administration of valsartan, its maximum plasma concentration (Cmax) is reached within 2-4 hours. The average absolute bioavailability is 23%. When valsartan is taken with food, the area under the concentration-time curve (AUC) is reduced by 48%, although starting about 8 hours after taking the drug, plasma concentrations of valsartan, both when taken on an empty stomach and when taken with food, are the same. The decrease in AUC, however, is not associated with a clinically significant decrease in therapeutic effect, so valsartan can be taken regardless of the time of ingestion.
Distribution
The volume of distribution (Vd) of valsartan at equilibrium after intravenous (IV) administration was approximately 17 liters, indicating that there was no marked distribution of valsartan in tissues. Valsartan is largely bound to serum proteins (94-97%), predominantly to albumin.
Metabolism
Valsartan is not significantly biotransformed (only about 20% of the ingested dose is excreted as metabolites). The hydroxyl metabolite is detected in plasma at low concentrations (less than 10% of the AUC of valsartan). This metabolite is pharmacologically inactive.
Elevation
The pharmacokinetic curve of valsartan has a descending multiexponential character (the elimination half-life of the initial phase (T1/2α) less than 1 hour and the final phase (T1/2β) about 9 hours). Valsartan is excreted mainly unchanged through the intestine (about 83%) and the kidneys (about 13%). After IV administration, plasma clearance of valsartan is about 2 l/h, and its renal clearance is 0.62 l/h (about 30% of total clearance). The half-life (T1/2) of valsartan is 6 hours.
In the range of doses studied, the kinetics of valsartan is linear. No changes in pharmacokinetic parameters were observed with repeated administration of valsartan. When valsartan is administered once daily, there is little cumulation. Plasma concentrations of valsartan in women and men were similar.
Pharmacokinetics in selected patient groups
Patients with CHF
Elderly patients (>65 years)
In some elderly patients, the systemic bioavailability of valsartan is greater than that of younger patients, but this has not been found to have any clinical significance.
Patients with impaired renal function
There has been no correlation between renal function and systemic bioavailability of valsartan. No dose adjustment is required in patients with impaired renal function (creatinine clearance (CK) greater than 10 mL/min). However, valsartan is highly bound to plasma proteins, so its excretion by hemodialysis is unlikely.
Patients with impaired hepatic function
About 70% of the absorbed dose of valsartan is excreted through the intestine (with bile), mostly unchanged. Valsartan is not significantly biotransformed. In patients with mild to moderate hepatic impairment, the bioavailability (AUC) of valsartan is increased by a factor of 2 compared to healthy volunteers. However, there is no correlation between the AUC of valsartan and the degree of hepatic impairment. The use in patients with severe hepatic impairment has not been studied.
Patients 6 to 18 years
The pharmacokinetic properties of valsartan in children and adolescents 6 to 18 years of age do not differ from the pharmacokinetic properties of valsartan in patients older than 18 years.
Indications
Indications
Adults
Arterial hypertension.
Chronic heart failure (II-IV functional class according to the NYHA classification) in patients receiving standard therapy with one or more drugs from the following pharmacotherapeutic groups: diuretics, cardiac glycosides, as well as ACE inhibitors or beta-blockers. The use of each of the listed drugs is not mandatory.
To improve the survival of patients after acute myocardial infarction complicated by left ventricular failure and/or left ventricular systolic dysfunction, in the presence of stable hemodynamic parameters.
Children and teenagers
Arterial hypertension in children and adolescents from 6 to 18 years.
Pharmacological effect
Pharmacological effect
Pharmacotherapeutic group: angiotensin II receptor antagonist
ATX code: C09CA03
Pharmacological properties
Pharmacodynamics
Valsartan is an active specific angiotensin II receptor antagonist intended for oral administration. Selectively blocks receptors of the AT1 subtype, which are responsible for the effects of angiotensin II. The consequence of AT1 receptor blockade is an increase in the plasma concentration of angiotensin II, which can stimulate unblocked AT2 receptors. Valsartan does not have any pronounced agonistic activity against AT1 receptors. The affinity of valsartan for receptors of the AT1 subtype is approximately 20,000 times higher than for receptors of the AT2 subtype.
Valsartan does not interact with or block receptors of other hormones or ion channels, which are of great importance in regulating the functions of the cardiovascular system.
The likelihood of coughing when using valsartan is very low, which is due to the lack of effect on angiotensin-converting enzyme (ACE), which is responsible for the degradation of bradykinin.
When comparing valsartan with an ACE inhibitor, the incidence of dry cough was significantly (p < 0.05) lower in patients receiving valsartan than in patients taking an ACE inhibitor (2.6% versus 7.9%, respectively). In the group of patients who previously developed a dry cough during treatment with an ACE inhibitor, this adverse event (AE) was observed in 19.5% of cases during treatment with valsartan, and in 19.0% of cases during treatment with a thiazide diuretic, while in the group of patients treated with an ACE inhibitor, cough was observed in 68.5% of cases (p < 0.05).
Use for arterial hypertension in patients over 18 years of age
When treating patients with arterial hypertension with valsartan, a decrease in blood pressure (BP) is observed, not accompanied by a change in heart rate.
After oral administration of a single dose of the drug in most patients, the onset of the antihypertensive effect is observed within 2 hours, and the maximum reduction in blood pressure is achieved within 4-6 hours, lasting more than 24 hours. With repeated use of the drug, the maximum reduction in blood pressure, regardless of the dose taken, is usually achieved within 2-4 weeks and is maintained at the achieved level during long-term therapy. In case of simultaneous use of the drug with hydrochlorothiazide, a significant additional reduction in blood pressure is achieved.
Abrupt cessation of valsartan use is not accompanied by a significant increase in blood pressure (rebound phenomenon) or other adverse events. In patients with arterial hypertension, type 2 diabetes mellitus and nephropathy, taking valsartan at a dose of 160-320 mg, there is a significant decrease in proteinuria (36-44%).
Use after acute myocardial infarction in patients over 18 years of age
When using valsartan for 2 years in patients who began taking it in the period from 12 hours to 10 days after acute myocardial infarction (complicated by left ventricular failure and/or left ventricular systolic dysfunction), the rates of overall mortality and cardiovascular mortality are reduced and the time to the first hospitalization for exacerbation of chronic heart failure (CHF) or recurrent infarction increases. myocardium, sudden cardiac arrest and stroke (non-fatal). The safety profile of valsartan in patients with acute myocardial infarction is similar to that in other conditions.
CHF in patients over 18 years of age
The mechanism of action of valsartan in CHF is based on its ability to eliminate the negative consequences of chronic hyperactivation of the renin-angiotensin-aldosterone system (RAAS) and its main effector, angiotensin II, namely vasoconstriction; fluid retention in the body; cell proliferation leading to remodeling of target organs (heart, kidneys, blood vessels); stimulation of excess synthesis of hormones that act synergistically with the RAAS (catecholamines, aldosterone, vasopressin, endothelin). With the use of valsartan for CHF, preload decreases, wedge pressure in the pulmonary capillaries and diastolic pressure in the pulmonary artery decreases, and cardiac output increases. Along with the hemodynamic effects, valsartan, due to indirect blockade of aldosterone synthesis, reduces sodium and water retention in the body.
In general, the use of valsartan leads to a decrease in the number of hospitalizations for CHF, a slowdown in the progression of CHF, an improvement in the functional class of CHF according to the NYHA classification, an increase in left ventricular ejection fraction, as well as a decrease in the severity of signs and symptoms of heart failure and an improvement in quality of life compared to placebo.
Use in patients over 18 years of age with arterial hypertension and impaired glucose tolerance
When using valsartan and changing lifestyle, there was a statistically significant reduction in the risk of developing diabetes mellitus in this category of patients. Valsartan had no effect on the incidence of deaths due to cardiovascular events, myocardial infarction and non-fatal ischemic attacks, hospitalizations due to heart failure or unstable angina, arterial revascularization, in patients with impaired glucose tolerance and arterial hypertension, differing by age, sex and race.
Use in children and adolescents from 6 to 18 years of age with arterial hypertension
In children and adolescents from 6 to 18 years of age, valsartan provides a dose-dependent, smooth reduction in blood pressure. When using valsartan, the maximum reduction in blood pressure, regardless of the dose taken, is usually achieved within 2 weeks, and is maintained at this level during long-term therapy.
Pharmacokinetics
Suction
After taking valsartan orally, its maximum concentration (Cmax) in the blood plasma is achieved within 2-4 hours. The average absolute bioavailability is 23%. When taking valsartan with food, the area under the concentration-time curve (AUC) decreases by 48%, although, starting from approximately the 8th hour after dosing, the concentrations of valsartan in the blood plasma are the same both when taken on an empty stomach and when taken with food. The decrease in AUC, however, is not accompanied by a clinically significant decrease in the therapeutic effect, so valsartan can be taken regardless of meal times.
Distribution
The volume of distribution (Vd) of valsartan at steady state after intravenous (IV) administration was approximately 17 L, indicating a lack of pronounced tissue distribution of valsartan. Valsartan is highly bound to serum proteins (94-97%), mainly to albumin.
Metabolism
Valsartan does not undergo significant biotransformation (only about 20% of the dose taken orally is excreted in the form of metabolites). The hydroxyl metabolite is detected in blood plasma in low concentrations (less than 10% of the AUC of valsartan). This metabolite is pharmacologically inactive.
Removal
The pharmacokinetic curve of valsartan has a descending multi-exponential character (half-life of the initial phase (T1/2α) is less than 1 hour and the final phase (T1/2β) is about 9 hours). Valsartan is excreted mainly unchanged through the intestines (about 83%) and kidneys (about 13%). After intravenous administration, the plasma clearance of valsartan is about 2 l/h, and its renal clearance is 0.62 l/h (about 30% of the total clearance). The half-life (T1/2) of valsartan is 6 hours.
In the range of doses studied, the kinetics of valsartan is linear. With repeated use of valsartan, no changes in pharmacokinetic parameters were observed. When taking valsartan once a day, the accumulation is insignificant. Plasma concentrations of valsartan were similar in women and men.
Pharmacokinetics in selected patient groups
Patients with CHF
In this category of patients, the time to reach Cmax and T1/2 are similar to those in healthy volunteers. The increase in AUC and Cmax is directly proportional to the increase in the dose of the drug (from 40 mg to 160 mg 2 times a day). The cumulation factor averages 1.7. When taken orally, the clearance of valsartan was approximately 4.5 l/h. The age of patients with CHF did not affect the clearance of valsartan.
Elderly patients (over 65 years old)
In some elderly patients, the systemic bioavailability of valsartan is higher than in younger patients, but this has not been shown to have any clinical significance.
Patients with impaired renal function
There was no correlation between renal function and systemic bioavailability of valsartan. In patients with impaired renal function (creatinine clearance (CC) more than 10 ml/min), no dose adjustment is required. However, valsartan has a high degree of binding to plasma proteins, so its elimination during hemodialysis is unlikely.
Patients with liver dysfunction
About 70% of the absorbed dose of valsartan is excreted through the intestines (with bile), mainly unchanged. Valsartan does not undergo significant biotransformation. In patients with mild to moderate liver dysfunction, there is a 2-fold increase in the bioavailability (AUC) of valsartan compared to healthy volunteers. However, there is no correlation between valsartan AUC values and the degree of liver dysfunction. The use of the drug in patients with severe liver dysfunction has not been studied.
Patients from 6 to 18 years old
The pharmacokinetic properties of valsartan in children and adolescents from 6 to 18 years of age do not differ from the pharmacokinetic properties of valsartan in patients over 18 years of age.
Special instructions
Special instructions
Hyperkalemia
When used concomitantly with dietary supplements containing potassium, potassium-sparing diuretics, potassium-containing salt substitutes, or with other drugs that may cause an increase in potassium levels in the blood (for example, heparin), caution should be exercised and regular monitoring of potassium levels in the blood should be carried out.
Renal dysfunction
There is no experience of safe use in patients with creatinine clearance less than 10 ml/min and in patients on hemodialysis, so valsartan should be used with caution in such patients. In patients with CC more than 10 ml/min, no dose adjustment is required.
Liver dysfunction
In patients with mild or moderate hepatic impairment without cholestasis, valsartan should be used with caution.
Sodium deficiency in the body and/or decreased blood volume
In patients with severe sodium deficiency in the body and/or reduced blood volume, for example, those receiving high doses of diuretics, in rare cases, after starting therapy with valsartan, arterial hypotension may develop, accompanied by clinical manifestations. Before starting treatment with Valz, it is necessary to adjust the sodium content in the body and/or replenish the blood volume, including by reducing the dose of the diuretic.
Renal artery stenosis
The use of the drug in a short course in patients with renovascular hypertension, which developed secondary to unilateral stenosis of the artery of a single kidney, does not lead to any significant change in renal hemodynamics, serum creatinine concentration or blood urea nitrogen. However, given that other drugs that affect the RAAS may cause an increase in serum urea and creatinine concentrations in patients with bilateral renal artery stenosis or stenosis of the artery of a solitary kidney, monitoring these indicators is recommended as a precautionary measure.
Kidney transplant
There are no data on the safety of using Valz in patients who have undergone kidney transplantation.
Primary hyperaldosteronism
The drug is not effective for the treatment of arterial hypertension in patients with primary hyperaldosteronism, since activation of the RAAS is not observed in this category of patients.
Aortic and mitral stenosis, obstructive hypertrophic cardiomyopathy
As with other vasodilating agents, caution should be exercised when taking Valz in patients with aortic or mitral stenosis and obstructive hypertrophic cardiomyopathy.
Pregnancy
Taking angiotensin II receptor antagonists is contraindicated during pregnancy. Patients planning a pregnancy should choose treatment with alternative medications that have a proven safety profile when used during pregnancy. If pregnancy is diagnosed during treatment with Valz, it should be discontinued as soon as possible and alternative treatment prescribed (see sections Contraindications and Use during pregnancy and breastfeeding).
CHF/period after myocardial infarction
In patients with CHF or after myocardial infarction who begin treatment with valsartan, a slight decrease in blood pressure is often observed, and therefore it is recommended to monitor blood pressure at the beginning of therapy. If recommendations for changing the dosage regimen are followed, there is usually no need to discontinue the drug due to arterial hypotension. Evaluation of patients with CHF should include assessment of renal function.
Due to inhibition of the RAAS, renal dysfunction may occur in some patients. In patients with CHF functional class II-IV according to the NYHA classification, treatment with ACE inhibitors and angiotensin II receptor antagonists may be accompanied by oliguria and/or an increase in azotemia and, in rare cases, the development of acute renal failure and/or death. Therefore, in these categories of patients, before using the drug Valz, as well as periodically during treatment, it is necessary to evaluate renal function.
Combination therapy for arterial hypertension
For arterial hypertension, the drug Valz can be used in monotherapy, as well as in combination with other antihypertensive drugs, in particular with diuretics.
Combination therapy in the period after myocardial infarction
It is possible to use the drug Valz in combination with other drugs used after myocardial infarction, namely: thrombolytics, acetylsalicylic acid as an antiplatelet agent, beta-blockers, HMG-CoA reductase inhibitors and diuretics. In this category of patients, it is not recommended to use Valz concomitantly with ACE inhibitors, since this combination therapy does not have advantages over valsartan or ACE inhibitor monotherapy in terms of overall mortality from any cause.
Combination therapy for CHF
For CHF, the drug Valz can be used both in monotherapy and simultaneously with other drugs – diuretics, cardiac glycosides, as well as ACE inhibitors or beta-blockers.
In this category of patients, the use of triple combination therapy with an ACE inhibitor, a beta-blocker and Valz is not recommended.
Angioedema (Quincke’s edema)
During treatment with valsartan, there have been reports of the development of angioedema, accompanied by swelling of the larynx and vocal cords, leading to airway obstruction, and/or swelling of the face, lips, pharynx and/or tongue. Some patients in this group had previously experienced angioedema while taking other medications, including ACE inhibitors. If angioedema develops, Valz should be discontinued immediately, after which drugs containing valsartan should not be taken in the future.
Double blockade of the RAAS
When treated with drugs that affect the RAAS, especially when they were combined, a marked decrease in blood pressure, syncope, stroke, hyperkalemia and changes in renal function (including acute renal failure) have been reported in sensitive patients.
Caution is required when combining angiotensin II receptor antagonists, including valsartan, with other drugs that block the RAAS, such as ACE inhibitors or aliskiren.
Concomitant use of angiotensin II receptor antagonists, including valsartan, with drugs containing aliskiren is contraindicated in patients with diabetes mellitus and/or with moderate or severe renal impairment (GFR less than 60 ml/min/1.73 m2 body surface area) and is not recommended in other patients.
Concomitant use of angiotensin II receptor antagonists with ACE inhibitors is contraindicated in patients with diabetic nephropathy and is not recommended in other patients.
Other RAAS stimulation conditions (320 mg dose only)
In patients in whom renal function may be dependent on the activity of the RAAS (for example, patients with severe congenital heart failure), treatment with ACE inhibitors is associated with the occurrence of oliguria and/or progressive azotemia and, in rare cases, acute renal failure and/or death. Since valsartan is an angiotensin II receptor antagonist, it cannot be excluded that its use may be associated with impaired renal function.
Children and teenagers under 18 years of age
Renal dysfunction
The use of the drug has not been studied in patients aged 6 to 18 years with impaired renal function with creatinine clearance <30 ml/min, as well as in patients on hemodialysis, so its use in this group of patients is not recommended. In patients from 6 to 18 years old with CC more than 30 ml/min, no dose adjustment is required. While taking Valz, renal function and serum potassium levels should be carefully monitored. In particular, these precautions must be observed when taking the drug Valz against a background of elevated temperature or decreased blood volume, since in this case the development of renal dysfunction is possible.
Liver dysfunction
As for adult patients, the use of Valz is contraindicated for patients from 6 to 18 years of age with severe liver dysfunction, biliary cirrhosis and cholestasis. Experience with the use of valsartan in patients with mild to moderate liver dysfunction is limited. The dose should not exceed 80 mg in this group of patients.
Impact on the ability to drive vehicles and machinery
Since the development of such adverse events as dizziness or fainting is possible during drug therapy, patients taking the drug Valz should be careful when driving vehicles and engaging in other potentially hazardous activities.
Active ingredient
Active ingredient
Valsartan
Composition
Composition
1 tablet 80 mg contains:
Active ingredient: valsartan 80 mg;
Excipients: lactose monohydrate 42.22 mg, microcrystalline cellulose 36.00 mg, croscarmellose sodium 10.80 mg, povidone K29-32 7.20 mg, talc 1.8 mg, magnesium stearate 1.26 mg, colloidal silicon dioxide 0.72 mg;
Film casing
Opadry II 85G34643 Pink about 7.20 mg (polyvinyl alcohol 3.168 mg, talc 1.440 mg, titanium dioxide 1.373 mg, macrogol – 3350 0.889 mg, iron oxide yellow 0.029 mg, iron oxide red 0.049 mg, lecithin 0.252 mg).
Pregnancy
Pregnancy
Like any other drug that affects the RAAS, Valz should not be used in women planning pregnancy. When prescribing any drug that affects the RAAS, the physician should inform women of childbearing age about the potential dangers of using these drugs during pregnancy.
The use of Valz during pregnancy is contraindicated, since, given the mechanism of action of angiotensin II receptor antagonists, a risk to the fetus cannot be excluded. The effect of ACE inhibitors (drugs that also affect the RAAS) on the fetus, if used in the second and third trimesters of pregnancy, can lead to its damage and death.
According to retrospective data, the use of ACE inhibitors in the first trimester of pregnancy increases the risk of having children with birth defects. There have been reports of spontaneous abortion, oligohydramnios (oligohydramnios) and renal dysfunction in newborns whose mothers unintentionally received valsartan during pregnancy.
If pregnancy is diagnosed during treatment with Valz, it should be discontinued as soon as possible.
It is unknown whether valsartan is excreted into breast milk in humans, therefore the use of Valz is contraindicated during breastfeeding.
Contraindications
Contraindications
Hypersensitivity to any of the components of the drug;
Severe liver dysfunction (more than 9 points on the Child-Pugh scale), biliary cirrhosis and cholestasis;
Pregnancy, breastfeeding period;
Age up to 6 years – according to arterial hypertension, up to 18 years – according to other indications (efficacy and safety of use have not been established);
Concomitant use with aliskiren and drugs containing aliskiren in patients with diabetes mellitus and/or moderate or severe renal impairment (glomerular filtration rate (GFR) less than 60 ml/min/1.73 m2 body surface area);
Concomitant use with ACE inhibitors in patients with diabetic nephropathy;
Lactose intolerance, lactase deficiency, glucose-galactose malabsorption (the drug contains lactose monohydrate).
With caution
Bilateral renal artery stenosis; stenosis of the artery of a single kidney; primary hyperaldosteronism, following a diet with limited salt intake; in conditions accompanied by a decrease in circulating blood volume (CBV) (including diarrhea and vomiting); severe renal failure (creatinine clearance less than 10 ml/min), as there is no clinical data; in patients aged 6 to 18 years and CC less than 30 ml/min, including those on hemodialysis; mild and moderate liver dysfunction of non-biliary origin without cholestasis, CHF functional class II-IV (according to NYHA), mitral or aortic stenosis, hypertrophic obstructive cardiomyopathy, patients after kidney transplantation; simultaneous use of drugs that block the RAAS (ACE inhibitors, aliskiren).
Side Effects
Side Effects
In controlled clinical trials of valsartan in adult patients with hypertension, the incidence of AEs was comparable to placebo.
There are no data on the dependence of the frequency of any of the AEs on the dose or duration of treatment, as well as gender, age or race. The safety profile of Valz in patients with arterial hypertension aged 6 to 18 years does not differ from the safety profile of valsartan in adult patients.
Below are the AEs that were observed during clinical trials, as well as when using the drug in clinical practice.
Frequency of side effects: very common (>10%); often (>1% and 0.1% and 0.01% and <0.1%); very rare (<0.01%), including isolated reports; frequency unknown (the frequency of development cannot be determined from the available data).
Within each group, identified by frequency of occurrence, AEs are distributed in decreasing order of their importance.
Patients with arterial hypertension
From the hematopoietic and lymphatic systems: frequency unknown – decrease in hemoglobin, hematocrit, neutropenia, thrombocytopenia.
From the immune system: frequency unknown – hypersensitivity reactions, including serum sickness.
Metabolism and nutrition: frequency unknown – increased potassium levels in the blood serum, hyponatremia.
From the organ of hearing and labyrinthine disorders: infrequently – vertigo.
Vascular disorders: frequency unknown – vasculitis.
From the respiratory system, chest and mediastinal organs: infrequently – cough.
From the gastrointestinal tract: infrequently – abdominal pain.
From the liver and biliary tract: frequency unknown – impaired liver function, including increased concentration of bilirubin in the blood plasma.
From the skin and subcutaneous tissues: very rarely – angioedema, skin rash, itching; frequency unknown – bullous dermatitis.
Musculoskeletal and connective tissue disorders: frequency unknown – myalgia.
From the kidneys and urinary tract: frequency unknown – impaired renal function, increased concentration of creatinine in the blood serum.
General disorders and disorders at the injection site: uncommon – increased fatigue.
Also, during clinical studies of valsartan in patients with arterial hypertension, the following AEs were observed, the cause-and-effect relationship of which with its use has not been established: arthralgia, asthenia, back pain, diarrhea, dizziness, insomnia, decreased libido, nausea, peripheral edema, pharyngitis, rhinitis, sinusitis, upper respiratory tract infections, viral infections.
Patients receiving valsartan after acute myocardial infarction and/or with CHF
From the hematopoietic and lymphatic systems: frequency unknown – thrombocytopenia.
From the immune system: frequency unknown – hypersensitivity reactions, including serum sickness.
From the side of metabolism and nutrition: infrequently – hyperkalemia; frequency unknown – increased potassium levels in the blood serum, hyponatremia.
From the nervous system: often – dizziness, postural dizziness; infrequently – fainting, headache.
From the organ of hearing and labyrinthine disorders: infrequently – vertigo.
From the heart: infrequently – increased symptoms of CHF.
Vascular disorders: often – marked decrease in blood pressure, orthostatic hypotension; frequency unknown – vasculitis.
From the respiratory system, chest and mediastinal organs: infrequently – cough.
From the gastrointestinal tract: infrequently – nausea, vomiting.
From the liver and biliary tract: frequency unknown – impaired liver function.
From the skin and subcutaneous tissues: infrequently – angioedema; frequency unknown – skin rash, itching, bullous dermatitis.
From the musculoskeletal and connective tissue side: rarely – rhabdomyolysis; frequency unknown – myalgia.
From the kidneys and urinary tract: often – impaired renal function; uncommon – acute renal failure, increased serum creatinine concentration; frequency unknown – increased urea nitrogen content in the blood plasma.
General disorders and disorders at the injection site: infrequently – asthenia, increased fatigue.
Also, during clinical studies of valsartan in patients after acute myocardial infarction and/or with CHF, the following AEs were observed, the cause-and-effect relationship with its use was not established: arthralgia, abdominal pain, back pain, asthenia, insomnia, decreased libido, neutropenia, peripheral edema, pharyngitis, rhinitis, sinusitis, upper respiratory tract infections, viral infections.
Interaction
Interaction
Dual blockade of the RAAS with angiotensin receptor antagonists, ACE inhibitors or aliskiren:
Concomitant use of angiotensin II receptor antagonists with drugs containing aliskiren is contraindicated in patients with diabetes mellitus and/or with moderate or severe renal impairment (GFR less than 60 ml/min/1.73 m2 body surface area) and is not recommended in other patients.
Concomitant use of angiotensin II receptor antagonists with ACE inhibitors is contraindicated in patients with diabetic nephropathy and is not recommended in other patients.
Co-administration is not recommended
Lithium preparations
With the simultaneous use of lithium preparations with ACE inhibitors and angiotensin II receptor antagonists, a reversible increase in the lithium content in the blood serum and, therefore, an increase in its toxic effect are observed. Due to the lack of experience with the use of valsartan and lithium, their simultaneous use is not recommended. If it is necessary to use valsartan and lithium preparations together, it is necessary to ensure control of the lithium content in the blood serum.
Medicines that may increase plasma potassium levels
If simultaneous use with dietary supplements, potassium-containing salt substitutes or other drugs that may cause an increase in potassium levels in the blood is necessary, regular monitoring of potassium levels in the blood plasma should be carried out.
Combinations requiring caution when using
Nonsteroidal anti-inflammatory drugs (NSAIDs)
With simultaneous use of valsartan with NSAIDs (including selective cyclooxygenase-2 inhibitors), its antihypertensive effect may be reduced. When using angiotensin II receptor antagonists simultaneously with NSAIDs, renal function may deteriorate and the potassium level in the blood plasma may increase. If it is necessary to use valsartan and NSAIDs together, before starting treatment, it is necessary to assess renal function and correct disturbances in water and electrolyte balance.
Transport proteins
According to the results of an in vitro study on liver cultures, valsartan is a substrate for the transporter proteins OATP1B1 and MRP2. With simultaneous use of valsartan with inhibitors of the OATP1B1 transport protein (rifampicin, cyclosporine) and with an inhibitor of the MRP2 transport protein (ritonavir), the systemic exposure of valsartan (Cmax and AUC) may increase.
Other groups of drugs
It has been established that with valsartan monotherapy there are no clinically significant interactions with other drugs (cimetidine, warfarin, furosemide, digoxin, atenolol, indomethacin, hydrochlorothiazide, amlodipine, glibenclamide).
Children and teenagers under 18 years of age
In children and adolescents, hypertension is often associated with impaired renal function. This category of patients is recommended to take valsartan with caution concomitantly with other drugs that affect the RAAS, because this may lead to an increase in serum potassium levels. Regular monitoring of renal function and serum potassium levels should be carried out in this group of patients.
Overdose
Overdose
Symptoms: marked decrease in blood pressure, which can lead to depression of consciousness, collapse and/or shock.
Treatment: symptomatic, the nature of which depends on the time elapsed since taking the drug and the severity of the symptoms. In case of accidental overdose, induce vomiting (if the drug was taken recently) or perform gastric lavage. In the event of a pronounced decrease in blood pressure, intravenous administration of a 0.9% sodium chloride solution is necessary as therapy; the patient should be placed with his legs elevated for the period of time required for therapy, taking active measures to maintain the activity of the cardiovascular system, including regular monitoring of the activity of the heart and respiratory system, blood volume and the amount of urine excreted.
Valsartan is not eliminated by hemodialysis.
Storage conditions
Storage conditions
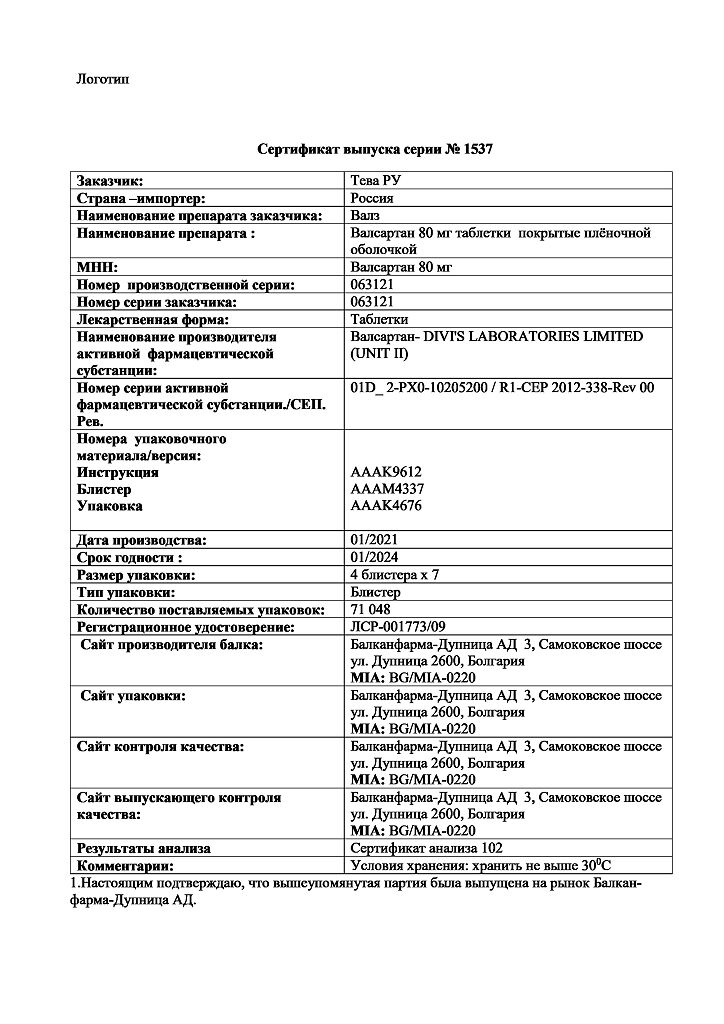
Store at a temperature not exceeding 30 °C.
Keep out of the reach of children!
Shelf life
Shelf life
3 years. Do not use after the expiration date stated on the package.
Manufacturer
Manufacturer
Balkanpharma – Dupnitsa AD, Bulgaria
Additional information
| Shelf life | 3 years. Do not use after the expiration date printed on the package. |
|---|---|
| Conditions of storage | Store at a temperature not exceeding 30 ° C. Keep out of reach of children! |
| Manufacturer | Balkanfarma – Dupnitsa AD, Bulgaria |
| Medication form | pills |
| Brand | Balkanfarma – Dupnitsa AD |
Other forms…
Related products
Buy Valz, 80 mg 28 pcs with delivery to USA, UK, Europe and over 120 other countries.