No products in the cart.
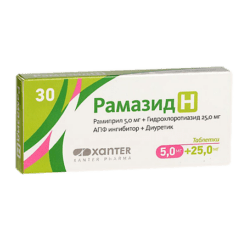
Ramazid N, tablets 5 mg+12, 5 mg 30 pcs
€13.93 €11.61
Description
Hypertension (high blood pressure), OedemaArterial hypertension (patients who are indicated for combination therapy).
Indications
Indications
Arterial hypertension (patients for whom combination therapy is indicated).
Pharmacological effect
Pharmacological effect
Pharmacodynamics
Special instructions
Special instructions
The simultaneous use of Ramazid N (12.5/5 mg) with drugs containing aliskiren or with angiotensin II receptor antagonists, resulting in double blockade of the RAAS, is not recommended due to the risk of an excessive decrease in blood pressure, the development of hyperkalemia and deterioration of renal function. The simultaneous use of Ramazid N (12.5/5 mg) with drugs containing aliskiren in patients with diabetes mellitus and/or renal failure with creatinine clearance <60 ml/min is contraindicated (see section “Contraindications” and “Interaction with other drugs”).
Active ingredient
Active ingredient
Hydrochlorothiazide, Ramipril
Composition
Composition
Active ingredients:
Pregnancy
Pregnancy
Pregnancy
Contraindications
Contraindications
Hypersensitivity to ramipril or other ACE inhibitors, hydrochlorothiazide, other thiazide diuretics, sulfonamide derivatives or to any of the excipients of the drug Ramazid N (12.5/5 mg) (see “composition”).
History of angioedema (hereditary, idiopathic, and also associated with therapy with ACE inhibitors).
Severe renal failure with creatinine clearance less than 30 ml/min per 1.73 m² body surface area.
Hemodialysis or hemofiltration using certain membranes with a negatively charged surface, such as high-strength polyacrylonitrile membranes (risk of developing hypersensitivity reactions, including severe anaphylactoid reactions), and low-density lipoprotein apheresis using dextran sulfate (risk of developing hypersensitivity reactions, including severe anaphylactoid reactions.
Hemodynamically significant bilateral renal artery stenosis, stenosis of the artery of a single kidney.
Clinically significant disturbances in the electrolyte balance of the blood, such as hypokalemia, hypomagnesemia or hypercalcemia (their possibility of aggravation during treatment with Ramazid N (12.5/5 mg)).
Severe liver dysfunction (more than 9 points on the Child-Pugh scale), hepatic encephalopathy (lack of clinical experience with use; it is known that in these conditions, minimal disturbances in water and electrolyte balance can provoke hepatic coma).
Anuria (due to the presence of hydrochlorothiazide in the drug).
Pregnancy.
Breastfeeding period.
Children and adolescents (up to 18 years) (insufficient data on the effectiveness and safety of this drug in children).
Severe arterial hypotension.
Concomitant use with drugs containing aliskiren in patients with diabetes mellitus or with moderate or severe renal failure (GFR < 60 ml/min/1.73 m²).
Concomitant use with angiotensin II receptor antagonists in patients with diabetic nephropathy.
With caution
With simultaneous use of the drug Ramazid N (12.5/5 mg) and drugs containing aliskiren or angiotensin II receptor antagonists (with double blockade of the renin-angiotensin-aldosterone system [RAAS], there is an increased risk of a sharp decrease in blood pressure, the development of hyperkalemia and deterioration of renal function) (see section “Special instructions”).
In conditions accompanied by increased activity of the RAAS, in which, with ACE inhibition, there is a risk of a sharp decrease in blood pressure with deterioration of renal function (see section “Special instructions”):
– severe arterial hypertension, especially malignant arterial hypertension;
– chronic heart failure, especially severe or for which other drugs with antihypertensive effects are being taken (see section “Special Instructions”);
– hemodynamically significant impairment of blood outflow from the left ventricle or blood flow into the left ventricle (hemodynamically significant aortic or mitral valve stenosis or hypertrophic obstructive cardiomyopathy [HOCM]);
– renovascular diseases, including hemodynamically significant unilateral renal artery stenosis (careful monitoring of creatinine concentration in the blood is required, see section “Special instructions”, “Side effects”);
– previous treatment with diuretics;
– disturbances in water and electrolyte balance as a result of insufficient intake of fluid and/or table salt, diarrhea, vomiting, profuse sweating (with inadequate replenishment of fluid and sodium losses).
In conditions in which an excessive decrease in blood pressure becomes especially dangerous (hemodynamically significant stenosis of the coronary or cerebral arteries), regular monitoring of the patient’s condition is required, especially at the beginning of treatment with the drug.
In case of impaired renal function with a creatinine clearance of 60-30 ml/min per 1.73 m² of body surface area due to the risk of developing hyperkalemia and leukopenia (dosage regimen adjustment is required, see section “Dosage and Administration” and regular monitoring of renal function, especially at the beginning of treatment, see section “Special Instructions”).
In the condition after kidney transplantation (regular monitoring of renal function is required, especially at the beginning of treatment).
In case of liver dysfunction (risk of deterioration of liver function, lack of sufficient clinical experience in using the drug, see section “Special instructions”, “Side effects”).
With systemic connective tissue diseases, such as systemic lupus erythematosus or scleroderma (the risk of impaired immune reactions increases, the risk of a decrease in the number of leukocytes in the peripheral blood).
When bone marrow hematopoiesis is suppressed, concomitant therapy with corticosteroids (glucocorticoids and mineralocorticoids), immunomodulators, cytostatics, antimetabolites, allopurinol, procainamide (the risk of a decrease in the number of leukocytes in the peripheral blood increases, see section “Special instructions”, “Side effects”, “Interaction with other drugs”).
In case of diabetes mellitus (the risk of developing hyperkalemia, and in the case of using hypoglycemic agents (insulin preparations and hypoglycemic agents for oral administration (sulfonylurea derivatives)) – the risk of developing hypoglycemic reactions due to the presence of ramipril in the drug; the risk of increased blood glucose concentration due to the presence of hydrochlorothiazide in the drug) (see section “Special instructions”, “Side effects”, “Interaction with others medicines”).
In elderly patients (over 65 years of age) (risk of a more pronounced antihypertensive effect, little experience with the drug, more regular monitoring of renal function is required).
Side Effects
Side Effects
Since the drug Ramazid N (12.5/5 mg) is an antihypertensive drug, many adverse reactions when using it are secondary to its blood pressure-lowering effect, which can cause reflex activation of the sympathetic nervous system or hyperfusion of various organs. Many other undesirable effects, such as effects on fluid and electrolyte balance, some anaphylactoid reactions or inflammatory reactions of the mucous membranes, are a consequence of ACE inhibition or other pharmacological effects of ramipril or hydrochlorothiazide.
According to the World Health Organization (WHO), the frequency of adverse reactions is distributed as follows: very often (>1/10); often (from >1/100 to 1/1000 to 1/10,000 to <1/1000); very rare (<1/10,000); frequency is unknown (it is not possible to determine the frequency of occurrence based on available data).Cardiac disorders
Uncommon: myocardial ischemia, including the development of angina; tachycardia, heart rhythm disturbances, palpitations, peripheral edema.
Frequency unknown: myocardial infarction.
Blood and lymphatic system disorders
Uncommon: decreased number of leukocytes in peripheral blood, decreased number of red blood cells in peripheral blood, decreased hemoglobin, hemolytic anemia, decreased number of platelets in peripheral blood.
Frequency unknown: disorders of bone marrow hematopoiesis, including agranulocytosis (a sharp decrease or disappearance of granulocytes from the peripheral blood), pancytopenia, eosinophilia, hemoconcentration due to a decrease in fluid content in the body and, including in the peripheral blood.
Nervous system disorders
Common: headache, dizziness (feeling of “lightness” in the head).
Uncommon: vertigo, paresthesia, tremor, imbalance, burning sensation of the skin, dysgeusia (impaired sense of taste), ageusia (loss of sense of taste).
Frequency unknown: cerebral ischemia, including ischemic stroke and transient cerebrovascular accident; disturbance of psychomotor reactions, parosmia (impaired sense of smell, including the subjective sensation of any smell in the absence of its objective absence).
Visual disorders
Uncommon: visual disturbances, including blurred vision, conjunctivitis.
Frequency unknown: xanthopsia, decreased tear production (due to the presence of hydrochlorothiazide in the drug).
Hearing and labyrinth disorders
Uncommon: ringing in the ears.
Frequency unknown: hearing loss.
Disorders of the respiratory system, chest and mediastinal organs
Common: non-productive (“dry”) cough, bronchitis.
Uncommon: sinusitis, shortness of breath, nasal congestion.
Frequency unknown: bronchospasm, including increased symptoms of bronchial asthma; allergic alveolitis (pneumonitis); non-cardiogenic pulmonary edema (due to the presence of hydrochlorothiazide in the drug).
Gastrointestinal disorders
Uncommon: inflammatory reactions of the mucous membrane of the gastrointestinal tract, digestive disorders, discomfort in the abdominal area, dyspepsia, gastritis, nausea, constipation; gingivitis (due to the presence of hydrochlorothiazide in the drug).
Very rare: vomiting, aphthous stomatitis, glossitis, diarrhea, epigastric pain, dry oral mucosa.
Frequency unknown: pancreatitis (in exceptional cases, when taking ACE inhibitors, pancreatitis is observed with a fatal outcome); increased activity of “pancreatic” enzymes in the blood: angioedema of the small intestine; sialadenitis (due to the presence of hydrochlorothiazide in the drug).
Renal and urinary tract disorders
Uncommon: renal dysfunction, including acute renal failure; an increase in the amount of urine excreted, an increase in the concentration of urea in the blood, an increase in the concentration of creatinine in the blood (even a slight increase in the concentration of creatinine with unilateral renal artery stenosis may indicate impaired renal function).
Not known: increase in pre-existing proteinuria; interstitial nephritis (due to the presence of hydrochlorothiazide in the drug).
Disorders of the skin and subcutaneous tissues
Uncommon: angioedema: in exceptional cases, airway obstruction due to angioedema can be fatal; psoriasis-like dermatitis; increased sweating; skin rash, in particular maculopapular skin rash; skin itching; baldness.
Frequency unknown: toxic epidermal necrolysis, Stevens-Johnson syndrome, erythema multiforme, pemphigus, worsening of psoriasis, exfoliative dermatitis, photosensitivity reaction, onycholysis, pemphigoid or lichenoid exanthema or enanthema, urticaria; systemic lupus erythematosus (due to the presence of hydrochlorothiazide in the drug).
Musculoskeletal and connective tissue disorders
Uncommon: myalgia.
Frequency unknown: arthralgia, spastic muscle contractions; muscle weakness, muscle rigidity, tetany (due to the presence of hydrochlorothiazide in the drug).
Endocrine system disorders
Not known: syndrome of inappropriate antidiuretic hormone secretion (SIADH).
Metabolic and nutritional disorders
Often: decompensation of diabetes mellitus, decreased glucose tolerance, increased concentrations of glucose in the blood, increased concentrations of uric acid in the blood, increased symptoms of gout, increased concentrations of cholesterol and triglycerides in the blood (due to the presence of hydrochlorothiazide in the drug).
Uncommon: anorexia, decreased appetite; decrease in potassium content in the blood (due to the presence of hydrochlorothiazide in the drug).
Rarely: increased potassium levels in the blood (due to the presence of ramipril in the drug).
Frequency unknown: decreased sodium content in the blood, glycosuria, metabolic alkalosis, hypochloremia, hypomagnesemia, hypercalcemia, dehydration (due to the presence of hydrochlorothiazide in the drug).
Vascular disorders
Uncommon: excessive decrease in blood pressure, orthostatic hypotension (impaired orthostatic regulation of vascular tone), fainting, flushing of blood to the facial skin.
Frequency unknown: thrombosis with severe fluid loss, vascular stenosis, the occurrence or intensification of circulatory disorders against the background of stenotic vascular lesions, Raynaud’s syndrome, vasculitis.
General disorders and disorders at the injection site
Often: increased fatigue, asthenia.
Uncommon: chest pain, increased body temperature.
Immune system disorders
Frequency unknown: anaphylactic or anaphylactoid reactions to ramipril (with ACE inhibition, severe anaphylactic or anaphylactoid reactions to insect venom may be enhanced) or anaphylactic reactions to hydrochlorothiazide; increase in titer of antinuclear antibodies.
Disorders of the liver and biliary tract
Uncommon: cholestatic or cytolytic hepatitis (in exceptional cases with fatal outcome), increased activity of liver enzymes and/or increased concentration of conjugated bilirubin in the blood; calculous cholecystitis (due to the presence of hydrochlorothiazide in the drug).
Frequency unknown: acute liver failure, cholestatic jaundice, hepatocellular lesions.
Disorders of the genital organs and breast
Uncommon: transient erectile dysfunction.
Frequency unknown: decreased libido, gynecomastia.
Mental disorders
Uncommon: depressed mood, apathy, anxiety, nervousness, sleep disturbances (including drowsiness).
Frequency unknown: confusion, restlessness, attention disturbances (decreased concentration).
Interaction
Interaction
Contraindicated combinations
• Extracorporeal treatments that expose blood to negatively charged surfaces, such as hemodialysis or hemofiltration with certain high-strength membranes (polyacrylonitrile membranes) and low-density lipoprotein apheresis with dextrin sulfate.
Risk of developing severe anaphylactoid reactions (see section “Contraindications”, “Special instructions”).
• Simultaneous use of the drug Ramazid N (12.5/5 mg) and drugs containing aliskiren
The simultaneous use of Ramazid N (12.5/5 mg) and drugs containing aliskiren in patients with diabetes mellitus or moderate to severe renal failure and creatinine clearance less than 60 ml/min is contraindicated and is not recommended in other patients (see section “Contraindications”, “With caution”, “Special instructions”).
• Simultaneous use of the drug Ramazid N (12.5/5 mg) and angiotensin II receptor antagonists
The simultaneous use of Ramazid N (12.5/5 mg) and angiotensin II receptor antagonists is contraindicated in patients with diabetic nephropathy and is not recommended in other patients (see section “Contraindications”, “With caution”, “Special instructions”).
Not recommended combinations
• With Katya salts, potassium-sparing diuretics (for example, spironolactone), epleron [spironolactone derivative], amiloride, triamterene), other drugs that can increase the content of potassium in the blood serum (including angiotensin II receptor antagonists, tacrolimus, cyclosporine, trimethoprim, sulfamethoxazole, included in co-trimoxazole [a combination antibacterial agent containing trimethoprim and sulfamethoxazole]).
An increase in the potassium content in the blood serum is possible, sometimes significantly (with simultaneous use, careful monitoring of the potassium content in the blood serum is required).
Combinations to use with caution
• With antihypertensive drugs and other drugs with antihypertensive effects (nitrites, tricyclic antidepressants)
Potentiation of the antihypertensive effect is possible.
• With general anesthesia, barbiturates, ethanol
Orthostatic hypotension may develop. Ramipril may potentiate the vasodilatory effect of ethanol.
• With diuretics
An excessive decrease in blood pressure is possible at the beginning of treatment (for simultaneous use with diuretics, see the section “Contraindications”, “With caution”, “Special instructions”).
• With vasopressor sympathomimetics (epineurine (adrenaline), isoproterenol, dobutamine, dopamine)
Reducing the antihypertensive effect of the drug Ramazid N (12.5/5 mg). It is recommended to carefully monitor blood pressure. In addition, the pressor effect of sympathomimetics may be reduced by hydrochlorothiazide.
• With allopurinol, immunosuppressive drugs, corticosteroids (glucocorticoids and mineralcorticoids), procainamide, cytostatics and other drugs that can change the peripheral blood picture
The likelihood of blood disorders increases (see section “Side effects”, “Special instructions”).
• With lithium salts
There may be a decrease in lithium excretion, leading to increased serum lithium concentrations and increased toxicity. Therefore, it is necessary to regularly monitor serum lithium concentrations.
• With hypoglycemic agents (for example, insulins, oral hypoglycemic agents (sulfonylurea derivatives))
ACE inhibitors may reduce insulin resistance. In some cases, in patients receiving hypoglycemic agents, such a decrease in insulin resistance can lead to the development of hypoglycemia. This effect may develop after several days or months of treatment. Hydrochlorothiazide may weaken the effect of hypoglycemic agents. Therefore, at the initial stage of simultaneous use of hypoglycemic agents and the drug Ramazid N (12.5/5 mg), particularly careful monitoring of blood glucose concentrations is required.
• With vildagliptin, other gliptins and estramustine
Increased incidence of angioedema.
• With mTOR inhibitors (mammalian Target of Rapamycin – target of rapamycin in mammalian cells), for example, temsirolimus
Combinations to consider
• With non-steroidal anti-inflammatory drugs (indomethacin, acetylsalicylic acid (more than 3 g/day))
The effect of the drug Ramazid N (12.5/5 mg) may be weakened, the risk of renal dysfunction and an increase in the content of potassium ions in the blood serum may increase.
Strict monitoring of serum creatinine concentrations and serum potassium levels is recommended.
• With heparin
Possible increase in serum potassium levels.
• With corticosteroids (glucocorticoids and mineralcorticoids), carbenoxolone, drugs containing licorice root, laxatives (with long-term use) and other kaliuretic drugs
The risk of developing hypokalemia increases.
• With cardiac glycosides, drugs that can prolong the QT interval, antiarrhythmics
The potential for the development of hypokalemia or hypomagnesemia (due to the content of hydrochlorothiazide in the drug), which can lead to a potentiation of the proarrhythmic effect of these drugs or a decrease in the antiarrhythmic effect of antiarrhythmics.
• With methyldopa
Possible hemolysis
• With calcium salts and drugs that increase calcium levels in blood plasma
When used simultaneously with hydrochlorothiazide, an increase in calcium levels in the blood serum is possible.
• With vitamin D
When used simultaneously with hydrochlorothiazide, an increase in calcium levels in the blood serum is possible (due to a slowdown in the excretion of calcium by the kidneys); careful monitoring of calcium levels in the blood serum is required.
• With carbamazepine
Risk of developing hyponatremia due to the potentiating effect of hydrochlorothiazide.
• With iodinated contrast agents
If dehydration occurs due to diuretics, including hydrochlorothiazide, there is an increased risk of acute renal impairment, especially when high doses of contrast agent are administered.
• With penicillin
Hydrochlorothiazide is excreted by the distal renal tubules and therefore reduces the excretion of penicillin.
• With quinidine
Hydrochlorothiazide reduces the excretion of quinidine.
• With orally administered ion exchange resins such as colestipol and colestyrami
The absorption of hydrochlorothiazide is reduced.
• With non-depolarizing muscle relaxants
Possible enhancement and prolongation of the muscle relaxant effect.
• With table salt
With a large amount of table salt coming from food, the antihypertensive effect of the drug Ramazid N (12.5/5 mg) may be weakened.
• With desensitizing therapy
The likelihood and severity of anaphylactic reactions to insect venom increases with ACE inhibition. It is assumed that similar reactions are possible to other allergens.
• With warfarin, acenocoumarol
When used concomitantly with ramipril, no effect on the anticoagulant effect of these drugs was observed.
Impact on laboratory results
• Assessment of parathyroid function
Hydrochlorothiazide stimulates renal calcium reabsorption and may cause hypercalcemia. This must be taken into account when assessing the function of the parathyroid glands (see section “Special instructions”).
Overdose
Overdose
Symptoms
In case of overdose, it is possible to develop a persistent increase in the amount of urine excreted, excessive peripheral vasodilation (with a pronounced decrease in blood pressure, the development of shock), bradycardia, water and electrolyte balance disorders, renal failure, heart rhythm disturbances, depression of consciousness, up to the development of coma; cerebral spasms, paresis and paralytic ileus.
In patients with impaired urine outflow (for example, with prostatic hyperplasia), excessive diuresis can provoke acute urinary retention with bladder overdistension.
Treatment
If possible, during the first 30 minutes you should perform gastric lavage and give adsorbents and sodium sulfate. In case of development of a persistent decrease in blood pressure, in addition to therapy aimed at replenishing the volume of circulating blood and electrolytes, administration of alpha1-adrenergic receptor agonists (norepinephrine, dopamine) is indicated. In case of bradycardia refractory to drug treatment, installation of a temporary artificial pacemaker may be required. In case of overdose, it is necessary to monitor serum creatinine concentrations and the content of electrolytes in the blood serum.
There is no experience regarding the effectiveness of forced diuresis, changes in urine pH, hemofiltration or hemodialysis to accelerate the elimination of ramipril and ramiprilat. Hydrochlorothiazide can be eliminated by hemodialysis. If you still intend to perform hemodialysis or hemofiltration, you should take into account the risk of developing anaphylactoid reactions when using high-flow membranes and do not use them (see section “Contraindications”, “Special instructions”, “Interaction with other drugs”).
Storage conditions
Storage conditions
At a temperature not exceeding 25 °C.
Shelf life
Shelf life
2 years.
Manufacturer
Manufacturer
Actavis Ltd, Malta
Additional information
| Shelf life | 2 years. |
|---|---|
| Conditions of storage | At a temperature not exceeding 25 ° C. |
| Manufacturer | Actavis Ltd, Malta |
| Medication form | pills |
| Brand | Actavis Ltd |
Other forms…
Related products
Buy Ramazid N, tablets 5 mg+12, 5 mg 30 pcs with delivery to USA, UK, Europe and over 120 other countries.