No products in the cart.
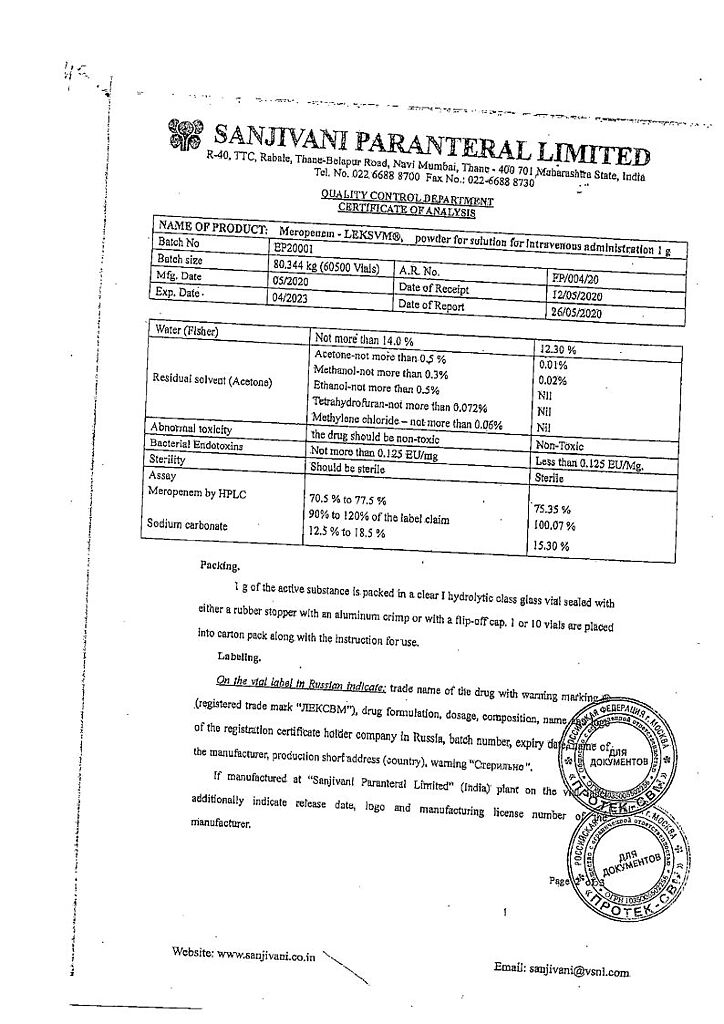
Meropenem-LEXVM, 1 g
€1.00
Out of stock
(E-mail when Stock is available)
Description
Meropenem-LEXVM is an antibiotic for parenteral use from the group of carabapenems, it has a bactericidal effect (inhibits the synthesis of the bacterial cell wall), easily penetrates through the cell wall of bacteria, resistant to the action of most beta-lactamases.
In contrast to imipenem it is practically not degraded in renal tubules by dehydropeptidase-1 (it does not need to be combined with cilastatin – specific inhibitor of dehydropeptidase-1) and, correspondingly, nephrotoxic degradation products are not formed, it has high affinity to proteins binding penicillin. Bactericidal and bacteriostatic concentrations practically do not differ.
It interacts with receptors – specific penicillin-binding proteins on the surface of cytoplasmic membrane, inhibits synthesis of pentidoglycan layer of cell wall, inhibits transpeptidase, promotes release of autolytic enzymes of cell wall which eventually causes its damage and death of bacteria.
The spectrum of antibacterial activity of meropenem includes most clinically relevant Gram-positive and Gram-negative aerobic and anaerobic bacterial strains:
- Gram-positive aerobes: Enterococcus faecalis (including vancomycin-resistant strains), Staphylococcus aureus(penicillin-unproducing and penicillin-producing [methylline-sensitive]); Streptococcus agalactiae, Streptococcus pneumoniae (penicillin-sensitive only); Streptococcus pyogenes, Streptococcus spp. groups viridans.
- Generative aerobes: Escherichia coli, Haemophilus influenzae (penicillin-producing and penicillin-producing), Klebsiella pneumoniae, Neisseria meningitidis, Pseudomonas aeruginosa, Proteus mirabilis.
- Anaerobic bacteria: Bacteroides fragilis, Bacteroides thetaiotaomicron, Peptostreptococcus spp.
Meropenem is effective in vitro against the following microorganisms, but clinically its effectiveness against diseases caused by these pathogens has not been proven:
- Gram-positive aerobes: Staphylococcus epidermidis (penicillinase-producing and penicillinase-producing [methylline-sensitive]).
- Gram-positive aerobes: Acinetobacter spp, Aeromonas hydrophila, Campylobacter jejuni, Citrobacter diversus, Citrobacter freundii, Enterobacter cloacae, Haemophilus influenzae (ampicillin-resistant, penicillin-zoon-producing strains), Hafnia alvei, Klebsiella oxytoca, Moraxella catarrhalis (penicillinase-producing and penicillinase-producing strains), Morganella morganii, Pasteurella multocida, Proteus vulgaris, Salmonella spp., Serratia marcesccns, Shigella spp, Yersinia enterocolitica.
- Anaerobic bacteria: Bacteroides distasonis, Bacteroides ovatus, Bacteroides uniformis, Bacteroides ureolyticus, Bacteroides vulgatus, Clostridium difficile, Clostridium peifringens, Eubacterium lentum, Fusobacterium spp, Prevotella bivia, Prevotella intermedia, Prevotella melaninogenica, Porpliyroiiionas asaccharolylica, Propionibacterium acnes.
Pharmacokinetics:
At an intravenous injection of 250 mg within 30 minutes, the Cmax of the active substance in plasma reaches 11 µg/mL, for a dose of 500 mg, 23 µg/mL, and 1 g, 49 µg/mL (absolute pharmacokinnetic proportional relationship to the dose administered for Cmax and AUC. When the dose is increased from 0.25 to 2 g, clearance decreases from 287 to 205 mL/min. When administered by IV bolus for 5 min, 500 mg Cmax is 52 mcg/ml, 1 g is 112 mcg/ml. The binding to plasma proteins is 2%.
It penetrates well into most tissues and body fluids, including cerebrospinal fluid (CSF) of patients with bacterial meningitis, reaching concentrations higher than required for suppression of most bacteria (bactericidal concentrations are formed 0.5-1.5 hours after the beginning of infusion). It penetrates into breast milk in insignificant amounts.
It is subject to minor metabolism in the liver with the formation of a single inactive metabolite. T1/2 – 1 hour, in children under 2 years old – 1.5-2.3 hours. There is a linear dependence of pharmacokinetic parameters in the dose range of 10-40 mg/kg in adults and children. It does not cumulate.
It is excreted by the kidneys – 70% unchanged within 12 hours. Urinary concentration of meropenem exceeding 10 µg/ml is maintained for 5 h after administration of 500 mg. In patients with renal insufficiency, clearance correlates with creatinine clearance. In elderly patients, decreased clearance of meropenem correlates with decreased creatinine clearance associated with age. T1/2 is 1.5 h. It is excreted by hemodialysis.
Indications
Indications
Infectious and inflammatory diseases caused by microorganisms sensitive to meropenem, including polymicrobial infections (as monotherapy or combination with other antibacterial, antiviral and antifungal drugs):
– lower respiratory tract infections (including pneumonia, including hospital pneumonia);
– urinary tract infections (including pyelonephritis, pyelitis);
— infections of the skin and soft tissues (including erysipelas, impetigo, secondary infected dermatoses);
– intra-abdominal infections (complicated appendicitis, peritonitis, pelvioperitonitis);
– septicemia;
— infections of the pelvic organs (including endometritis);
– bacterial meningitis;
– suspected bacterial infection in adults with febrile neutropenia (empirical treatment as monotherapy or in combination with antiviral or antifungal agents).
Pharmacological effect
Pharmacological effect
Meropenem-LEKSVM is an antibiotic for parenteral use from the carabapenem group, has a bactericidal effect (inhibits the synthesis of the bacterial cell wall), easily penetrates the bacterial cell wall, and is resistant to the action of most beta-lactamases.
Unlike imipenem, it is practically not destroyed in the renal tubules by dehydropeptidase-1 (does not need to be combined with cilastatin, a specific inhibitor of dehydropeptidase-1) and, accordingly, no nephrotoxic breakdown products are formed, and has a high affinity for penicillin-binding proteins. Bactericidal and bacteriostatic concentrations are practically the same.
Interacts with receptors – specific penicillin-binding proteins on the surface of the cytoplasmic membrane, inhibits the synthesis of the pentidoglycan layer of the cell wall, inhibits transpeptidase, promotes the release of autolytic enzymes of the cell wall, which ultimately causes its damage and death of bacteria.
The spectrum of antibacterial activity of meropenem includes the majority of clinically significant gram-positive and gram-negative aerobic and anaerobic strains of bacteria:
Gram-positive aerobes: Enterococcus faecalis (including vancomycin-resistant strains), Staphylococcus aureus (penicillinase-non-producing and penicillinase-producing [methylllin-sensitive]); Streptococcus agalactiae, Streptococcus pneumoniae (penicillin-sensitive only); Streptococcus pyogenes, Streptococcus spp. viridans group.
Gram-negative aerobes: Escherichia coli, Haemophilus influenzae (penicillinase-non-producing and penicillinase-producing), Klebsiella pneumoniae, Neisseria meningitidis, Pseudomonas aeruginosa, Proteus mirabilis.
Anaerobic bacteria: Bacteroides fragilis, Bacteroides thetaiotaomicron, Peptostreptococcus spp.
Meropenem is effective in vitro against the following microorganisms, but its clinical effectiveness against diseases caused by these pathogens has not been proven:
Gram-positive aerobes: Staphylococcus epidermidis (penicillinase-non-producing and penicillinase-producing [methylllin-sensitive]).
Gram-negative aerobes: Acinetobacter spp., Aeromonas hydrophila, Campylobacter jejuni, Citrobacter diversus, Citrobacter freundii, Enterobacter cloacae, Haemophilus influenzae (ampicillin-resistant, penicillinzone-non-producing strains), Hafnia alvei, Klebsiella oxytoca, Moraxella catarrhalis (penicillinase-non-producing and penicillinase-producing), Morganella morganii, Pasteurella multocida, Proteus vulgaris, Salmonella spp., Serratia marcesccns, Shigella spp., Yersinia enterocolitica.
Anaerobic bacteria: Bacteroides distasonis, Bacteroides ovatus, Bacteroides uniformis, Bacteroides ureolyticus, Bacteroides vulgatus, Clostridium difficile, Clostridium peifringens, Eubacterium lentum, Fusobacterium spp., Prevotella bivia, Prevotella intermedia, Prevotella melaninogenica, Porpliyroiiionas asaccharolylica, Propionibacterium acnes.
Pharmacokinetics:
With intravenous administration of 250 mg over 30 minutes, the Cmax of the active substance in the blood plasma reaches 11 mcg/ml, for a dose of 500 mg – 23 mcg/ml, 1 g – 49 mcg/ml (absolute pharmacokinetic proportional dependence on the administered dose for Cmax and AUC. When the dose is increased from 0.25 to 2 g, clearance decreases from 287 to 205 ml/min. When administered intravenously over 5 minutes, 500 mg Cmax is 52 mcg/ml, 1 g is 112 mcg/ml. Communication with plasma proteins is 2%.
Penetrates well into most tissues and body fluids, incl. into the cerebrospinal fluid (CSF) of patients with bacterial meningitis, reaching concentrations exceeding those required to suppress most bacteria (bactericidal concentrations are created 0.5-1.5 hours after the start of infusion). Passes into breast milk in small quantities.
Subjects to minor metabolism in the liver with the formation of a single inactive metabolite. T1/2 – 1 hour, in children under 2 years – 1.5-2.3 hours. In the dose range of 10-40 mg/kg in adults and children, a linear dependence of the pharmacokinetic parameters is observed. Does not cumulate.
Excreted by the kidneys – 70% unchanged within 12 hours. The concentration of meropenem in the urine exceeding 10 mcg/ml is maintained for 5 hours after administration of 500 mg. In patients with renal failure, clearance correlates with creatinine clearance. In elderly patients, the decrease in meropenem clearance correlates with the age-related decrease in creatinine clearance. T1/2 – 1.5 hours. Excreted during hemodialysis.
Special instructions
Special instructions
Patients with a history of hypersensitivity to carbapenems, penicillins, or other beta-lactam antibiotics may exhibit hypersensitivity to meropenem.
Treatment of patients with liver diseases should be carried out under the control of the activity of “liver” transaminases and the concentration of bilirubin.
During treatment, pathogen resistance may develop, and therefore long-term treatment is carried out under constant monitoring of the spread of resistant strains. In persons with diseases of the gastrointestinal tract (GIT), especially colitis, it is necessary to consider the possibility of developing pseudomembranous colitis (the toxin produced by Clostridium difficile is one of the main causes of colitis associated with antibiotics), the first symptom of which may be the development of diarrhea during treatment.
When monotherapy for established or suspected severe lower respiratory tract infection caused by Pseudomonas aeruginosa, regular testing of the sensitivity of the pathogen is recommended. There is no experience with the use of meropenem in children with neutropenia or primary or secondary immunodeficiency.
During the treatment period, care must be taken when driving vehicles and engaging in potentially hazardous activities that require increased concentration and speed of psychomotor reactions.
Active ingredient
Active ingredient
Meropenem
Composition
Composition
Meropenem-LEKSVM powder for the preparation of a solution for intravenous administration
1 fl.:
meropenem 1 g.
Contraindications
Contraindications
Hypersensitivity to any of the components of the drug. Children up to 3 months of age (no data on effectiveness and tolerability).
With caution. Simultaneous administration with nephrotoxic drugs; patients with colitis.
Use for liver dysfunction
Treatment of patients with liver diseases should be carried out under the control of the activity of “liver” transaminases and the concentration of bilirubin.
Use for renal impairment
If renal function is impaired, the dose is adjusted depending on creatinine clearance.
Use in children
Contraindicated in children under 3 months (no data on efficacy and tolerability). There is no experience of use in children with impaired renal function.
Side Effects
Side Effects
From the digestive system: pain in the epigastric region, nausea, vomiting, diarrhea, constipation, anorexia, jaundice; candidiasis of the oral mucosa; pseudomembranous colitis.
From the urinary system: dysuria, edema, impaired renal function (hypercreatininemia, increased concentration of urea in plasma), hematuria.
Allergic reactions: skin itching, skin rash, urticaria, erythema multiforme; malignant exudative erythema (Stevens-Johnson syndrome), angioedema, anaphylactic shock.
From the nervous system: headache, dizziness, paresthesia; very rarely – agitation, impaired consciousness, epileptiform seizures, convulsions.
From laboratory parameters: thrombocytosis, eosinophilia, thrombocytopenia, decrease in hemoglobin (Hb), hematocrit, leukopenia, shortening of prothrombin and partial thromboplastin time, leukocytosis, hypokalemia; gtperbilrubinemia, increased activity of alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), lactate dehydrogenase (LDH).
Local reactions: inflammation, phlebitis, thrombophlebitis, pain, swelling at the injection site; tissue damage with a concomitant increase in creatine phosphokinase (CPK) – with intramuscular administration.
Other: positive direct or indirect Coombs test, anemia, hypervolemia, vaginal candidiasis.
A cause-and-effect relationship with taking meropenem has not been established: fainting, hallucinations, depression, anxiety, increased excitability, insomnia, cholestatic hepatitis, heart failure (HF), shortness of breath, tachycardia, bradycardia, decreased or increased blood pressure (BP); cardiac arrest, myocardial infarction, pulmonary embolism (PE).
Interaction
Interaction
Compatible with 0.9% sodium chloride solution, 5-10% dextrose solution, 0.02% sodium hydrocarbonate solution, 5% dextrose solution with 0.225% sodium chloride solution, 5% dextrose solution with 0.15% potassium chloride solution, 2.5% and 10% mannitol solution.
Reduces the plasma concentration of valproic acid, which may lead to a decrease in the anticonvulsant effect. Drugs that block tubular secretion slow down excretion and increase plasma concentrations.
Overdose
Overdose
Accidental overdose is possible during treatment, especially in patients with impaired renal function.
Treatment: symptomatic. In patients with impaired renal function, meropenem and its metabolites are eliminated by hemodialysis.
Storage conditions
Storage conditions
In a place protected from light at a temperature not exceeding 25°C.
Keep out of the reach of children.
Shelf life
Shelf life
Shelf life: 2 years.
Do not use after expiration date.
Manufacturer
Manufacturer
Protek SVM, Russia
Additional information
| Shelf life | Shelf life: 2 years. Do not use after the expiration date. |
|---|---|
| Conditions of storage | Store in a light-protected place at a temperature not exceeding 25°C. Keep out of reach of children. |
| Manufacturer | Protek SVM, Russia |
| Medication form | Powder for preparation of solution |
| Brand | Protek SVM |
Related products
Buy Meropenem-LEXVM, 1 g with delivery to USA, UK, Europe and over 120 other countries.