No products in the cart.
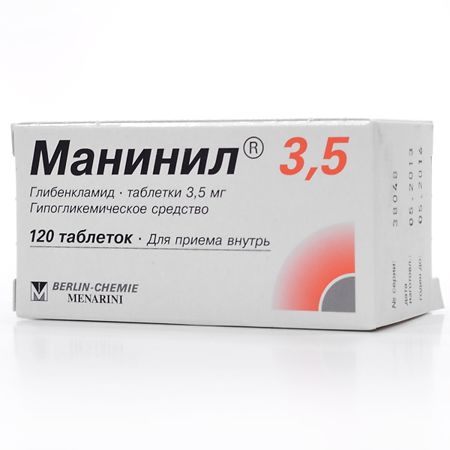
Maninil 3, 5, tablets 3,5mg 120 pcs
€5.79 €5.15
Description
Maninil is an oral hypoglycemic drug from the group of II generation sulfonylurea derivatives.
It stimulates insulin secretion through binding to specific receptors of pancreatic β-cell membrane, decreases threshold of glucose irritation of pancreatic β-cells, increases insulin sensitivity and degree of its binding to target cells, increases insulin release, increases effect of insulin on glucose absorption by muscle and liver, thereby reducing blood glucose concentration.
Acts in the second stage of insulin secretion. Inhibits lipolysis in adipose tissue. It has a hypolipidemic effect, reduces the thrombogenic properties of the blood.
Maninil® 1.5 and Maninil® 3.5 in micronized form is a high-tech, specially milled form of glibenclamide that allows the drug to be absorbed from the gastrointestinal tract faster.
Due to the earlier achievement of Cmax of glibenclamide in plasma, the hypoglycemic effect almost corresponds in time to the rise in blood glucose concentration after a meal, which makes the action of the drug milder and physiological. The duration of hypoglycemic action is 20-24 hours.
The hypoglycemic effect of the preparation Maninil® 5 develops in 2 hours and lasts 12 hours.
Indications
Indications
Type 2 diabetes mellitus – as monotherapy or as part of combination therapy with other oral hypoglycemic drugs, except sulfonylurea derivatives and glinides.
Pharmacological effect
Pharmacological effect
Maninil is an oral hypoglycemic drug from the group of sulfonylurea derivatives of the second generation.
Stimulates insulin secretion by binding to specific membrane receptors of the pancreatic β-cell, reduces the threshold of glucose irritation of pancreatic β-cells, increases sensitivity to insulin and the degree of its binding to target cells, increases the release of insulin, enhances the effect of insulin on the absorption of glucose by muscles and liver, thereby reducing the concentration of glucose in the blood.
Acts in the second stage of insulin secretion. Inhibits lipolysis in adipose tissue. It has a hypolipidemic effect, reduces the thrombogenic properties of blood.
Maninil® 1.5 and Maninil® 3.5 in micronized form are a high-tech, specially crushed form of glibenclamide, which allows the drug to be absorbed more quickly from the gastrointestinal tract.
Due to the earlier achievement of Cmax of glibenclamide in plasma, the hypoglycemic effect practically corresponds in time to the rise in blood glucose concentration after a meal, which makes the effect of the drug milder and physiological. The duration of the hypoglycemic effect is 20-24 hours.
The hypoglycemic effect of the drug Maninil® 5 develops after 2 hours and lasts 12 hours.
Special instructions
Special instructions
In elderly patients, the risk of developing hypoglycemia is slightly higher, so more careful selection of the dose of the drug and regular monitoring of fasting and postprandial blood glucose concentrations are necessary, especially at the beginning of treatment.
Alcohol can provoke the development of hypoglycemia, as well as the development of a disulfiram-like reaction (nausea, vomiting, abdominal pain, a feeling of heat on the face and upper body, tachycardia, dizziness, headache), so you should refrain from drinking alcohol during treatment with Maninil®.
Major surgical interventions and injuries, extensive burns, infectious diseases with febrile syndrome may require the abolition of oral hypoglycemic drugs and the prescription of insulin.
During treatment, prolonged exposure to the sun is not recommended.
Impact on the ability to drive vehicles and other mechanisms that require increased concentration
During the treatment period, patients should be careful when driving vehicles and other potentially dangerous activities that require increased attention and speed of psychomotor reactions.
During treatment with Maninil®, you must strictly follow your doctor’s recommendations regarding diet and self-monitoring of blood glucose concentrations.
Prolonged abstinence from eating, insufficient carbohydrate supply, intense physical activity, diarrhea or vomiting pose a risk of developing hypoglycemia.
Concomitant use of drugs that act on the central nervous system and lower blood pressure (including beta-blockers), as well as peripheral neuropathy, can mask the symptoms of hypoglycemia.
Active ingredient
Active ingredient
Glibenclamide
Composition
Composition
Active ingredients:
glibenclamide (micronized form) 3.5 mg.
Excipients:
lactose monohydrate – 63.9967 mg,
potato starch – 27.75 mg,
hymetellosis – 11 mg,
colloidal silicon dioxide – 3.5 mg,
magnesium stearate – 0.25 mg, crimson dye (Ponceau 4R) (E124) – 0.0033 mg.
Pregnancy
Pregnancy
The drug is contraindicated for use during pregnancy and breastfeeding.
If pregnancy occurs, the drug should be discontinued.
Contraindications
Contraindications
hypersensitivity to other sulfonylurea derivatives, sulfonamides, diuretics containing a sulfonamide group in the molecule, and to probenecid, since cross-reactions may occur;
Hypersensitivity to glibenclamide and/or components included in the drug;
diabetes mellitus type 1;
diabetic ketoacidosis, diabetic precoma and coma;
condition after resection of the pancreas;
severe liver failure;
severe renal failure (creatinine clearance less than 30 ml/min);
decompensation of carbohydrate metabolism in infectious diseases, burns, injuries or after major surgical operations, when insulin therapy is indicated;
leukopenia;
intestinal obstruction, gastric paresis;
hereditary lactose intolerance, lactase deficiency or glucose-lactose malabsorption syndrome;
deficiency of glucose-6-phosphate dehydrogenase;
pregnancy and lactation (breastfeeding);
children and adolescents under 18 years of age (efficacy and safety have not been studied).
The drug should be prescribed with caution: for diseases of the thyroid gland (with dysfunction), febrile syndrome, hypofunction of the anterior pituitary gland or adrenal cortex, chronic alcoholism, acute alcohol intoxication, in elderly patients (over 70 years old) due to the risk of developing hypoglycemia.
Side Effects
Side Effects
Determination of the frequency of side effects:
often (> 1/100, < 1/10); uncommon (> 1/1000, < 1/100); rare (> 1/10,000, < 1/1000); very rare (<1/10,000), including isolated reports.
From the metabolic side: often – hypoglycemia (hunger, hyperthermia, tachycardia, drowsiness, weakness, wetness of the skin, incoordination of movements, tremor, general anxiety, fear, headache, transient neurological disorders, including visual and speech disorders, the appearance of paresis or paralysis or altered perception of sensations); increase in body weight.
From the immune system: infrequently – itching, urticaria, purpura, petechiae, increased photosensitivity; very rarely – generalized allergic reactions, accompanied by skin rash, arthralgia, fever, proteinuria and jaundice; allergic vasculitis; anaphylactic shock.
From the hematopoietic system: rarely – thrombocytopenia; very rarely: leukopenia, erythropenia, agranulocytosis; in isolated cases – pancytopenia, hemolytic anemia.
From the digestive system: uncommon – nausea, feeling of heaviness in the stomach, belching, vomiting, abdominal pain, diarrhea, metallic taste in the mouth.
From the liver and biliary tract: very rarely – temporary increase in the activity of liver enzymes, intrahepatic cholestasis, hepatitis.
Other: very rarely – blurred vision and accommodation disorders, increased diuresis, transient proteinuria, hyponatremia, disulfiram-like reaction when taking alcohol (the most common signs of effect: nausea, vomiting, abdominal pain, a feeling of heat on the face and upper body, tachycardia, dizziness, headache), cross-allergy to probenecid, sulfonylurea derivatives, sulfonamides, diuretics (diuretics) containing a sulfonamide group in the molecule.
Interaction
Interaction
Strengthening the hypoglycemic effect of the drug Maninil® is possible when taken simultaneously with ACE inhibitors, anabolic agents and male sex hormones, other oral hypoglycemic agents (for example, acarbose, biguanides) and insulin, azapropazone, NSAIDs, beta-blockers, quinolone derivatives, chloramphenicol, clofibrate and its analogues, coumarin derivatives, disopyramide, fenfluramine, antifungal drugs (miconazole, fluconazole), fluoxetine, MAO inhibitors, PAS, pentoxifylline (in high doses when administered parenterally), perhexiline, pyrazolone derivatives, phosphamides (for example, cyclophosphamide, ifosfamide, trophosfamide), probenecid, salicylates, sulfonamides, tetracyclines and tritoqualine.
Urine acidifying agents (ammonium chloride, calcium chloride) enhance the effect of the drug Maninil® by reducing the degree of its dissociation and increasing its reabsorption.
The hypoglycemic effect of the drug Maninil® may be reduced with the simultaneous use of barbiturates, isoniazid, diazoxide, corticosteroids, glucagon, nicotinates (in high doses), phenytoin, phenothiazines, rifampicin, thiazide diuretics, acetazolamide, oral contraceptives and estrogens, thyroid hormone preparations, sympathomimetic agents, slow calcium channel blockers, lithium salts.
H2 receptor antagonists can, on the one hand, weaken and, on the other hand, enhance the hypoglycemic effect of the drug Maninil®.
Pentamidine in isolated cases can cause a strong decrease or increase in blood glucose concentrations.
When used simultaneously with the drug Maninil®, the effect of coumarin derivatives may be enhanced or weakened.
Along with enhancing the hypoglycemic effect, beta-blockers, clonidine, guanethidine and reserpine, as well as drugs with a central mechanism of action, can reduce the feeling of warning signs of hypoglycemia.
Overdose
Overdose
Symptoms: hypoglycemia (hunger, hyperthermia, tachycardia, drowsiness, weakness, wetness of the skin, loss of coordination of movements, tremor, general anxiety, fear, headache, transient neurological disorders (for example, visual and speech disorders, manifestations of paresis or paralysis or altered perception of sensations). As hypoglycemia progresses, the patient may lose self-control and consciousness, developing a hypoglycemic coma.
Treatment: for mild hypoglycemia, the patient should take a piece of sugar, food or drinks with a high sugar content (jam, honey, a glass of sweet tea). In case of loss of consciousness, it is necessary to administer intravenous glucose – 40-80 ml of a 40% dextrose (glucose) solution, then an infusion of a 5-10% dextrose solution. Then you can additionally administer 1 mg of glucagon intravenously, intramuscularly or subcutaneously. If the patient does not regain consciousness, then this measure can be repeated; further intensive therapy may be required.
Storage conditions
Storage conditions
At a temperature not exceeding 25 °C
Shelf life
Shelf life
3 years
Manufacturer
Manufacturer
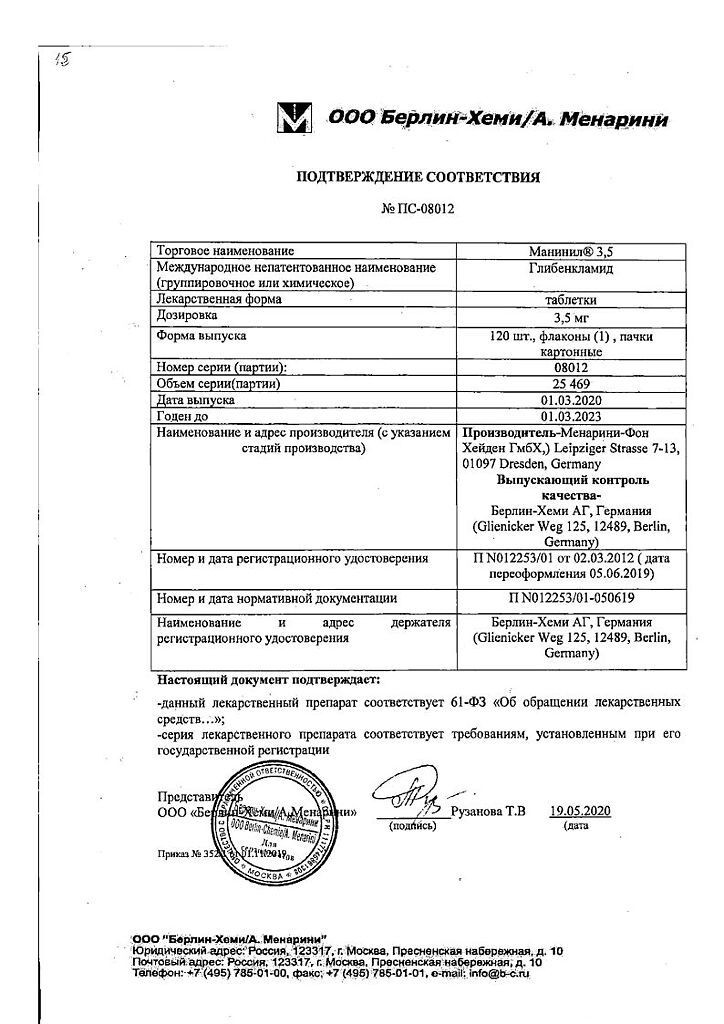
Berlin-Chemie/Menarini, Germany
Additional information
| Shelf life | 3 years |
|---|---|
| Conditions of storage | At a temperature not exceeding 25 °C |
| Manufacturer | Berlin-Chemie/Menarini, Germany |
| Medication form | pills |
| Brand | Berlin-Chemie/Menarini |
Other forms…
Related products
Buy Maninil 3, 5, tablets 3,5mg 120 pcs with delivery to USA, UK, Europe and over 120 other countries.