No products in the cart.
Clarithromycin, 500 mg 14 pcs
€18.29 €15.25
Description
Pharmacological action – broad spectrum antibacterial.
Pharmacological action:
Clarithromycin is a broad spectrum semi-synthetic macrolide antibiotic. Antibacterial activity of clarithromycin is carried out by inhibition of protein synthesis due to binding to 50s-subunit of bacterial ribosomes. Clarithromycin has pronounced activity against a wide range of aerobic and anaerobic gram-positive and gram-negative organisms. Minimum inhibitory concentration of clarithromycin (MIC) is half that of erythromycin for most microorganisms.
The 14-hydroxy metabolite of clarithromycin also has antimicrobial activity. Minimum inhibitory concentrations of this metabolite are equal to or greater than the MAC of clarithromycin; against H. influenzae 14-hydroxy metabolite is twice as active as clarithromycin.
Clarithromycin has in vitro activity against the following organisms – Gram-positive aerobic bacteria: Staphylococcus aureus (sensitive to methicillin), Streptococcus agalactiae, Streptococcus pyogenes, Streptococcus pneumonia, Streptococcus viridans and Listeria monocytogenes; Gram-negative aerobic bacteria: Haemophilus influenzae, Haemophilus parainfluenzae, Moraxella (Branhamella) catarrhalis, Neisseria gonorrhoea, Legionella pneumophila, Bordetella pertussis, Helicobacter pylori, Campylobacter jejuni; mainly intracellular microorganisms: Mycoplasma pneumonia, Ureaplasma urealyticum, Chlamydia trachomatis, Chlamydia pneumonia, Mycobacterium avium, Mycobacterium leprae, M. kansaii, M. chelonae, M. marinum, M. fortitum; anaerobic microorganisms: Bacteroides fragilis, Clostridium perfringens, Propionibacterium acnes, Peptococcus species; Peptostreptococcus species. In addition, the drug is active against Toxoplasma species.
Bactericidal activity of clarithromycin is against some bacterial strains: Haemophilus influenzae; Streptococcus pneumoniae; Streptococcus pyogenes; Streptococcus agalactiae; Moraxella (Branhamella) catarrhalis; Neisseria gonorrhoeae; Helicobacter pylori and Campylobacter spp.
Pharmacokinetics:
Clarithromycin is quickly and well absorbed from the gastrointestinal tract after oral administration. The microbiologically active metabolite 14-hydroxyclarithromycin is formed after the first passage through the liver. Food intake has no effect on the bioavailability of clarithromycin; however, it slightly slows down the onset of clarithromycin absorption and the formation of the 14-hydroxy metabolite. The pharmacokinetics of clarithromycin are nonlinear, with equilibrium concentration reached 2 days after initiation of the drug.
Clarithromycin is excreted with the urine and also with the feces, mainly through the bile. When taking 250 mg of clarithromycin 2 times per day. 15-20% of the administered dose is excreted unchanged in the urine. When administered 500 mg 2 times/day, urinary excretion is about 36%. 14-hydroxyclarithromycin is the main metabolite found in the urine, accounting for about 10-15%.
The plasma concentration of clarithromycin is higher when 500 mg of clarithromycin is taken 3 times/day than when this dose is taken 2 times/day.
Clarithromycin content in tissues, including glandular and pulmonary tissue, is several times higher than in circulating blood. At therapeutic concentrations, clarithromycin is 80% bound to plasma proteins.
Clarithromycin penetrates gastric mucus. Clarithromycin levels in gastric mucus and tissues are increased when combined therapy with omeprazole. Clarithromycin penetrates into breast milk.
Indications
Indications
Infections caused by microorganisms sensitive to clarithromycin:
– lower respiratory tract infections (including acute and chronic bronchitis, pneumonia);
– upper respiratory tract infections (including sinusitis and pharyngitis);
– infections of the skin and soft tissues;
— duodenal ulcer for eradication of Helicobacter pylori (as part of complex therapy with proton pump inhibitors).
Pharmacological effect
Pharmacological effect
Pharmacological action – broad spectrum antibacterial.
Pharmaceutical action:
Clarithromycin is a semisynthetic broad-spectrum macrolide antibiotic. The antibacterial effect of clarithromycin is carried out by suppressing protein synthesis due to binding to the 50s subunit of bacterial ribosomes. Clarithromycin has pronounced activity against a wide range of aerobic and anaerobic gram-positive and gram-negative organisms. The minimum inhibitory concentration (MIC) of clarithromycin is half that of erythromycin for most microorganisms.
The 14-hydroxy metabolite of clarithromycin also has antimicrobial activity. The minimum inhibitory concentrations of this metabolite are equal to or greater than the MIC of clarithromycin; against H. influenzae, the 14-hydroxy metabolite is twice as active as clarithromycin.
Clarithromcin is active in vitro against the following organisms – gram-positive aerobic bacteria: Staphylococcus aureus (sensitive to methicillin), Streptococcus agalactiae, Streptococcus pyogenes, Streptococcus pneumonia, Streptococcus viridans and Listeria monocytogenes; gram-negative aerobic bacteria: Haemophilus influenzae, Haemophilus parainfluenzae, Moraxella (Branhamella) catarrhalis, Neisseria gonorrhoea, Legionella pneumophila, Bordetella pertussis, Helicobacter pylori, Campylobacter jejuni; predominantly intracellular microorganisms: Mycoplasma pneumonia, Ureaplasma urealyticum, Chlamydia trachomatis, Chlamydia pneumonia, Mycobacterium avium, Mycobacterium leprae, M. kansaii, M. chelonae, M. marinum, M. fortitum; anaerobic microorganisms: Bacteroides fragilis, Clostridium perfringens, Propionibacterium acnes, Peptococcus species; Peptostreptococcus species. In addition, the drug is active against Toxoplasma species.
Clarithromycin has bactericidal activity against certain bacterial strains: Haemophilus influenzae; Streptococcus pneumoniae; Streptococcus pyogenes; Streptococcus agalactiae; Moraxella (Branhamella) catarrhalis; Neisseria gonorrhoeae; Helicobacter pylori and Campylobacter spp.
Pharmacokinetics:
Clarithromycin is quickly and well absorbed from the gastrointestinal tract after oral administration. The microbiologically active metabolite 14-hydroxyclarithromycin is formed after the first passage through the liver. Food intake does not affect the bioavailability of clarithromycin; however, it slightly slows down the onset of absorption of clarithromycin and the formation of the 14-hydroxy metabolite. The pharmacokinetics of clarithromycin is nonlinear; in this case, the equilibrium concentration is achieved 2 days after starting the drug.
Clarithromycin is excreted in the urine and also in feces, mainly through bile. When taking 250 mg of clarithromycin 2 times a day. 15-20% of the administered dose is excreted unchanged in the urine. When taking 500 mg 2 times a day. urinary excretion is about 36%. 14-hydroxyclarithromycin is the main metabolite found in urine, accounting for about 10-15%.
When taking 500 mg of clarithromycin 3 times a day. The concentration of clarithromycin in plasma is higher than when taking this dose 2 times a day.
The content of clarithromycin in tissues, including glandular and pulmonary tissue, is several times higher than in circulating blood. At therapeutic concentrations, clarithromycin is 80% bound to plasma proteins.
Clarithromycin penetrates gastric mucus. The level of clarithromycin in gastric mucus and tissue increases during combination therapy with omeprazole. Clarithromycin passes into breast milk.
Special instructions
Special instructions
The use of clarithromycin tablets in children under 12 years of age is not recommended.
When clarithromycin and warfarin are co-administered, prothrombin time should be regularly monitored.
When clarithromycin and digoxin are co-administered, the level of digoxin concentration in the blood serum should be monitored.
Active ingredient
Active ingredient
Clarithromycin
Composition
Composition
1 film-coated tablet:
active ingredient:
clarithromycin 500 mg
excipients: povidone – 20 mg; MCC – 324 mg; croscarmellose sodium – 40 mg; colloidal silicon dioxide – 6 mg; magnesium stearate – 10 mg,
film shell: Opadry II white (hypromellose – 34.95%, lactose monohydrate – 27.18%, titanium dioxide – 25.24%, macrogol 4000 – 9.7%, sodium citrate dihydrate – 2.93%) – 20 mg.
Contraindications
Contraindications
– hypersensitivity to clarithromycin and other components of the drug, as well as hypersensitivity to other macrolide antibiotics;
– simultaneous use of clarithromycin with the following drugs: astemizole, cisapride, pimozide, terfenadine, ergot alkaloids (for example, ergotamine, dihydroergotamine), midazolam for oral use (see “Interaction with other drugs”);
– simultaneous use of clarithromycin with HMG-CoA reductase inhibitors (statins), which are largely metabolized by the CYP3A4 isoenzyme (lovastatin, simvastatin), due to an increased risk of myopathy, including rhabdomyolysis;
– simultaneous use of colchicine in patients with impaired liver and/or kidney function;
– simultaneous use of P-glycoprotein inhibitors or potent inhibitors of the CYP3A4 isoenzyme;
– patients with a history of QT interval prolongation or ventricular arrhythmia, including polymorphic ventricular tachycardia (“torsade de pointes”);
– severe renal failure (creatinine clearance less than 30 ml/min), simultaneous use of clarithromycin with ticagrelor or ranolazine;
– severe liver failure occurring simultaneously with renal failure;
– cholestatic jaundice/hepatitis that occurred during the use of clarithromycin (history);
– porphyria;
– hypokalemia (risk of QT interval prolongation);
– lactation period (breastfeeding);
– children under 12 years of age (efficacy and safety have not been established);
– lactose intolerance, lactase deficiency, glucose-galactose malabsorption.
With caution
– renal failure of moderate severity;
– liver failure of moderate and severe severity;
– IHD, severe heart failure, severe bradycardia (less than 50 beats/min);
– simultaneous use of clarithromycin with other ototoxic drugs, especially aminoglycosides;
– simultaneous use of clarithromycin with statins that are independent of the metabolism of the CYP3A isoenzyme (for example, fluvastatin);
– simultaneous use with benzodiazepines, such as alprazolam, triazolam, midazolam for intravenous use;
– simultaneous use with drugs that are metabolized by the CYP3A4 isoenzyme, for example, carbamazepine, cilostazol, cyclosporine, disopyramide, methylprednisolone, omeprazole, indirect anticoagulants (for example: warfarin), quinidine, rifabutin, sildenafil, tacrolimus, vinblastine;
– simultaneous use with drugs that induce the CYP3A4 isoenzyme (for example: rifampicin, phenytoin, carbamazepine, phenobarbital, St. John’s wort);
– simultaneous use with blockers of “slow” calcium channels that are metabolized by the CYP3A4 isoenzyme (for example: verapamil, amlodipine, diltiazem);
– simultaneous use of class IA (quinidine, procainamide) and class III antiarrhythmic drugs (dofetilide, amiodarone, sotalol);
– hypomagnesemia;
– pregnancy.
Side Effects
Side Effects
Clarithromycin is generally well tolerated by patients
From the gastrointestinal tract: nausea, vomiting, dyspepsia, diarrhea, abdominal pain, stomatitis, glossitis, pancreatitis, oral candidiasis, discoloration of the tongue and teeth; rarely – pseudomembranous enterocolitis. Tooth discoloration is reversible and can usually be restored with special treatment at a dental clinic. As with other antibiotics from the macrolide group, liver function disorders are possible, incl. increased activity of liver enzymes, hepatocellular and/or cholestatic hepatitis with or without jaundice. These liver problems can be severe, but are usually reversible. Very rare cases of liver failure and death have been observed, mainly due to severe concomitant diseases and/or concomitant drug therapy.
From the blood system: in exceptional cases – leukopenia and thrombocytopenia; increase in serum creatinine level.
From the central and peripheral nervous system: paresthesia, headache, disturbances of smell, changes in taste; dizziness, agitation, insomnia, nightmares, fear, ringing in the ears, confusion, disorientation, hallucinations, psychosis, depersonalization; reversible hearing loss; convulsions.
From the cardiovascular system: as with other macrolides, prolongation of the QT interval, ventricular tachycardia, polymorphic ventricular tachyarrhythmia (torsades de pointes).
From the musculoskeletal system: arthralgia, myalgia.
From the urinary system: isolated cases of increased plasma creatinine, interstitial nephritis, renal failure.
Allergic reactions: urticaria, angioedema, anaphylactic shock, in rare cases – Stevens-Johnson syndrome, toxic elidermal necrolysis.
Other: rarely – hypoglycemia in patients taking oral hypoglycemic drugs or insulin.
Interaction
Interaction
When clarithromycin is co-administered with cisapride, pimozide and terfenadine, increased plasma concentrations of these drugs are observed, which can cause prolongation of the QT interval and cardiac arrhythmias, including ventricular tachycardia, ventricular fibrillation, arrhythmia and torsade de pointes; similar effects are observed when taking astemizole and other macrolides simultaneously.
Clarithromycin does not interact with oral contraceptives.
As with other macrolide antibiotics, concomitant use of clarithromycin and other drugs metabolized by cytochrome P450 (warfarin, ergot alkaloids, triazolam, midazolam, disopyramide, lovastatin, rifabutin, phenytoin, cyclosporine and tacrolimus) may be accompanied by an increase in the concentration of these drugs in the blood serum.
With simultaneous use of clarithromycin and HMG-KoA reductase inhibitors (lovastatin, simvastatin), rhabdomyolysis may develop.
With the simultaneous administration of clarithromycin and theophylline, the concentration of theophylline in the blood serum and its toxicity increase.
The simultaneous administration of clarithromycin and warfarin or digoxin may be accompanied by an increase in the severity of their effects.
With the simultaneous administration of clarithromycin and carbamazepine, the effect of carbamazepine may be enhanced due to a decrease in the rate of excretion of carbamazepine.
When clarithromycin and zidovudine (orally) are taken simultaneously in HIV-infected adult patients, the steady-state concentration of zidovudine may decrease; this can be largely avoided by increasing the interval between doses of clarithromycin and zidovudine to 1-2 hours. For children, such an interaction was not observed.
When taking ritonavir and clarithromycin simultaneously, the values of the pharmacokinetic parameters for the latter increase: AUC, Cmax, Cmin. For patients with normal renal function, no dose adjustment is usually required due to the wide therapeutic dosage range of clarithromycin.
With the simultaneous use of clarithromycin and omeprazole, clarithromycin and lansoprazole, as well as clarithromycin and ranitidine, an increase in the concentration of drugs in the blood plasma is possible, but usually no dose adjustment is required.
With the simultaneous use of clarithromycin and hypoglycemic agents, including insulin, in rare cases, hypoglycemia may develop.
Overdose
Overdose
Symptoms: gastrointestinal symptoms; one of the patients, when taking 8 g of clarithromycin, had a case of mental state disturbance, paranoid behavior, hypoglycemia, hypoxemia.
Treatment: gastric lavage, maintenance therapy. Hemodialysis or peritoneal dialysis is ineffective, as for other macrolides.
Storage conditions
Storage conditions
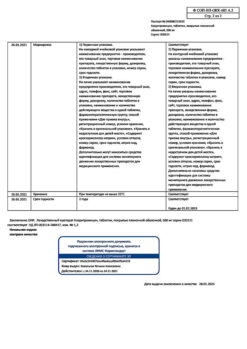
At a temperature not exceeding 25 °C.
Keep out of the reach of children.
Shelf life
Shelf life
2 years. Do not use after the expiration date stated on the package.
Manufacturer
Manufacturer
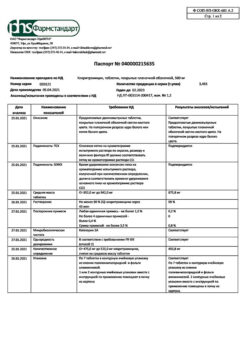
Pharmstandard-Tomskkhimpharm, Russia
Additional information
| Shelf life | 2 years. Do not use after the expiration date stated on the package. |
|---|---|
| Conditions of storage | At a temperature not higher than 25 ° C. Keep out of reach of children. |
| Manufacturer | Pharmstandard-Tomskkhimpharm, Russia |
| Medication form | sustained release tablets |
| Brand | Pharmstandard-Tomskkhimpharm |
Other forms…
Related products
Buy Clarithromycin, 500 mg 14 pcs with delivery to USA, UK, Europe and over 120 other countries.