No products in the cart.
Description
Pharmgroup:
Cephalosporin antibiotic.
Pharmic action:
Claforan is a semi-synthetic antibiotic of the group of cephalosporins of generation III for parenteral use. Cefotaxime acts bactericidally. It is also resistant to the action of most B-lactamases.
The following are usually sensitive to the drug: Aeromonas hydrophila; Bacillus subtilis; Bordetella pertussis; Borrelia burgdorferi; Moraxella (Branhamella) catarrhalis; Citrobacter diversus; Clostridium perfringens; Corynebacterium diphtheriae; Escherichia coli; Enterobacter spp. (sensitivity depends on epidemiological data and on the level of resistance in each particular country); Erysipelothrix insidiosa; Eubacterium; Haemophilus penicillin- and nonpenicillin-forming strains, including ampi-R; Klebsiella pneumoniae; Klebsiella oxytoca; Methi-S-Staphylococcus, including penicillin- and nonpenicillin-derived strains; Morganella morganii; Neisseria gonorrhoeae, including penicillin- and nonpenicillin-derived strains; Neisseria meningitidis; Propionibacterium; Proteus mirabilis, vulgaris; Providencia; Streptococcus pneumoniae, Salmonella; Seratia spp. (sensitivity depends on epidemiological data and on the level of resistance in each country); Shigella, Streptococcus spp.; Veillonella; Yersinia (sensitivity depends on epidemiological data and on the level of resistance in each country).
The following are resistant to Claforan drug: Acinetobacter baumannii, Bacteroides fragilis; Clostridium difficile; Enterococcus; Gram-negative anaerobes; Listeria monocytogenes, Methi-R staphylococcus; Pseudomonas aeruginosa, Pseudomonas cepacia; Stenotrophomonas maltophilia.
Pharmacokinetics: In adults – 5 minutes after a single IV administration of 1 g of cefotaxime the concentration in blood plasma is 100 µg/ml. After intravenous administration of cefotaxime in the same dose the maximum concentration in plasma is detected after 0.5 hours and is 20 to 30 mcg/ml.
The T1/2 of Claforan is 1 h when administered intravenously and 1-1.5 h when administered intravenously.
The binding to plasma proteins (predominantly albumins) is on average 25-40%.
About 90% of the administered dose is excreted in the urine: 50% unchanged and about 20% as the metabolite deacetylcephotaxime.
The T1/2 of cefotaxime is increased up to 2.5 h in the elderly (over 80 years).
In adults with impaired renal function, the volume of distribution does not change and the T1/2 does not exceed 2.5 h, even in the last stages of renal failure.
In children, neonates and preterm infants, plasma cefotaxime levels and volume of distribution are similar to those in adults receiving the same dose of the drug in mg/kg. The T1/2 of cefotaxime is 0.75 to 1.5 h.
In neonates and preterm infants, plasma levels of cefotaxime and volume of distribution are similar to those in children. The average T1/2 of cefotaxime is 1.4 to 6.4 h.
Indications
Indications
Cefotaxime is intended for the treatment of infections caused by microorganisms sensitive to the drug.
septicemia, bacteremia;
endocarditis;
respiratory tract infections;
urinary tract infections;
intra-abdominal infections (including peritonitis);
meningitis (except listeria) and other CNS infections;
skin and soft tissue infections;
bone and joint infections;
Prevention of infections after surgical operations on the gastrointestinal tract, urological and obstetric-gynecological operations.
Pharmacological effect
Pharmacological effect
Pharmaceutical group:
Antibiotic cephalosporin.
Pharmaceutical action:
Klaforan is a semisynthetic antibiotic of the third generation cephalosporin group for parenteral use. Cefotaxime is bactericidal. It is also resistant to most B-lactamases.
The following are usually sensitive to the drug: Aeromonas hydrophila; Bacillus subtilis; Bordetella pertussis; Borrelia burgdorferi; Moraxella (Branhamella) catarrhalis; Citrobacter diversus; Clostridium perfringens; Corynebacterium diphtheriae; Escherichia coli; Enterobacter spp. (sensitivity depends on epidemiological data and the level of resistance in each specific country); Erysipelothrix insidiosa; Eubacterium; Haemophilus penicillinase-forming and non-penicillinase-forming strains, including ampi-R; Klebsiella pneumoniae; Klebsiella oxytoca; Methi-S-Staphylococcus, including penicillinase-forming and non-penicillinase-forming strains; Morganella morganii; Neisseria gonorrhoeae, including penicillinase-forming and non-penicillinase-forming strains; Neisseria meningitidis; Propionibacterium; Proteus mirabilis, vulgaris; Providencia; Streptococcus pneumoniae, Salmonella; Seratia spp. (sensitivity depends on epidemiological data and the level of resistance in each specific country); Shigella, Streptococcus spp.; Veillonella; Yersinia (sensitivity depends on epidemiological data and the level of resistance in each specific country).
The following are resistant to Klaforan: Acinetobacter baumannii, Bacteroides fragilis; Clostridium difficile; Enterococcus; gram-negative anaerobes; Listeria monocytogenes, Methi-R staphylococcus; Pseudomonas aeruginosa, Pseudomonas cepacia; Stenotrophomonas maltophilia.
Pharmacokinetics: In adults, 5 minutes after a single intravenous injection of 1 g of cefotaxime, the concentration in the blood plasma is 100 mcg/ml. After intramuscular administration of cefotaxime at the same dose, the maximum concentration in the blood plasma is detected after 0.5 hours and ranges from 20 to 30 mcg/ml.
T1/2 of the drug Klaforan is 1 hour with intravenous administration and 1–1.5 hours with intramuscular administration.
Binding to plasma proteins (mainly albumin) averages 25–40%.
About 90% of the administered dose is excreted in the urine: 50% unchanged and about 20% as a metabolite of desacetylcefotaxime.
In the elderly (over 80 years old), T1/2 of cefotaxime increases to 2.5 hours.
In adults with impaired renal function, the volume of distribution does not change, and T1/2 does not exceed 2.5 hours, even in the last stages of renal failure.
In children, newborns and premature infants, cefotaxime plasma levels and volume of distribution are similar to those in adults receiving the same mg/kg dose of the drug. T1/2 of cefotaxime ranges from 0.75 to 1.5 hours.
In neonates and prematurely born children, cefotaxime plasma levels and volume of distribution are similar to those in children. The average T1/2 of cefotaxime ranges from 1.4 to 6.4 hours.
Special instructions
Special instructions
Anaphylactic reactions:
the prescription of cephalosporins requires the collection of an allergic history (allergic diathesis, hypersensitivity reactions to β-lactam antibiotics);
if the patient develops a hypersensitivity reaction, treatment should be discontinued;
the use of cefotaxime is strictly contraindicated in patients with a history of an immediate hypersensitivity reaction to cephalosporins. If there is any doubt, the presence of a doctor during the first administration of the drug is mandatory, due to a possible anaphylactic reaction.
Cross-allergy between cephalosporins and penicillins is known, which occurs in 5-10% of cases. In persons with a history of allergy to penicillins, the drug is used with extreme caution.
Pseudomembranous colitis.
In the first weeks of treatment, pseudomembranous colitis may occur, manifested by severe, prolonged diarrhea. The diagnosis is confirmed by colonoscopy and/or histological examination. This complication is regarded as very serious: the administration of Claforan is immediately stopped and adequate therapy is prescribed, including oral vancomycin or metronidazole.
Active ingredient
Active ingredient
Cefotaxime
Composition
Composition
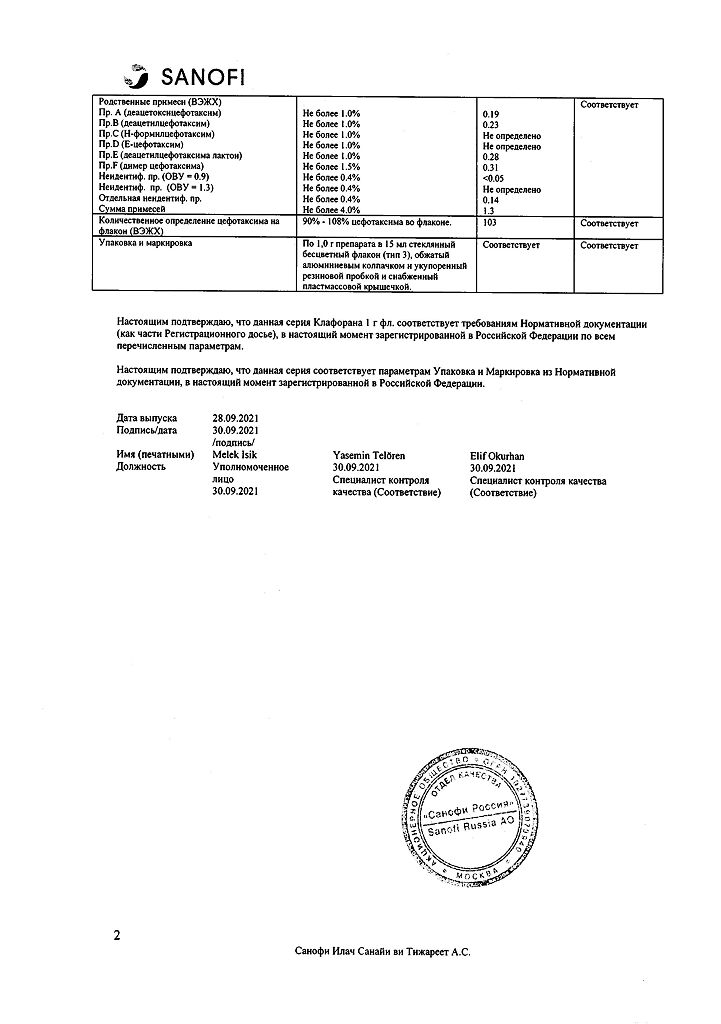
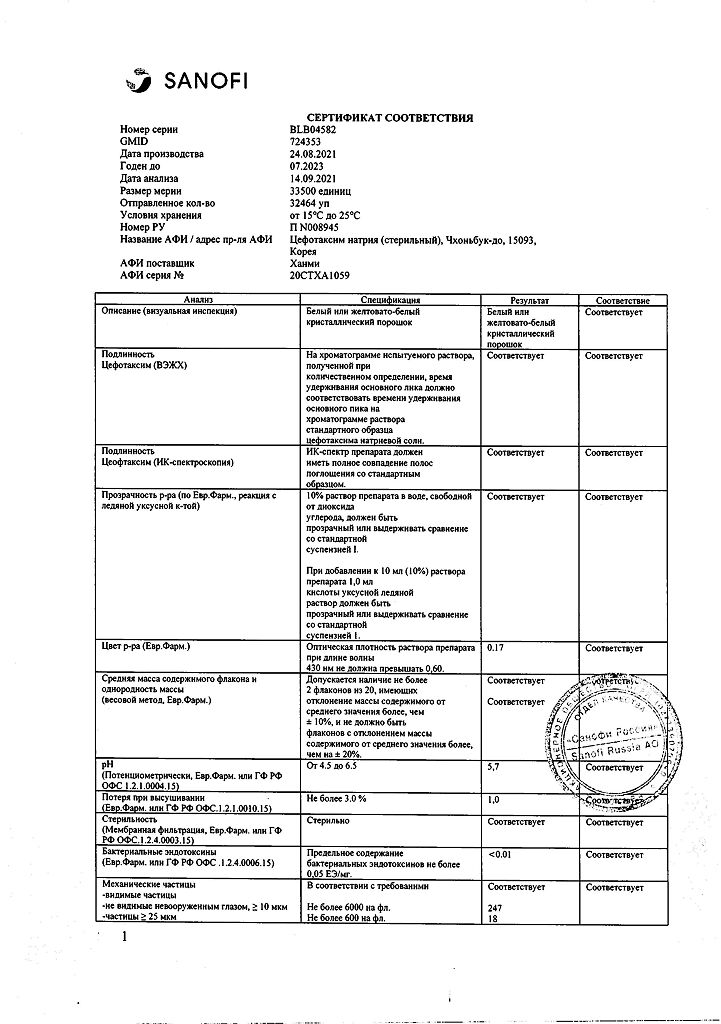
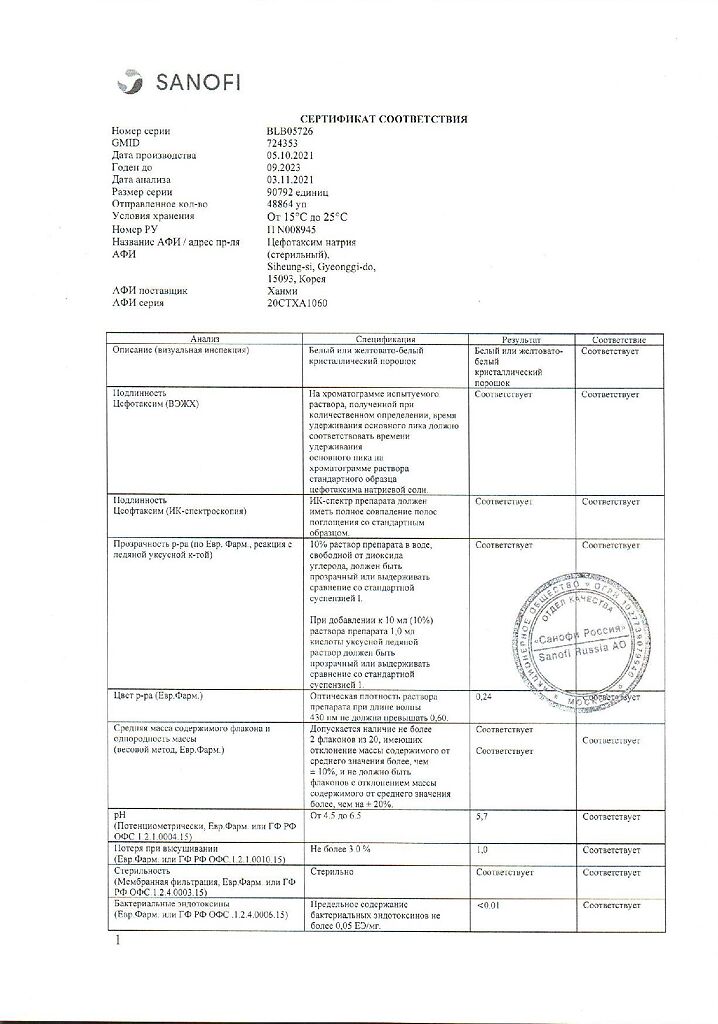
One bottle contains 1 g of sterile cefotaxime powder, which corresponds to 1.048 g of cefotaxime sodium salt.
Pregnancy
Pregnancy
Cefotaxime passes into breast milk, so if it is necessary to prescribe the drug, breastfeeding should be interrupted.
Cefotaxime penetrates the placental barrier. Studies conducted on animals did not reveal the teratogenic effect of the drug. However, the safety of cefotaxime during pregnancy in humans has not been determined and the drug should not be used during pregnancy.
Contraindications
Contraindications
hypersensitivity to lidocaine or other amide-type local anesthetic;
intrasedial blockades without an established pacemaker;
hypersensitivity to cephalosporins;
for forms containing lidocaine:
severe heart failure;
intravenous administration
children under 2.5 years of age (intramuscular administration)
Side Effects
Side Effects
Anaphylactic reactions: angioedema, bronchospasm, weakness, rarely – anaphylactic shock.
Skin reactions: rash, redness, urticaria. As with other cephalosporins, complications such as erythema multiforme, Stevens-Johnson syndrome, and toxic skin necrosis are very rarely possible.
Gastrointestinal reactions: nausea, vomiting, abdominal pain, diarrhea may occur. As with the prescription of other broad-spectrum antibiotics, diarrhea can be a symptom of enterocolitis, which in some cases is accompanied by the appearance of blood in the stool. A special form of enterocolitis is pseudomembranous colitis (see “Special Instructions”).
Liver reactions: increased liver enzymes (ALT, AST, LDH, gamma-GT, alkaline phosphatase) and/or bilirubin.
Reactions from peripheral blood: neutropenia, rarely – agranulocytosis, eosinophilia, thrombocytopenia, isolated cases of hemolytic anemia.
Reactions from the kidneys: deterioration of renal function (increased creatinine levels), especially when combined with aminoglycosides, very rarely cases of interstitial nephritis have been reported.
Reactions from the central nervous system: encephalopathy (in case of large doses), especially in patients with renal failure.
Reactions from the cardiovascular system: in isolated cases of arrhythmia, following bolus administration through a central venous catheter (see “Method and duration of use”).
Other: fever, inflammation at the injection site, superinfection.
When treating borreliosis: Jarisch-Herxheimer reaction (during the first days of treatment), skin rash, itching, fever, leukopenia, increased levels of liver enzymes, difficulty breathing and discomfort in the joints.
In addition to the above, the rate of administration of the drug should be monitored (See “Dosage and Administration”), as well as renal function should be monitored in all cases of combined use of cefotaxime with aminoglycosides.
In patients requiring sodium restriction, the sodium content of cefotaxime sodium salt (48.2 mg/g) should be taken into account. If the course of treatment lasts more than 10 days, the leukocyte count should be monitored and, in case of neutropenia, treatment should be discontinued.
Interaction
Interaction
Compatibility instructions: cefotaxime should not be mixed with other antibiotics, either in the same syringe or in the same infusion solution. This also applies to aminoglycosides.
For infusions, the following solutions can be used (cefotaxime concentration 1 g/250 ml): water for injection, 0.9% sodium chloride solution, 5% dextrose, Ringer’s solution, sodium lactate, as well as: Hemaccel, Yonosteril, Macrodex 6%, Reomacrodex 12%, Tutofusin V.
Probenicid delays excretion and increases plasma concentrations of cephalosporins.
As with other cephalosporins, cefotaxime may potentiate the nephrotoxic effect of drugs that have nephrotoxic effects.
During therapy with cephalosporins, a positive Coombs test may occur.
It is recommended to use glucose oxidase methods for determining blood sugar levels, due to the development of false-positive results when using nonspecific reagents.
Overdose
Overdose
There is a risk of developing reversible encephalopathy when using high doses of β-lactam antibiotics, including cefotaxime. There is no specific antidote.
Storage conditions
Storage conditions
In a place protected from light, at a temperature not exceeding 25 °C
Shelf life
Shelf life
2 years
Manufacturer
Manufacturer
Sanofi Ilac Sanayi ve Ticaret A.Ş., Türkiye
Additional information
| Shelf life | 2 years |
|---|---|
| Conditions of storage | In a light-protected place, at a temperature not exceeding 25 °C |
| Manufacturer | Sanofi Ilac Sanayi ve Ticaret A.Ş., Turkey |
| Medication form | Powder for preparation of solution |
| Brand | Sanofi Ilac Sanayi ve Ticaret A.Ş. |
Related products
Buy Claforan, 1 g with delivery to USA, UK, Europe and over 120 other countries.