No products in the cart.
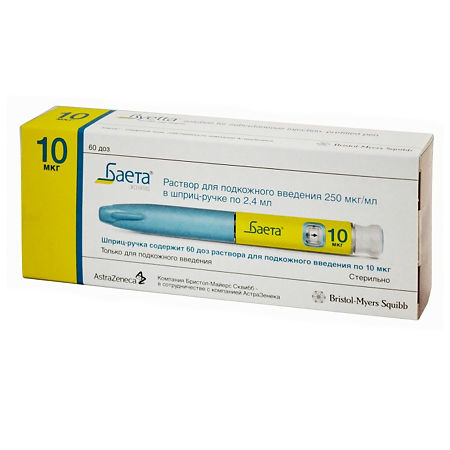
Baeta, 250 µg/ml 2.4ml syringe pen cartridges
€204.42 €170.35
Out of stock
(E-mail when Stock is available)
Description
Baeta is a hypoglycemic drug.
Pharmacodynamics
Exenatide (exendin-4) is an incretin mimetic and is a 39-amino acid amidopeptide. Incretins such as glucagon-like peptide-1 (GFP-1) increase glucose-dependent insulin secretion, improve β-cell function, inhibit inadequately elevated glucagon secretion, and slow gastric emptying after they enter the general bloodstream from the gut. Exenatide is a potent incretin mimetic that causes increased glucose-dependent insulin secretion and has other hypoglycemic effects inherent to incretins to improve glycemic control in patients with type 2 diabetes.
The amino acid sequence of exenatide partially matches that of human GFP-1, whereby it binds to and activates human GFP-1 receptors, resulting in enhanced glucose-dependent insulin synthesis and secretion from pancreatic β-cells involving cyclic AMP and/or other intracellular signaling pathways.
Exenatide stimulates insulin release from β-cells in the presence of elevated glucose concentrations.
Exenatide differs chemically and pharmacologically from insulin, sulfonylurea derivatives, D-phenylalanine derivatives and meglitinides, biguanides, thiazolidinediones and alpha-glucosidase inhibitors.
Exenatide improves glycemic control in patients with type 2 diabetes through the following mechanisms.
In hyperglycemic states, exenatide increases glucose-dependent insulin secretion from pancreatic β-cells. This insulin secretion stops as blood glucose concentrations decrease and approach normal, thereby reducing the potential risk of hypoglycemia.
Insulin secretion during the first 10 minutes (in response to a rise in glycemia), known as the “first phase of insulin response,” is specifically absent in patients with type 2 diabetes. In addition, loss of the first phase of the insulin response is an early disruption of β-cell function in type 2 diabetes. Administration of exenatide restores or significantly enhances both the first and second phases of insulin response in patients with type 2 diabetes.
In patients with type 2 diabetes mellitus against a background of hyperglycemia, administration of exenatide suppresses excessive glucagon secretion. However, exenatide does not disrupt the normal glucagon response to hypoglycemia.
The administration of exenatide has been shown to decrease appetite and food intake; it suppresses gastric motility, leading to delayed gastric emptying.
In patients with type 2 diabetes, therapy with exenatide in combination with metformin, thiazolidinedione and/or sulfonylureas leads to decreased fasting blood glucose concentration, postprandial blood glucose, and HbA1c, thereby improving glycemic control in these patients.
Pharmacokinetics
Intake. After subcutaneous administration of exenatide at a dose of 10 mcg in patients with type 2 diabetes mellitus, exenatide is rapidly absorbed and reaches Cmax in 2.1 hours, which is 211 pg/mL. The AUCo-inf is 1036 pg×h/ml. When exposed to exenatide, the AUC increases in proportion to the increase in dose from 5 to 10 micrograms, while there is no proportional increase in Cmax. The same effect was observed when exenatide was administered p/c to the abdomen, thigh or forearm.
Distribution. The apparent volume of distribution (Vd) of exenatide after p/k administration is 28.3 liters.
Metabolism and excretion. Exenatide is mainly excreted by glomerular filtration followed by proteolytic breakdown. Clearance of exenatide is 9.1 l/hour. The final T1/2 is 2.4 hours. These pharmacokinetic characteristics of exenatide are not dose dependent. Measurable concentrations of exenatide are determined within approximately 10 hours after administration of the dose.
Pharmacokinetics in special clinical cases. In patients with mild to moderately severe renal impairment (creatinine Cl 30-80 ml/min), the clearance of exenatide is not significantly different from that of patients with normal renal function; therefore, no dose adjustment is required. However, in patients with end-stage renal failure on dialysis, average clearance is reduced to 0.9 l/h (compared to 9.1 l/h in healthy subjects).
Because exenatide is primarily excreted by the kidneys, impaired liver function is not thought to alter exenatide blood concentrations.
Age has no effect on the pharmacokinetic characteristics of exenatide. Therefore, elderly patients do not require dose adjustments.
The pharmacokinetics of exenatide in children has not been studied.
There are no clinically significant differences in the pharmacokinetics of exenatide between men and women.
The pharmacokinetics of Exenatide are virtually unchanged between races. There is no need to make dose adjustments based on ethnicity.
There is no significant correlation between body mass index (BMI) and the pharmacokinetics of exenatide. No dose adjustment for BMI is required.
Indications
Indications
Monotherapy: type 2 diabetes as monotherapy in addition to diet and exercise to achieve adequate glycemic control.
Combination therapy: type 2 diabetes as adjunctive therapy to metformin, a sulfonylurea derivative, thiazolidinedione, a combination of metformin and a sulfonylurea derivative, or metformin and thiazolidinedione if adequate glycemic control is not achieved.
Active ingredient
Active ingredient
Composition
Composition
1 ml of solution for subcutaneous injection contains:
active ingredient:
exenatide 250 mcg,
excipients:
sodium acetate trihydrate,
glacial acetic acid,
/p>
Mannitol,
Methacresol,
Injection water
How to take, the dosage
How to take, the dosage
Subcutaneously, into the thigh, abdomen, or forearm.
The starting dose is 5 mcg administered 2 times/day at any time during a 60-minute period before a morning and evening meal. The drug should not be administered after a meal. In case of missing an injection of the drug the treatment is continued without changing the dose.
In 1 month after the start of treatment the dose of the drug can be increased to 10 mcg 2 times per day.
When co-administered with metformin, thiazolidinedione or a combination of these drugs, the initial dose of metformin and/or thiazolidinedione may not be changed. If Baeta is combined with sulfonylurea derivatives, a dose reduction of the sulfonylurea derivative may be required to reduce the risk of hypoglycemia.
Interaction
Interaction
The drug Baeta should be used with caution in patients taking oral drugs that require rapid absorption from the gastrointestinal tract, because Baeta may cause delayed gastric emptying. Patients should be advised to take oral medications whose effect depends on their threshold concentration (e.g., antibiotics) at least 1 h before exenatide administration. If such drugs must be taken with food, they should be taken during those meals when exenatide is not administered.
The concomitant administration of digoxin (at a dose of 0.25 mg once daily) with Baeta decreases the Cmax of digoxin by 17% and increases the Tmax by 2.5 hours. However, the overall pharmacokinetic effect at equilibrium is not altered.
The AUC and Cmax of lovastatin decreased by approximately 40 and 28%, respectively, and the Tmax increased by approximately 4 hours on administration of Baeta.
The co-administration of Baetal with HMG-CoA reductase inhibitors was not accompanied by changes in blood lipid composition (HDL-cholesterol, LDL-cholesterol, total cholesterol and triglycerides).
In patients with mild to moderate arterial hypertension stabilized by lisinopril (5-20 mg/day), Baeta did not alter the AUC and Cmax of lisinopril at equilibrium. Tmax of lisinopril at equilibrium was increased by 2 hours. There were no changes in mean daily MAP and DAP.
It was noted that when warfarin was administered 30 minutes after Baeta, the Tmah increased by approximately 2 hours. No clinically significant changes in Cmax and AUC were observed.
The use of Baetal in combination with insulin, D-phenylalanine derivatives, meglitinides or alpha-glucosidase inhibitors has not been studied.
Special Instructions
Special Instructions
Intravenous or intramuscular administration is not recommended.
Baet should not be used if particles are found in the solution or if the solution is cloudy or stained.
An antibody to exenatide may appear on therapy with Baetal. However, this does not affect the frequency and types of side effects reported.
Patients should be informed that treatment with Baeta may result in decreased appetite and/or body weight and that there is no need to change the dosing regimen because of these effects.
Patients should read the “Syringe Pen Guide” included with the drug before starting treatment with Baeta.
Contraindications
Contraindications
Side effects
Side effects
Adverse reactions that occurred more frequently than occasional are listed according to the following gradation: very common – â¥10%, common – â¥1%, but
Digestive system disorders: very often – nausea, vomiting, diarrhea; often – decreased appetite, dyspepsia, gastroesophageal reflux; sometimes – abdominal pain, abdominal bloating, belching, constipation, impaired taste sensation, flatulence.
CNS disorders: frequently – dizziness, headache; rarely – somnolence.
Endocrine system disorders: very often – hypoglycemia (in combination with sulfonylurea derivatives); often – trembling sensation, weakness, hyperhidrosis.
Allergic reactions: rarely – rash, itching, angioedema; extremely rare – anaphylactic reaction.
Others: often – skin reaction at the injection site; rarely – dehydration (associated with nausea, vomiting and/or diarrhea). Several cases of increased clotting time (INR) have been reported with concomitant use of warfarin and exenatide, which was sometimes accompanied by bleeding.
In view of the fact that the incidence of hypoglycemia increases when coadministering Baeta with sulfonylurea derivatives, it is necessary to consider reducing the dose of sulfonylurea derivatives when the risk of hypoglycemia increases. Most episodes of hypoglycemia were mild to moderate in intensity and were managed with oral carbohydrate intake.
In general, side effects were mild to moderate in intensity and did not lead to treatment withdrawal. Most commonly, reported nausea of mild to moderate intensity was dose-dependent and decreased over time without interfering with activities of daily living.
Overdose
Overdose
Symptoms:Serious nausea and vomiting, and rapid development of hypoglycemia (if the dose is 10 times the maximum recommended).
Treatment: conduct symptomatic therapy, including parenteral glucose administration in cases of severe hypoglycemia.
Pregnancy use
Pregnancy use
The drug is contraindicated in pregnancy and during breastfeeding.
Additional information
| Weight | 0.082 kg |
|---|---|
| Shelf life | 2 years |
| Conditions of storage | In the dark place at 2-8 °C (do not freeze) |
| Manufacturer | Baxter Pharmaceutical Solutions LLC, USA |
| Medication form | solution |
| Brand | Baxter Pharmaceutical Solutions LLC |
Related products
Buy Baeta, 250 µg/ml 2.4ml syringe pen cartridges with delivery to USA, UK, Europe and over 120 other countries.