No products in the cart.
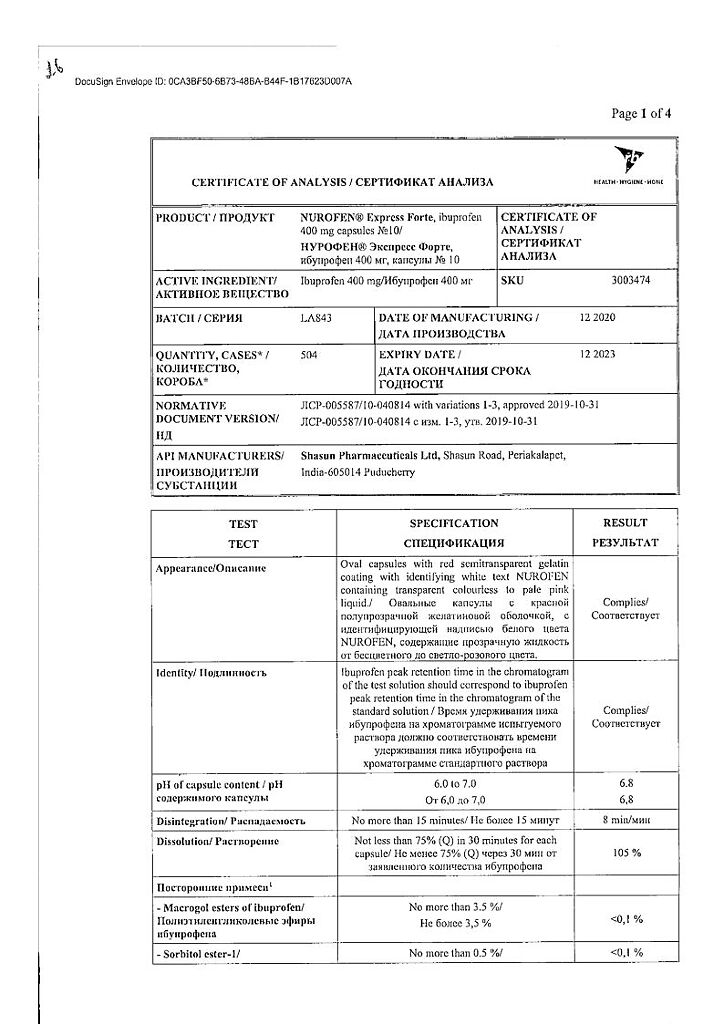
Nurofen Express Forte, 400 mg capsules 10 pcs
€5.79 €5.15
Description
The double-concentrated liquid active ingredient capsule (400 mg ibuprofen)*** works directly at the source of pain to help relieve it.
The mechanism of action of ibuprofen, a propionic acid derivative of the nonsteroidal anti-inflammatory drugs (NSAIDs), is due to inhibiting the synthesis of prostaglandins, mediators of pain, inflammation and hyperthermia.
Inhibits cyclooxygenase-1 (COX-1) and cyclooxygenase-2 (COX-2) indiscriminately, thus inhibiting the synthesis of prostaglandins. It has a fast directed action against pain (analgesic), antipyretic and anti-inflammatory effect. In addition, ibuprofen reversibly inhibits platelet aggregation.
Pharmacokinetics
Absorption is high, quickly and almost completely absorbed from the gastrointestinal tract (GIT). After drug intake on an empty stomach, ibuprofen is detected in blood plasma within 15 minutes, maximum concentration (Cmax) of ibuprofen in plasma is reached after 30-40 minutes, which is twice as fast as after taking the equivalent dose of the drug Nurofen®, in dosage form of 200 mg coated tablets.
Ingestion of the drug with food may increase the time to reach maximum concentration (TCmax). The binding to plasma proteins is more than 90%, the half-life (T1/2) is 2 hours. Slowly penetrates into the joint cavity, stays in synovial fluid, creating higher concentrations in it than in blood plasma. After absorption, about 60% of the pharmacologically inactive R-form is slowly transformed into the active S-form. It is metabolized in the liver. It is excreted by kidneys (not more than 1% unchanged) and, to a lesser extent, with bile.
There were no significant differences in pharmacokinetic profile of the drug in elderly people compared to younger people.
In limited studies, ibuprofen was detected in very low concentrations in breast milk.
Indications
Indications
Sore throat, Pain after injuries and operations, Fever, Back pain, Pain, Headache, Toothache, Rheumatoid arthritis, Joint pain (arthralgia). Nurofen® Express Forte is used for headache, migraine, toothache, painful menstruation, neuralgia, back pain, muscle and rheumatic pain; febrile conditions with flu and colds.
.
Active ingredient
Active ingredient
Ibuprofen
Composition
Composition
One capsule contains the active substance – ibuprofen 400 mg,
excipients:
macrogol-600 335.3 mg,
potassium hydroxide 44.82 mg,
Water 29.88 mg;
Capsule shell:
gelatin 197 mg,
sorbitol (partially dehydrated) 95.68 mg,
water 25.02 mg,
Crimson dye [Ponceau 4R] (E124) 0.79 mg,
Ink white [Opacode WB NS-78-18011] (water 48%, titanium dioxide (E171) 29%, propylene glycol 10%, isopropanol 8%, hypromellose 3cP 5%).
How to take, the dosage
How to take, the dosage
Read the instructions carefully before taking this medicine.
To be taken orally. For short-term use only.
Adults and children over 12 years: Orally take 1 capsule without chewing. The capsule should be taken with water. The interval between doses of the drug should be at least 4 hours. Maximal daily dose is 1200 mg. The maximum daily dose for children 12-17 years old is 800 mg.
If symptoms persist or worsen when taking the drug for 2-3 days, you should stop treatment and see a doctor.
Interaction
Interaction
The concomitant use of ibuprofen with the following drugs should be avoided:
– Acetylsalicylic acid: except in low doses of acetylsalicylic acid (no more than 75 mg per day) prescribed by a physician, because co-administration may increase the risk of side effects.
When used concomitantly, ibuprofen decreases the anti-inflammatory and antiplatelet effects of acetylsalicylic acid (increased incidence of acute coronary failure is possible in patients receiving low-dose acetylsalicylic acid as an antiplatelet after starting ibuprofen).
– Other NSAIDs, including selective cyclooxygenase-2 inhibitors: concomitant use of two or more drugs from the NSAID group should be avoided because of possible increased risk of side effects.
Cautiously use concomitantly with the following drugs:
– Anticoagulants and thrombolytics: NSAIDs may increase the effect of anticoagulants, particularly warfarin and thrombolytics.
Hypotensive drugs (ACE inhibitors and angiotensin II antagonists) and diuretics: NSAIDs may reduce the effectiveness of drugs in these groups. Diuretics may increase nephrotoxicity of NSAIDs.
– Glucocorticosteroids: increased risk of gastrointestinal ulcers and gastrointestinal bleeding.
– Antiaggregants and selective serotonin reuptake inhibitors: increased risk of gastrointestinal bleeding.
– Cardiac glycosides: Concomitant use of NSAIDs and cardiac glycosides may worsen heart failure, decrease glomerular filtration rate, and increase plasma concentrations of cardiac glycosides.
Lithium drugs: there is data on the likelihood of increased plasma lithium concentrations with NSAIDs.
– Methotrexate: there is data on the likelihood of increased plasma concentrations of methotrexate with NSAIDs.
– Cyclosporine: increased risk of nephrotoxicity with concomitant use of NSAIDs and cyclosporine
– Mifepristone: NSAIDs should not be started earlier than 8-12 days after mifepristone is finished, because NSAIDs may decrease the effectiveness of mifepristone.
– Tacrolimus: simultaneous use of NSAIDs and tacrolimus may increase the risk of nephrotoxicity.
– Zidovudine: concomitant use of NSAIDs and zidovudine may increase hematotoxicity. There is evidence of an increased risk of hemarthrosis and hematomas in HIV-positive patients with hemophilia co-treated with zidovudine and ibuprofen.
– Quinolone antibiotics: patients co-treated with NSAIDs and quinolone antibiotics may have an increased risk of seizures.
Special Instructions
Special Instructions
It is recommended that the drug be taken in as short a course as possible and in the minimum effective dose necessary to eliminate symptoms. During long-term treatment it is necessary to monitor the peripheral blood picture and the functional state of the liver and kidneys.
In case of gastropathy symptoms a careful control is indicated, including esophagogastroduodenoscopy, general blood test (hemoglobin determination), fecal occult blood test. If it is necessary to determine 17-ketosteroids, the drug should be cancelled 48 hours before the study. During the treatment period it is not recommended to take ethanol.
Patients with renal insufficiency should consult a physician before using the drug, since there is a risk of impairment of renal function.
Patients with arterial hypertension, including a history of and/or chronic heart failure, should consult a physician before using the drug, as the drug may cause fluid retention, increased blood pressure, and edema. Information for women planning pregnancy: the drug inhibits cyclooxygenase and prostaglandin synthesis and may affect ovulation, disrupting female reproductive function (reversible after treatment withdrawal).
Influence on driving, operating machinery
Patients who experience dizziness, drowsiness, lethargy or visual disturbances while taking ibuprofen should avoid driving or operating machinery.
Contraindications
Contraindications
- Hypersensitivity to ibuprofen or any of the ingredients of the drug.
- Complete or incomplete combination of bronchial asthma, recurrent polyposis of the nose and sinuses, and intolerance to acetylsalicylic acid or other non-steroidal anti-inflammatory drugs (including history).
- Erotic ulcerative diseases of the gastrointestinal tract (including gastric and duodenal ulcer, Crohn’s disease, ulcerative colitis) or ulcer bleeding in the active phase or in the history (two or more confirmed episodes of peptic ulcer disease or ulcer bleeding).
- Bleeding or gastrointestinal ulcer perforation in history triggered by use of NSAIDs.
- Severe hepatic impairment or active liver disease.
- Severe renal impairment (creatinine clearance < 30 ml/min), confirmed hyperkalemia.
- Decompensated heart failure; period after coronary artery bypass.
- Cerebrovascular or other bleeding.
- Hemophilia and other bleeding disorders (including hypocoagulation), hemorrhagic diathesis.
- Fructose intolerance.
- Pregnancy (III trimester).
- Children under 12 years.
Cautions
If you have any of the conditions listed in this section, please consult your doctor before using the drug.
Concurrent use of other NSAIDs, history of single episode peptic ulcer disease or peptic ulcer bleeding;
gastritis, enteritis, colitis, presence of Helicobacter pylori infection, ulcerative colitis;
Bronchial asthma or history of allergic conditions with exacerbation or history of bronchospasm;
systemic lupus erythematosus or mixed connective tissue disease (Sharp’s syndrome) – increased risk of aseptic meningitis;
renal failure including dehydration (creatinine clearance 30-60 ml/min), nephrotic syndrome;
Hepatic failure, cirrhosis with portal hypertension, hyperbilirubinemia, arterial hypertension and/or heart failure, cerebrovascular disease;
Blood diseases of unclear etiology (leukopenia and anemia), severe somatic diseases, dyslipidemia/hyperlipidemia, diabetes, peripheral artery disease;
smoking;
frequent alcohol consumption;
concomitant use of medications that may increase the risk of ulceration or bleeding, particularly oral glucocorticosteroids (including prednisolone), anticoagulants (including warfarin), antiaggregants (including acetylsalicylic acid, clopidogrel), selective serotonin reuptake inhibitors (including citalopram, fluoxetine, paroxetine, sertraline);
pregnancy I-II trimester, breastfeeding, advanced age.
.
Side effects
Side effects
The risk of side effects can be minimized by taking the drug in a short course at the lowest effective dose necessary to control symptoms.
The side effects are mostly dose-dependent. The following adverse reactions have been reported with short-term administration of ibuprofen in doses not exceeding 1200 mg/day (3 capsules). When treating chronic conditions and with long-term use, other adverse reactions may occur.
The incidence of adverse reactions has been evaluated based on the following criteria: Very common (> 1/10), common (> 1/100 to < 1/10), infrequent (> 1/1000 to < 1/100), rare (> 1/10 000 to < 1/1000), very rare (< 1/10 000), frequency unknown (no data on frequency estimates).
Blood and lymphatic system disorders
- Very rare: hematopoiesis disorders (anemia, leukopenia, aplastic anemia, hemolytic anemia, thrombocytopenia, pancytopenia, agranulocytosis).
The first symptoms of these disorders are fever, sore throat, superficial mouth ulcers, flu-like symptoms, marked weakness, nosebleeds and subcutaneous hemorrhages, bleeding and bruising of unknown etiology.
Immune system disorders
- Infrequent: hypersensitivity reactions – non-specific allergic reactions and anaphylactic reactions, respiratory reactions (bronchial asthma, including its exacerbation, bronchospasm, shortness of breath), skin reactions (itching, urticaria, purpura, Quincke’s edema, exfoliative and bullous dermatoses, including toxic epidermal necrolysis (Lyell’s syndrome), Stevens-Johnson syndrome, erythema multiforme), allergic rhinitis, eosinophilia.
- very rarely: severe hypersensitivity reactions, including swelling of the face, tongue and throat, shortness of breath, tachycardia, arterial hypotension (anaphylaxis, Quincke’s edema or severe anaphylactic shock).
Gastrointestinal disorders
- Infrequent: abdominal pain, nausea, dyspepsia (including heartburn, bloating).
- Seldom: diarrhea, flatulence, constipation, vomiting.
- Very rare: peptic ulcer, perforation or gastrointestinal bleeding, melena, bloody vomiting, in some cases with fatal outcome, especially in elderly patients, ulcerative stomatitis, gastritis.
- Frequency unknown: exacerbation of colitis and Crohn’s disease.
Hepatic and biliary tract disorders
- Very rare: hepatic dysfunction (especially with long-term use), hepatitis, jaundice.
Renal and urinary system disorders
- Very rare: acute renal failure, hematuria and proteinuria, nephritic syndrome, nephrotic syndrome, papillary necrosis, interstitial nephritis, cystitis.
Nervous system disorders
- Infrequent: headache.
- Very rare: aseptic meningitis (single cases of symptoms of aseptic meningitis, such as neck stiffness, headache, nausea, vomiting, fever, and loss of orientation, have been observed with ibuprofen treatment in patients with autoimmune diseases (systemic lupus erythematosus and mixed connective tissue disease).
Cardiovascular disorders
- Frequency unknown: heart failure, peripheral edema, increased risk of thrombotic complications (such as myocardial infarction or stroke) with long-term use, increased blood pressure.
Respiratory, chest and mediastinal disorders
- Frequency unknown: bronchial asthma, bronchospasm, shortness of breath.
Laboratory indices
- hematocrit or hemoglobin (may decrease)
- bleeding time (may increase)
- plasma glucose concentration (may decrease)
- creatinine clearance (may decrease)
- plasma creatinine concentration (may increase)
- hepatic transaminase activity (may increase)
If side effects occur, discontinue use and seek medical attention.
.
Overdose
Overdose
The use of the drug in children at a dose of 400 mg/kg may lead to symptoms of intoxication. In adults the dose effect is less pronounced. The half-life in overdose is 1.5-3 hours.
Symptoms.
The majority of patients who have used clinically significant amounts of NSAIDs have only developed nausea, vomiting, epigastric pain or very rarely diarrhea. Tinnitus, headache, and gastrointestinal bleeding may also occur.
In more severe poisoning, toxic lesions of the central nervous system may occur, which are manifested as vertigo, drowsiness, sometimes – agitation and disorientation or coma.
Sometimes patients experience seizures. In severe poisoning hyperkalemia and metabolic acidosis may develop, increased prothrombin time / increased prothrombin index may be observed, possibly as a result of effects on circulating blood clotting factors. Acute renal failure, liver damage, arterial hypotension, respiratory failure and cyanosis may develop.
In patients with bronchial asthma, exacerbation of the course of the disease is possible.
Treatment.
Treatment should be symptomatic and supportive, and should include ensuring airway patency and monitoring cardiac performance and vital functions until normalization.
The oral administration of activated charcoal or gastric lavage within 1:00 of a potentially toxic dose of the drug is recommended.If ibuprofen has already been absorbed into the body, alkaline agents can be administered to speed the excretion of acidic ibuprofen with the urine.
In frequent or prolonged seizures, diazepam or lorazepam should be used intravenously. Bronchodilators should be used to treat exacerbations of bronchial asthma.
Pregnancy use
Pregnancy use
The drug is contraindicated in the third trimester of pregnancy. The use of ibuprofen in I-II trimesters of pregnancy should be avoided, if it is necessary to take the drug should be consulted with a physician.
There is evidence that ibuprofen in small amounts may penetrate into breast milk without any adverse effects on the health of the infant, therefore in case of short-term use it is not necessary to stop breast-feeding.
If long-term use of the drug is necessary, consult a physician to decide on stopping breastfeeding for the period of application of the drug.
Similarities
Similarities
Nurofen, Nurofen Express, Brufen, Ibuprofen, Dolgit, Ibuprofen-Chemopharm, Nurofen Forte, MIG 400, Faspik, Nurofen Express Lady, Nurofen Express Forte, Nurofen Children, Next Uno Express, Nurofast
Additional information
| Weight | 0.025 kg |
|---|---|
| Shelf life | 3 years. Do not use after the date on the package. |
| Conditions of storage | In a dry place at a temperature not exceeding 25 ° C. |
| Manufacturer | Reckitt Benckiser Healthcare International Ltd, United Kingdom |
| Medication form | capsules |
| Brand | Reckitt Benckiser Healthcare International Ltd |
Other forms…
Related products
Buy Nurofen Express Forte, 400 mg capsules 10 pcs with delivery to USA, UK, Europe and over 120 other countries.