No products in the cart.
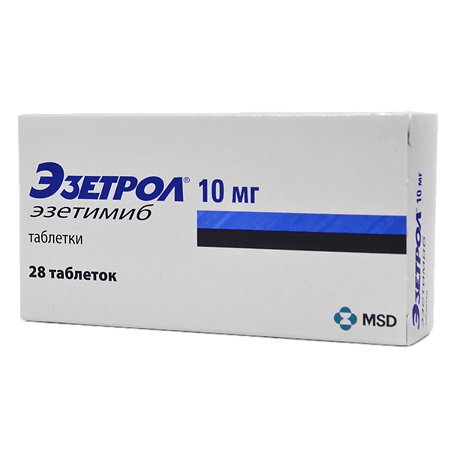
Ezetrol, tablets 10 mg 28 pcs
€104.43 €87.03
Description
EZETROL is a selective representative of a new class of hypolipidemic drugs that reduce absorption of cholesterol (CHL) in the intestine, including CHL of vegetable fats.
The mechanism of action of EZETROL differs from the mechanism of action of other classes of hypolipidemic drugs (e.g., statins, bile acid sequestrants, fibrates). Unlike bile acid sequestrants, Ezetimibe does not increase bile acid excretion and does not inhibit CL synthesis in the liver unlike statins.
On entry into the small intestine, Ezetimibe localizes at the brush border of the small intestine and slows down absorption of CHL, which leads to a decrease in the entry of CHL from the intestine into the liver.
After 2 weeks of use, EZETROL reduces intestinal ChL absorption by 54% compared to placebo.
Pharmacokinetics
.
Indications
Indications
Prevention of heart attacks and strokes – increased blood cholesterol;
– coronary heart disease;
– atherosclerosis.
Active ingredient
Active ingredient
Ezetimibe
Composition
Composition
1 tablet contains:
Active substance:
ezetimibe 10 mg;
Associates:
croscarmellose sodium;
lactose monohydrate;
magnesium stearate;
microcrystalline cellulose;
povidone;
sodium lauryl sulfate.
How to take, the dosage
How to take, the dosage
Ingestion, at any time of the day, regardless of meals.
Patients should switch to an appropriate lipid-lowering diet before starting treatment and continue this diet for the duration of Ezetrol therapy®.
The recommended dose of Ezetrolol in monotherapy or in combination with a statin is 10 mg once daily.
There is no need to adjust doses in elderly patients (see “Pharmacokinetics”).
In hepatic failure
Dose adjustment for patients with mild hepatic failure (5-6 points on the Child-Pugh scale) is not required. Treatment with ezetimibe is not recommended for patients with moderate (7-9 Child-Pugh scores) and severe (greater than 9 Child-Pugh scores) hepatic dysfunction (see “Pharmacokinetics” and “Contraindications”).
In renal failure
There is no need to adjust doses for patients with impaired renal function (see “Pharmacokinetics”).
In concomitant therapy with fatty acid sequestrants
Esetrol should be taken at a dose of 10 mg once daily no later than 2 hours before or no earlier than 4 hours after taking fatty acid sequestrants.
Interaction
Interaction
In preclinical studies it was shown that ezetimibe does not induce cytochrome P450 enzymes involved in drug metabolism. No clinically significant pharmacokinetic interactions were observed between ezetimibe and agents metabolized by cytochrome P450 1A2, 2D6, 2C8, 2C9 and ZA4 or N-acetyltransferase.
Ezetimibe has no effect on the pharmacokinetics of dapsone, dextromethorphan, digoxin, oral contraceptives (ethinylestradiol and levonorgestrel), glipizide, tolbutamide, midazolam and warfarin when taken simultaneously. Concomitant administration of cimetidine with ezetimibe has no effect on the bioavailability of ezetimibe.
Antacids: Concomitant administration decreases the rate of absorption of ezetimibe, but has no effect on its bioavailability. This decrease in absorption rate is not considered clinically significant.
Cholestyramine: Concurrent administration reduces the mean AUC of total ezetimibe (ezetimibe + ezetimibe glucuronide) by approximately 55%. Additional reductions in LDL cholesterol levels due to the addition of ezetimibe to cholestyramine may be reduced by this interaction.
Cyclosporine: In kidney transplant patients with Cl creatinine >50 ml/min receiving cyclosporine at a constant dose, a single dose of Ezetrol at 10 mg resulted in an average 3.4-fold increase in AUC of Ezetrol (2.3 to 7.9-fold). In one patient after kidney transplantation and with severe renal insufficiency (creatinine Cl 13.2 ml/min/1.73 m2) who received complex therapy including cyclosporine there was 12-fold increase of Ezetrol levels compared to control group. In 12 healthy volunteers who received ezetimibe at a dose of 20 mg daily for 8 days concomitantly with cyclosporine at a dose of 100 mg daily on day 7, an increase in the AUC of cyclosporine by an average of 15% (from a decrease of 10% to an increase of 51%) was found compared with patients in whom cyclosporine was used in monotherapy at a dose of 100 mg/day.
Fibrates:Concomitant administration of fenofibrate or gemfibrozil increases total ezetimibe concentrations by approximately 1.5 and 1.7-fold, respectively. However, these increases are not considered clinically significant.
The safety and efficacy of ezetimibe in combination with fibrates has not been established. Fibrates may increase cholesterol excretion with bile, which can lead to cholelithiasis. In a preclinical study in dogs, ezetimibe increased gallbladder cholesterol levels. Although the significance of these findings in humans is unknown, concomitant administration of ezetimibe with fibrates prior to clinical trials is not recommended.
Statins: No clinically significant pharmacokinetic interactions have been observed with ezetimibe concomitantly administered with atorvastatin, lovastatin, pravastatin, simvastatin, fluvastatin and rosuvastatin.
Special Instructions
Special Instructions
Patients should switch to an appropriate lipid-lowering diet before starting treatment and continue this diet for the duration of therapy with Ezetrol.
If Ezetrol is prescribed in combination with a statin, carefully read the instructions for medical use of the particular statin.
Liver enzymes
In controlled clinical studies with concomitant administration of Ezetrol and statins, patients showed increased liver enzymes (3 times the upper limit of normal). If Ezetrol is prescribed in combination with a statin, liver function monitoring should be performed at the beginning of treatment and further in accordance with the recommendations for this statin.
Skeletal musculature
In clinical trials, the incidence of myopathy or rhabdomyolysis associated with the use of Ezetrol was not greater than that of the respective control group (placebo or statin). However, myopathy and rhabdomyolysis are known adverse reactions of statins and other lipid-lowering drugs. In clinical trials, the incidence of an increase in CPK activity of more than 10 times the GFR was 0.2% in the Ezetrol group compared with 0.1% in the placebo group, and 0.1% in the Ezetrol with statin combination group compared with 0.4% in the statin monotherapy group.
Hepatic impairment
Because the effects of doses of ezetimibe greater than 10 mg in patients with moderate to severe hepatic impairment have not been studied, Ezetrol is not recommended in these patients.
Fibrates
The safety and effectiveness of prescribing ezetimibe in combination with fibrates has not been established. Therefore, concomitant administration of ezetrol and fibrates is not recommended.
Cyclosporine
Cautions should be taken when prescribing ezetimibe to patients receiving cyclosporine. Cyclosporine concentrations should be monitored when concomitant administration of Ezetrol and cyclosporine.
Contraindications
Contraindications
– Moderate (7-9 points on the Child-Pugh scale) and severe (over 9 points on the Child-Pugh scale) degree of liver failure;
– Lactose intolerance, lactase deficiency or glucose/galactose malabsorption syndrome;
– Children under 18 years old;
– Hypersensitivity to any of the drug components.
When prescribing Ezetrol in combination with a statin to control contraindications it is necessary to follow the instructions for use of the prescribed statin.
The drug should be administered with caution in patients receiving cyclosporine; concomitant use with fibrates is not recommended until additional data are available from clinical studies.
Side effects
Side effects
In clinical studies of 8 to 14 weeks in which 3366 patients were enrolled, Ezetrol, administered at a dose of 10 mg daily in monotherapy or in combination with a statin, showed good tolerability.
The adverse effects were generally mild and transient; the overall adverse effect rate and the rate of treatment withdrawal due to adverse effects with Ezetrolone were different from those with placebo.
In patients taking Ezetrolone in monotherapy (n=5691) or in combination with statin (n=1675), the most common (≥1/100,
Mototherapy with Ezetimibe: headache, abdominal pain, diarrhea.
Combination therapy with statin: headache, fatigue, abdominal pain, constipation, diarrhea, abdominal bloating, nausea, increased ALT and ACT, myalgia.
Laboratory measures: the incidence of clinically significant elevation of serum ALT and/or ACT enzymes 3 or more times the upper limit of normal (ULN) was similar with administration of Ezetrol in monotherapy (0.5%) and placebo (0.3%).
In a study of the safety of combination therapy, the incidence of clinically significant increases in serum enzymes was 1.3% in patients taking Ezetrol in combination with statins and 0.4% in patients taking statins in monotherapy.
The increase in serum enzymes was usually asymptomatic, was not accompanied by the occurrence of cholestasis and went away both with continuation of treatment and after discontinuation of the drug.
The incidence of a clinically significant increase in creatine phosphokinase (CPK – ≥10×VGN) in patients treated with Ezetrol monotherapy was similar to that in patients treated with placebo or statin monotherapy.
Clinical experience of use
The following adverse reactions have been reported with Ezetrol in clinical practice: Hypersensitivity reactions, including angioneurotic edema and skin rash; myalgia; increased CPK, liver enzymes, hepatitis, thrombocytopenia, pancreatitis, nausea. Very rare – myopathy/rhabdomyolysis.
Overdose
Overdose
Symptoms: Several cases of overdose have been reported, most of which were without adverse events and, if they did occur, adverse events were not serious.
In clinical trials, one in which ezetimibe was administered to 15 healthy volunteers at a dose of 50 mg daily for 14 days and another to 18 patients with primary hypercholesterolemia at a dose of 40 mg daily for 56 days, good tolerability of the drug was demonstrated.
Treatment: Symptomatic and maintenance therapy.
Pregnancy use
Pregnancy use
Animal studies with administration of ezetimibe have shown no direct or indirect adverse effects on pregnancy, embryo/fetal development, labor and postnatal development. No teratogenic effects were observed when ezetimibe was administered to pregnant rats in combination with lovastatin, simvastatin, pravastatin, or atorvastatin. When administered to pregnant rabbits, fetal skeletal development defects were observed with low frequency.
There are no clinical data on the use of the drug Ezetrol during pregnancy. Therefore, the use of the drug Ezetrol during pregnancy is not recommended. In case of pregnancy, the use of the drug Ezetrol should be discontinued.
In studies on rats it was found that ezetimibe is excreted with breast milk. There are no data on excretion of ezetimibe with breast milk in women. In this regard, Ezetrol is not recommended to use in breastfeeding mothers. If the use of the drug is necessary, the patient should stop breastfeeding.
Similarities
Similarities
Otrio, Lipobon
Additional information
| Weight | 0.012 kg |
|---|---|
| Shelf life | 2 years |
| Conditions of storage | At a temperature not exceeding 30 °C |
| Manufacturer | MSD International GmbH (Puerto Rico Branch) LLC, Puerto Rico |
| Medication form | pills |
| Brand | MSD International GmbH (Puerto Rico Branch) LLC |
Related products
Buy Ezetrol, tablets 10 mg 28 pcs with delivery to USA, UK, Europe and over 120 other countries.